Study finds 79% of Canadians support the therapeutic use of psilocybin for people at the end of life
by Laval University – January 23, 2024
Nearly 4 out of 5 Canadians believe that the use of psilocybin, the active ingredient in hallucinogenic mushrooms, is an acceptable medical approach to treat existential distress in patients suffering from a serious and incurable disease. This is the main conclusion of an online survey of 2,800 people conducted by a research team led by Michel Dorval, professor at Université Laval’s Faculty of Pharmacy and researcher at the CHU de Québec-Université Laval Research Center. The results have been published in the journal Palliative Medicine.
Canadian law currently prohibits the production, sale or possession of psilocybin. Since January 2022, however, a special access program has made it possible to obtain an exemption from Health Canada for medical or scientific reasons. A doctor can apply on behalf of a patient if psychotherapy, antidepressants or anxiolytics have failed, or if the patient’s condition requires urgent intervention.
Researchers surveyed 1,000 residents of Québec and 1,800 residents of Ontario, Alberta and British Columbia to find out their opinion on the potential easing of rules surrounding the medical use of psilocybin. Analysis of their answers shows that 79% of respondents consider psilocybin-assisted therapy a reasonable medical choice to treat existential distress in patients at the end of life.
“Our results seem to indicate that the social acceptability of this intervention is high in the Canadian population,” comments Professor Dorval. “If we consider only Québec respondents, the acceptability rate is similar to the national average.”
Support for psilocybin is higher among respondents who have already been exposed to palliative care. “Having been close to loved ones at the END OF LIFE, or having witnessed their distress, could explain this openness to new approaches designed to help people at this stage of their life,” suggests Dorval.
Support is also higher among respondents who have already used PSILOCYBIN. “There are still many prejudices against PSYCHEDELIC SUBSTANCES, says the researcher. Familiarity with these substances probably helps to better understand their true effects as well as their therapeutic potential.”
This study was carried out as part of Louis Plourde’s doctoral research at Université Laval’s Faculty of Pharmacy. Researchers from McGill University, Université de Montréal and UQAR co-authored the article published in Palliative Medicine.
Article from – Laval University
Magic mushrooms are following a path well-trodden by cannabis
André Picard – Health Columnist
Last week, Vancouver police raided three stores that have been openly selling “magic mushrooms” and other psychedelic drugs for years.
In recent months, similar raids have happened across the country, mostly at mushroom dispensaries with names like Fun Guyz and Shroomyz, in Montreal, Toronto, Hamilton and elsewhere.
Yet, nothing much ever comes of these raids and the stores continue to operate and proliferate.
It all has an early 1990s feel to it, when owners of “medicinal cannabis” shops openly defied police and mounted legal challenges to archaic drug laws.
In 2000, Ontario’s top court ruled on the case of Terrance Parker, who used cannabis to control his epilepsy, saying that it was unconstitutional for him to have to choose between his health and imprisonment. Shortly after, the federal government formally regulated the use of medical cannabis. Years of widespread public acceptance led to the legalization of recreational cannabis in 2018.
Will history repeat itself? Will psychedelic drugs like psilocybin eventually be legalized?
Probably. And it’s a shame we’re going to waste countless police and court resources to get there when policy-makers and politicians could instead be proactive.
Prohibition has never worked, and it never will.
The Supreme Court has also made it abundantly clear that, under Canada’s Charter of Rights of Freedoms, individuals have pretty broad leeway to a) put whatever substances they want into their bodies, and b) that access to care must be straightforward and equitable.
The learned justices said so when they struck down unduly restrictive prohibitions to medical cannabis and to medical assistance in dying. And they would almost certainly say so if we continue to restrict access to psychedelics for people who find them helpful to treat conditions like depression and post-traumatic stress disorder.
Like medical cannabis, the evidence for the benefits of psychedelics is not especially strong, but the potential harms are also minimal. If benefits outweigh harms, what justification is there for denying access to patients?
To date, the response of governments to psychedelics has mirrored that to medical cannabis – creating bureaucratic hurdles. Health Canada has allowed some patients to buy the drugs legally, either by applying for a personal exemption (few of which are granted) or by requesting “special access” via their physician.
But most people who want to self-medicate with magic mushrooms can’t be bothered with onerous paperwork and intrusive scrutiny. Hence the popularity of dispensaries.
Health Canada has also approved about two dozen clinical trials. But it has blocked many more researchers from studying the popular drugs, creating frustration.
Meanwhile, as with cannabis, the public relations war is being won, hands-down, by activists. They have powerful anecdotal stories about the benefits of psychedelics, often told by military veterans with war wounds like PTSD.
Investors are also salivating about the possibilities, with the market for psychedelics estimated at US$7-billion by 2027, according to Data Bridge Market Research. Every hip venture capitalist is betting big on ‘shrooms.
The danger is that, like cannabis, we see an orgy of get-rich-quick ventures, and patients get trampled in the capitalist stampede. We’re already seeing a flurry of clinics making outrageous claims and offering dubious psychedelic therapies. These clinics have the potential to do a lot more harm than storefronts selling microdosing kits to consumers who are generally quite well-informed.
Broader decriminalization of drugs is coming because the war on drugs has been an abject failure. But there will be some growing pains.
B.C. is in the midst of a three-year pilot project where anyone can possess up to 2.5 grams of opioids, cocaine, MDMA (ecstasy) or similar drugs. Trafficking, production and exportation of these drugs is still a crime. So far, the change seems to have made little difference, good or bad. No single measure will resolve the toxic drug crisis. But psychedelics are the least of our worries.
Where drug use is more public, governments have responded with restrictions on where drugs can be used – not near schools, daycares, playgrounds, splash pads, skateboard parks, and other places children congregate. That’s good policy.
Decriminalization shouldn’t be a free-for-all. We regulate where other drugs – alcohol, tobacco, cannabis – can be used; we should do the same with other drugs. We also need to make spaces available for safer drug use; proportionally, we need as many safe consumption sites as the population of drug users demands.
In the end, a drug is a drug is a drug. People should be free to use whatever drugs they choose. Public policy responses should focus on education and public safety, not stigmatization and criminalization.
Article from The Globe and Mail
Could magic mushrooms be an alternative to medical assistance in dying?
Advocates say psilocybin therapy is a viable alternative to MAID for some Canadians facing end-of-life despair or other mental struggles.
By Ben Mussett Staff Reporter – February 14, 2023
But that fear of dying vanished after Hughes, 66, tried psilocybin therapy, where a patient consumes psilocybin — the psychoactive ingredient in what are commonly known as “magic mushrooms” — under the supervision of a specially trained therapist.
“I am living more fully than I ever have in my life,” she said.
Although shops hawking magic mushrooms are popping up across Canada, the substance remains illegal. After starting to approve legal exemptions for dozens of terminally ill patients in 2020, critics say the federal government has since restricted access to the psychedelic treatment.
“I am just dismayed that my government would rather I live with the end-of-life anxiety, or just stop that entirely by taking MAID (medical assistance in dying),” said Hughes. “It feels cruel, thoughtless — just the opposite of empathetic.”
In an emailed statement, a spokesperson for the minister of Mental Health and Addictions said Tuesday that “Health Canada is aware of increasing interest in the potential therapeutic uses of psilocybin.
As Canadians debate whether those suffering from severe mental health challenges should be eligible for MAID, Hughes and other advocates view psilocybin therapy as a viable alternative for people facing end-of-life despair or other mental struggles.
Earlier this month, the federal government announced plans to delay an expansion of MAID that would include individuals suffering solely from mental health anguish by one year, to March 17, 2024.
At a news conference on Tuesday, Hughes and others, including MPs from the NDP and Green Party, called on the federal government to ease medical access to psilocybin therapy.
“We should never find ourselves in a situation where we’ve made it easier for a patient to access MAID than to access psilocybin,” said Green Party Leader Elizabeth May.
In the summer of 2020, Health Canada started approving psilocybin therapy for terminally ill patients through a Section 56(1) exemption of the Controlled Drugs and Substances Act. Patients could also access psilocybin therapy through a clinical trial, although they’re relatively rare in Canada.
Now, patients must find a doctor willing to apply to SAP to prescribe psilocybin to them. When Hughes explained to Health Canada that she couldn’t find a doctor who would, she was told to reapply for a Section 56 (1) exemption. She did, but said she hasn’t heard back.
This past summer, Hughes, along with six other patients and a health-care practitioner, filed a legal challenge against the Canadian government and federal minister of health, alleging that the inaccessibility of psilocybin therapy violated Section 7 of the Canadian Charter of Rights and Freedoms, which guarantees the right to life, liberty and security of the person.
Dr. Valorie Masuda, a palliative-care physician from B.C. who appeared in Ottawa on Tuesday, called psilocybin therapy a “valuable, essential tool for palliative care.”
Over the past couple of years, she said she’s treated close to 25 patients using this method, with a 75 to 80 per cent success rate in reducing existential distress, depression and anxiety.
However, this past summer, she said the SAP informed her she could no longer access psilocybin for her patients because, she alleges, she was “treating too many people.”
Story from The Toronto Star
Federal Court ruling sets back health workers seeking psilocybin mushroom access
VANCOUVER – Darryl Greer – The Canadian Press Sept. 30, 2023
Megan McLaren thought her future career was in law enforcement, but her path radically shifted thanks in part to psychedelic drug therapy, she says.
McLaren left a civilian position with the Vancouver Police Department in 2019 for a job in counselling with the Surrey School District and is now a registered clinical counsellor with a practice in Squamish, B.C.
When the pandemic hit and her position was cut from the school district, she began researching psychedelics, eventually signing up for a three-month group therapy program involving the use of ketamine in mid-2021.
Now, she and dozens of other health care professionals across the country are fighting the federal government in court for legal access to psychedelics, namely psilocybin mushrooms, in order to offer such therapeutic treatments in their practices.
Before they can offer patients these drug-assisted therapies though, doctors, psychologists, counsellors, and nurses want a special exemption from Canada’s Controlled Drugs and Substances Act.
The exemption would allow them to take magic mushrooms themselves in “experiential training” before they’re qualified to offer the treatments to patients.
“We’ve got people in Canada right now who are being approved for medical assistance in dying, and those same people are being unapproved for taking mushrooms,” McLaren said in an interview.
“We’re in a little bit of a backwards moment when Canada is more willing to end people’s lives than to give them a chance of surviving or dying with dignity, dying with less anxiety.”
McLaren is part of a group of more than 60 other health care professionals that applied this month to the Federal Court of Canada to overturn a decision denying them the needed exemptions.
A ruling in a nearly identical case filed in 2022 involving almost 100 other health care professionals was dismissed on Sept. 25 by a Federal Court judge who upheld the decision denying them the exemptions.
The judge found “there is insufficient evidence to demonstrate a need for, or benefit of, experiential training with psilocybin.”
“The evidence does not establish that psilocybin-assisted psychotherapy by an experientially trained practitioner is safer and more effective, and the decisions do not prevent patients from accessing psilocybin under their own exemption or accessing psilocybin-assisted psychotherapy,” the ruling says.
Ottawa-based human rights lawyer Nicholas Pope said Friday that he’ll be appealing the ruling all the way to the Supreme Court of Canada if necessary.
He said he’s confident that case law and precedents are on the side of both patients and health care workers seeking legal access to psilocybin mushrooms.
Pope said it’s a “unique situation” where case law related to pre-legalization cannabis litigation set the stage for legal battles involving mushrooms now.
“Here we have a safer substance, a substance that there’s more evidence for its efficacy and we have two decades of law (established) that says people have a right to access this, so it’s just a matter of time before we get these cases before the right courts,” he said.
Pope said it is an “absurd situation” where anyone can easily access psilocybin mushrooms from illegal dispensaries that have popped up across the country, while people with “serious and pressing medical issues and health concerns” are fighting for legal access.
“That’s why I’ve been taking on a lot of these cases and doing them pro bono because this is just something that needs to change,” he said.
Pope said a lawsuit filed on behalf of several patients in July 2022 is the most pivotal, challenging Canada’s prohibition on psilocybin as unconstitutional.
“That’s sort of the big glacial pace action that seeks to strike down the whole system,” he said.
Thomas Hartle, one of eight plaintiffs in that case, said in an interview in August that access to mushrooms isn’t necessarily the problem, but rather access to qualified therapists who can administer the treatment.
Diagnosed with colon cancer eight years ago, Hartle was one of the first people in the country allowed to consume mushrooms legally under what’s known as the special access program, but he had to fly to B.C. from his home in Saskatchewan to undergo the treatment.
Travelling anywhere is both physically and financially draining, he said, but with no qualified psilocybin therapists closer to home, he’s had to spend thousands on travel, food and accommodations to receive the therapy out of province.
Hartle said Friday that his stage four cancer is still progressing, but mushroom therapy sessions have been effective in lightening the end-of-life anxiety associated with it.
He said the lawsuit moves “like a glacier,” as he grapples with an uncertain future.
“I do kind of these days feel like the legal case will probably outlive me,” he said. “I am not at this time anticipating seeing a resolution to that. I would really like to, but the pace that things are going I don’t think that is a realistic expectation for me.”
Story from – BC CTV
Hamilton’s first magic mushroom store opens
Dispensary is pushing for legalization; police are investigating
By Ritika Dubey – Spectator Reporter
Tuesday, December 13, 2022
Hamilton’s first-ever psilocybin mushrooms store opened Monday on Main Street East.
Catching up on the trends on the West Coast, and more recently, Toronto, the Mushroom Cabinet is part of “the cause” — pushing to bring legal psychedelic reforms and reducing stigma around the substance, said Matthew Francis, the store’s spokesperson.
“We’re interested in pushing forward and getting into legalization,” he said.
Before the mushrooms store front took over, the location was a provincially licensed cannabis store, the city said.
Francis, a Hamiltonian who makes a living through standup comedy, compared the psilocybin mushrooms store to the illegal cannabis market before the legalization of the substance, calling it “a grey area.”
“I know it’s technically not a grey area,” he said, “but Health Canada is approving medicinal (psilocybin) and that’s how it happened with cannabis too. I see it being the same thing.”
For their part, Health Canada says, “At this time, there are no approved therapeutic products containing psilocybin in Canada.” Health Canada also contests Francis’ suggestion that cannabis followed a similar path, saying that therapeutic uses of cannabis were not approved before legalization.
In 2020, the federal Health Ministry started exempting some palliative patients with end-of-life distress to use medical psilocybin for treating their mental health. But since 2021, the process came to a halt leading some patients to later sue the minister of health over access to mushrooms.
Health Canada’s website lists mushrooms as illegal, but acknowledges “increasing interest” in therapeutic uses of the drug. Among risks, Health Canada lists “bad trips,” “flashbacks” and the potential for side effects when consumed with other substances.
He was also involved in unlicensed cannabis stores and dispensaries prior to the cannabis legalization, which later closed down after the substance was legalized. “That was the goal to get things legal. It wasn’t for money,” he said.
Hamilton police said they’re investigating the store after receiving a tip through the city’s Crime Stoppers earlier on Monday.
“Police are investigating as psilocybin is considered a Schedule III drug, which means it is illegal to distribute the substance,” police spokesperson Jackie Penman said.
Francis said he isn’t “necessarily worried” about the newly opened store being shut down, drawing a comparison with cannabis stores prior to legalization. “Psilocybin will be no different. It’s a charter issue … and as an adult, you should be able to control what you put into your body.”
Story from – Hamilton Spectator
A Legal Play for ‘Shrooms in Canada Could Make Waves in the US
Tiffany Kary – August 8, 2022
Welcome to The Dose, a weekly newsletter on cannabis and psychedelics. It’s clear from many pitches in my inbox that the psychedelics industry is optimistic the new Netflix series, ‘How To Change Your Mind,’ will spur more interest in the still-illegal drugs. But what are the actual prospects for a legal market to buy and sell them? Here’s a look at a lawsuit that some say has a shot at real change.
Canada’s big case
A Canadian lawsuit over magic mushrooms could help spur the wave of liberalization the nascent industry has been pushing for. So just who is behind it, and what are its prospects?
Filed in late July, the lawsuit challenges the Canadian federal government to make it easier for medical patients to get access to psilocybin, arguing that current regulations violate their constitutional rights. Brought on behalf of eight individuals with conditions such as depression, cancer and chronic pain, the lawsuit came together with the help of TheraPsil, a Victoria-based nonprofit that helps patients access psychedelic drugs through Canada’s current bureaucratic process of applying, one patient at a time, for government approval.
The case isn’t expected to see trial for another year or so, but if it succeeds, it could force Canada to set up a legal framework for medical psilocybin, similar to the one it established for medical marijuana in 2001. And, just as with Canada’s early adoption of medical marijuana, it could be a harbinger of more open access in the US and beyond.
“It doesn’t take a genius to look at what happened with cannabis,” said Spencer Hawkswell, TheraPsil’s chief executive officer.
The legal challenge came about collectively through the nonprofit’s board, which is made up of patients and healthcare practitioners who questioned how to speed up access to psilocybin for patients who don’t have long to live, Hawkswell told me. TheraPsil estimates its waitlist of people seeking help who are in palliative care is around 900. It has had about 2,000 requests in total.
One patient and plaintiff in the case is Thomas Hartle, a 54-year old former IT specialist with stage four colon cancer. He’s found psilocybin helps manage his anxiety about his condition. But after taking it about four times through Canada’s legal avenues, he’s having a hard time getting more, Hartle said. (Even though some people are “one and done,” he said he needs it about every six months to reset his frame of mind.)
The case could do more than just help Hartle and other Canadian patients. It’s part of a broad movement of advocacy that’s coming both from individuals and foundations.
“I think every step forward for psychedelics anywhere in the world helps every other jurisdiction that wants to legalize,” said Sanjay Singhal, a Canadian entrepreneur whose Nikean Foundation has donated to TheraPsil. He noted that while Nikean is an “enthusiastic supporter” of the legal action, as a charity, it can’t participate in legal or lobbying efforts. Singhal, who co-founded Audiobooks.com, recently sold that company.
Other TheraPsil donors include David Bronner, the CEO of Dr. Bronner’s soap, who’s been instrumental in US marijuana legalization and whose company donated more than $1 million to Oregon’s psychedelics legalization efforts. There’s also the Evolve Foundation, which describes itself as a philanthropic organization focused on the US and China. It has made more than 40 grants to organizations, many in the psychedelics and mindfulness space, according to its website.
Pushing for Changes
As efforts expand to legalize psychedelic treatments, an initiative in Oregon, which counted Bronner among its supporters, has found success.
It has the state on course to start legalized use for wellness starting in 2023. Some cities, such as Seattle and Detroit, have decriminalized psychedelic substances, which may improve research and an underground market, but doesn’t do much for legal products. Other efforts have fallen a bit flat — like a regulatory change in Canada earlier this year that has aimed to improve access for patients but has been criticized as too slow by TheraPsil and others.
Given Canada’s proximity to the large and influential US market — and the path of marijuana across North America — Canada’s psilocybin lawsuit has spurred some high hopes.
“If the lawsuit prevails, it’s going to be a revolution,” said Marc Goldgrub, a Toronto-based lawyer with Green Economy Law who specializes in psychedelics. Narrow medical use may pressure Canada to allow more widespread use for wellness — similar to Oregon’s approach.
“Money talks. I think if they open an individualized medical program, so much money is going to come up to Canada,” he told me. “And that money will push for a lot more.”
From there, the pressure would be on to the US to move forward with its own versions of legalization to stem an outflow of cash and talent to Canada, he predicted.
“We’re already seeing that money here,” he said. “I’m already getting calls from Americans who want to get involved.”
Story from – Bloomberg News
1st patient in Quebec gets approval from Health Canada for magic mushroom therapy
Montreal clinic becomes 1st in province to treat depression with psilocybin
Virginie Ann · The Canadian Press ·
When Thomas Hartle indulges in a session of psilocybin treatment, the end-of-life anxiety, distractions and noises associated with his terminal colon cancer go away.
“Before the treatment, it’s like you’re sitting in your car. It’s summer. You have your windows down, You’re stuck in rush-hour traffic. It’s noisy. It’s unpleasant,” said Hartle, who lives in Saskatchewan.
“Your favourite song is on the radio, but you can’t actually appreciate any of it because all of the other distractions are preventing you from even noticing that the radio is on. After a psilocybin treatment, [it’s like] you’re still in your car, in traffic, but you have the windows up, the air conditioning is on and it’s quiet. It’s just you and the music.”
Hartle, 54, is one of the very few Canadians to have received legal psychedelics psychotherapy for a mental health condition since Health Canada made it easier in January for health-care workers to access psilocybin — the hallucinogenic compound found in some mushrooms.
In Montreal, meanwhile, a pioneering clinic in the emerging field of psychedelic-assisted psychotherapy is about to become the first health-care facility in Quebec to legally treat depression with psilocybin.
“It’s a privilege to be able to accompany people in the exploration of their psychological distress and to offer something different than conventional treatment such as antidepressants,” Dr. Andrew Bui-Nguyen, of the Mindspace by Numinus clinic, said in a recent interview.
Bui-Nguyen said his clinic received Health Canada’s approval on May 5 to care for a patient who had undergone several unsuccessful treatments for depression.
“There’s a rigorous screening procedure,” Bui-Nguyen said, adding that Quebec’s health insurance plan doesn’t cover the treatment. “We look at the diagnosis, the medical history, if there’s a risk of addiction, what treatments have already been tried. There must have been a lot of treatments done beforehand so the application is solid.”
Health Canada on Jan. 5 restored its “Special Access Program” — abolished under former prime minister Stephen Harper in 2013 — allowing health-care experts to request access to restricted drugs that have not yet been authorized for sale in the country.
Before January, people could only access psychedelic-assisted psychotherapy through clinical trials or medical exemptions. Now, licensed experts can file applications on behalf of patients with mental health conditions such as post-traumatic stress disorder, depression and anxiety, but for whom conventional treatment has failed.
Health Canada says it has received 15 requests for the use of psilocybin or MDMA — a psychedelic drug with stimulant properties — since resuming the program.
In April, a clinic called Roots To Thrive, in Nanaimo, B.C., became the first health centre in Canada to offer a legal psilocybin group therapy program, in which Hartle took part.
“The therapy part has a capital T in this whole process,” Hartle said. “It isn’t just taking psychedelics. It’s just a tool in the process; the therapy is crucial to getting a good outcome.”
Psychedelic-assisted treatment, Bui-Nguyen explained, requires multiple therapy sessions before and after patients experience the drug. Patients will consume psilocybin while they are supervised by two psychotherapists and remain in the clinic-secured environment for up to six hours.
“It’s not miraculous,” Bui-Nguyen said. “You don’t take psilocybin and that’s it, a psychedelic trip and after the depression is cured — no! The patient has a lot of work to do. But it opens perspectives; it creates new paths in the brain that we aren’t used to taking. The patient then explores new roads to get out of depression.”
In the world’s largest study on psychedelics’ affect on the brain, released in March in the journal Science Advances, lead author Danilo Bzdok said psychedelic drugs might just be the next big thing to improve clinical care of major mental health conditions.
“There’s something like a renaissance, a reawakening of psychedelics,” Bzdok, an associate professor with McGill University’s biomedical engineering department, said in a recent interview.
He said the evidence-based benefits are very promising. Patients, he said, say they have experienced up to six months of lasting effects after a single psychedelic-aided therapy session. They have also experienced a reduction of symptoms associated with mental health conditions, Bzdok said, adding that there were fewer side-effects compared to antidepressants.
Mindspace by Numinus CEO Payton Nyquvest said psychedelics have the potential to become a widespread treatment. As Health Canada continues to approve more requests, he hopes the recognition will make the treatment much more accessible.
“We haven’t seen significant innovation in mental health care in probably over 40 years,” Nyquvest said in a recent interview.
“We’re at a time where new and better treatments for mental health are needed now more than ever. No matter what you look at, depression, anxiety, and suicidality … these are all rates that continue to go up with no clear line in terms of how we’re going to address these massive societal issues. Psychedelics represent an opportunity to make a significant impact.”
Hartle’s own experience echoed those hopes. “The improvement in my mental health is so night and day that it would be difficult to say all of the things that it does for me,” he said.
“I still have cancer. I still have difficulty with what it physically does, but there are days when I don’t even think about it. What would you do to have a day where you just feel normal?”
Story from – CBC.ca
Terminally ill B.C. patients the first in Canada to consume legal supply of magic mushrooms
“Having this approval, I feel like the luckiest person. I know a number of people with cancer who have died waiting for one.” — Thomas Hartle
Sarah Grochowski – Apr 02, 2022
One of them, 54-year-old Thomas Hartle, arrived at Nanaimo airport Saturday morning from his home in Saskatoon to participate in psychedelic therapy using psilocybin, the active ingredient in magic mushrooms, which he hasn’t been able to legally do since August, when his one one-year exemption from the Controlled Drugs and Substances Act expired.
By that time, his Stage 4 colon cancer had returned.
“Having this approval, I feel like the luckiest person. I know a number of people with cancer who have died waiting for one,” said Hartle, a father of two girls, who will undergo psychedelic therapy by palliative care physicians with Nanaimo-based health care organization Roots To Thrive.
“I really didn’t think I was going to make it this long,” he said.
Psychedelic-inspired approaches for treating neurodegenerative disorders
This Review article is part of the special issue – Psychedelics & Neurochemistry
Abstract
Psychedelics are increasingly being recognized for their potential to treat a wide range of brain disorders including depression, post-traumatic stress disorder (PTSD), and substance use disorder. Their broad therapeutic potential might result from an ability to rescue cortical atrophy common to many neuropsychiatric and neurodegenerative diseases by impacting neurotrophic factor gene expression, activating neuronal growth and survival mechanisms, and modulating the immune system. While the therapeutic potential of psychedelics has not yet been extended to neurodegenerative disorders, we provide evidence suggesting that approaches based on psychedelic science might prove useful for treating these diseases. The primary target of psychedelics, the 5-HT2A receptor, plays key roles in cortical neuron health and is dysregulated in Alzheimer’s disease. Moreover, evidence suggests that psychedelics and related compounds could prove useful for treating the behavioral and psychological symptoms of dementia (BPSD). While more research is needed to probe the effects of psychedelics in models of neurodegenerative diseases, the robust effects of these compounds on structural and functional neuroplasticity and inflammation clearly warrant further investigation.
For more information: OnLine Library – Wiley.com
Download PDF here: PDF
People ‘microdosing’ on psychedelics to improve wellbeing during pandemic
Addiction expert says findings of survey suggest small doses of drugs being taken to treat health issues – December 2021
There has been a shift towards recreational drug users taking tiny doses of psychedelics, such as LSD and magic mushrooms, to improve their wellbeing and mental health during the pandemic, a leading addiction expert has said.
People were microdosing to self-medicate rather than following the trend, popularised in Silicon Valley, of consuming small amounts of psychedelics to enhance creativity, Prof Adam Winstock, the founder and director of the Global Drug Survey, said.
The 2021 survey found that among those respondents who both microdosed and took psychiatric drugs almost half reported reducing or stopping their prescribed medication.
Winstock, a London-based consultant psychiatrist and addiction medicine specialist, said the findings suggested people had been experimenting with microdosing during the pandemic, perhaps due to increased waiting times for mental health services.
The report also found people were experimenting with a wide variety of psychedelics. About a third of those who microdosed with LSD or magic mushrooms (psilocybin) reported also trying other substances, including ecstasy (MDMA), ketamine, a dissociative anaesthetic, and ayahuasca, a strong hallucinogenic plant-cocktail revered by indigenous faith healers.
While a tripping dose of LSD is about 100 micrograms, ambitious tech workers from Silicon Valley have eulogised the effect of taking 10 to 20 micrograms every few days on their creativity and productivity, with people in the UK reporting doing so for similar reasons.
“In the past people were using microdosing for performance enhancement and creativity,” said Winstock. “Now, I think people are shifting towards using microdosing to enhance wellbeing and to address mental health distress.”
Of the fifth of microdosers who said they were taking psychiatric drugs, about a quarter reported they stopped taking their medications altogether and another quarter reduced their intake.
“This, for me, is microdosing shifting into treating mental health,” added Winstock, who is an honorary clinical professor at the Institute of Epidemiology and Health Care, University College London.
More than a fifth of respondents to the survey who had used LSD and magic mushrooms in the last 12 months reported having microdosed either drug during that period.
Three-quarters of them reported no side-effects, while about 10% reported unwanted mental effects and 8% physical effects.
Winstock was cautious about the findings, noting that the majority of research on psychedelics and mental health involved full doses of the drugs.
He said he hoped the survey would encourage mental health services, the psychiatric establishment and policymakers to engage positively with microdosing, adding that if the practice remains illegal vulnerable people could be exploited or accidentally take hallucinogenic and harmful doses.
The largest placebo-controlled trial into psychedelics to date by researchers at Imperial College London found that the mood uplift reported by microdosers might just be the placebo effect.
One of the lead researchers on that study, Dr David Erritzoe, clinical director of the university’s Centre for Psychedelic Research, said he supported further clinical trials into the possible benefits of microdosing.
But he added that the hype around the practice was leading people to report inflated positive effects.
“The problem is that it’s a bit counterculture and from something as cool as Silicon Valley. You have bestselling books by really cool people writing about how their lives have been transformed. And it taps into scepticism about medical expertise and big pharma. All that adds to people’s expectations and a potential placebo effect.”
The 2021 Global Drug Survey, which received responses from more than 32,000 people from more than 20 countries between December 2020 and March 2021, also noted the impact of Covid, with a slight drop in the use of recreational drugs.
While the use of psychedelics had dropped slightly over that period, Winstock said data from the previous six years showed an upward trend in their use.
Many people also reported that they had taken further precautions when taking drugs socially during the pandemic.
Of the 14,000 respondents who reported using cannabis, 42% said they less frequently shared a joint, vape, pipe or bong with other people during the pandemic.
Just under a quarter (24%) said they were more likely to use joints, pipes and bongs prepared only by themselves, while a fifth reported increasing social distancing while using cannabis.
Of the respondents who reported using cocaine, 26% said they were less likely to share a straw or snorter with another person, while a fifth said they were less likely to snort a line racked up by someone else.
As we approach the end of the year in Canada, we have a small favour to ask. We’d like to thank you for putting your trust in our journalism this year – and invite you to join the million-plus people in 180 countries who have recently taken the step to support us financially, keeping us open to all, and fiercely independent.
In 2021, this support sustained investigative work into offshore wealth, spyware, sexual harassment, labour abuse, environmental plunder, crony coronavirus contracts, and Big Tech.
The new year, like all new years, will hopefully herald a fresh sense of cautious optimism, and there is certainly much for us to focus on in 2022 – a volley of elections, myriad economic challenges, the next round in the struggle against the pandemic and a World Cup.
With no shareholders or billionaire owner, we can set our own agenda and provide trustworthy journalism that’s free from commercial and political influence, offering a counterweight to the spread of misinformation. When it’s never mattered more, we can investigate and challenge without fear or favour.
Unlike many other media organisations, Guardian journalism is available for everyone to read, regardless of what they can afford to pay. We do this because we believe in information equality. Greater numbers of people can keep track of global events, understand their impact on people and communities, and become inspired to take meaningful action.
If there were ever a time to join us, it is now. Every contribution, however big or small, powers our journalism and sustains our future.
Story from The Guardian
Metaphysics and mushrooms: Psychedelics can change how you think about the universe
Research shows that psilocybin leads people away from materialism and toward transcendentalism. Apparently, mushrooms teach metaphysics.
NEUROPSYCH —
Metaphysics is the branch of philosophy that deals with “being.” A new study finds that a single trip on a psychedelic can cause lasting changes in a person’s metaphysical beliefs. Overall, people moved away from “hard materialism” to more transcendental, idealistic, and supernatural views of the cosmos.
After decades of being shunned, psychedelics are enjoying a biomedical renaissance because many of them show great promise in treating a variety of mental health conditions when used in tightly controlled environments. Now, a new study, soon to be published in Scientific Reports, claims that psychedelics can change a person’s beliefs about metaphysics.
Of metaphysics and mushrooms
Everyone has metaphysical beliefs, even if they are unaware of them. For example, many people have an intuitive belief in mind-body duality (that is, the mind and body are separable) even if they have never heard of the term. These beliefs are often associated with certain behaviors as well, with dualists taking less care of their bodies than physicalists, who argue that the mind is part of the body. Similar relationships between metaphysical beliefs and human behavior can be found elsewhere. Those who believe in free will are less likely to lie, cheat, and be aggressive.
Sharpening one’s understanding of metaphysics can be accomplished with various methods, such as meditation. Near death experiences often do the same. One commonly discussed but less investigated method is psychedelic drug use. While many anecdotes suggest that psychedelics cause people to adopt a non-materialist view of the cosmos, hard data was lacking. After all, it could just be that those already predisposed to idealism — the notion that fundamental reality is mental rather than physical — are also more likely to try these drugs.
In the first attempt to confirm and quantify these effects, a team of researchers led by Dr. Christopher Timmermann of the Centre for Psychedelic Research at the Imperial College London gauged the metaphysical stances of several hundred people before and after they tripped in a ritualistic setting.
Philosophy, drugs, and rock ‘n’ roll
The study came in two parts. In the first, nearly 900 volunteers who signed up to attend a psychedelic ceremony were recruited to answer a series of questions — for instance, on realms of existence — aimed at determining their baseline metaphysical beliefs. After the ceremony (in which psilocybin was used), the volunteers were asked to complete the survey again four weeks and six months later.
In general, users reported moving away from belief in materialism or physicalism — that is, the idea that the universe is primarily physical rather than mental or spiritual — and toward other views such as transcendentalism, non-naturalism, or idealism. Effects were seen at both four weeks and six months, and the effects were largest for those who were taking the drug for the first time. Another important change was the drift from hardline stances of any kind toward more mixed or moderate views. Participants also reported improved mental health.
The clinical trial was similar but involved only 60 participants. Half were given escitalopram (an antidepressant) and the other half psilocybin. The results were largely the same, with the psilocybin group experiencing a shift away from hard materialism toward more transcendental, idealistic, and supernatural conceptions of the universe.
Overall, the psychedelic experience moved people away from a “hard materialist” view. However, regardless of belief (in materialism or dualism), people tended to moderate their views after taking the drug — as if psychedelics made people more tolerant of uncertainty.
Caveat emptor
In an email to BigThink, Dr. Timmermann summarized the findings by explaining:
“…[t]hat we provide evidence for the first time that psychedelics shift beliefs concerning the nature of reality. These beliefs are central to the way human beings organize society and may correspond to deeply rooted worldviews. Specifically, we found that people rejected the notion of physicalism (the idea that the world is made up of material, as opposed to mental or spiritual things) after a single psychedelic experience, endorsed the notion of fate more, and also the idea that all things in the universe are conscious, what we call panpsychism. Importantly, we found that these changes were related to improvements in mental health.”
The authors note that it is beyond the scope of the paper to draw any conclusions regarding which metaphysical system is best for mental health. They do speculate that very stringent beliefs of any kind about metaphysics are unhealthy. Finally, the authors advise that future studies involving psychedelics warn participants that their worldviews may be altered by their participation. Caveat emptor: Acid might change your perspective on panpsychism.
Story from Big Think
Mark Messier on leadership, trust and magic mushrooms
The hockey icon talks with Marie-Danielle Smith about mental health, hockey violence—and what he’ll do when the New York Rangers call
By Marie-Danielle Smith – October 21, 2021
He’s a six-time Stanley Cup winner, the second most prolific playoff-points scorer ever, a two-time most valuable player in the NHL, a 15-time all-star and the only person ever to captain two different teams to Stanley Cup championships—the Edmonton Oilers, even after the departure of his great friend Wayne Gretzky, and the New York Rangers.
First he was “the Moose,” then he was “the Messiah,” according to New Yorkers—that’s a play on his last name—for ending a 54-year Stanley Cup drought in 1994. He’s an officer of the Order of Canada. And he’s now the author of a memoir he hopes will convey the lessons he learned along the way.
Mark Messier chatted with me ahead of the release of No One Wins Alone, authored with writer Jimmy Roberts. Our conversation has been edited for length and clarity.
Q: Your book is a meditation on leadership as much as it is a memoir. What’s the biggest lesson you’re hoping people will draw from it?
A: One of the questions I get all the time is: what’s the single most important lesson of leadership? I’m not sure there’s an answer because it’s so multidimensional. I do know that earning trust is just massive and earning the right to lead the people is critical. You know, Abe Lincoln said no man can govern another without his consent. You can’t expect to lead people unless you’ve earned that right.
Q: How do you earn it?
A: It always starts with trust. One of the most important things I did with the players I played with was getting to know them on a more personal level. Taking the time to understand where they came from. Understanding who they are as people and spending as much time as possible with them away from the rink so you develop a relationship that is deeper than a professional relationship.
John Wooden, a great basketball coach, said great coaching is being able to give correction without resentment. When you’ve got to be honest with a player and he might not like it but he doesn’t hold it against you or think you have something against him as a person. As a leader you’ve got to be able to go home at night and put your head on the pillow and know it’s up to him to resolve the issue.
Q: You talk about the importance of connection between teammates. Your relationship with Wayne Gretzky shines through as a critical one.
A: It’s not very often that you can look at someone eight days younger than you and look at them as a role model. Normally you get that from folks who are much older than you, who have been around with much more experience. But our best example was the same age as us. We’re all grateful that the stars collided and that we all came together at the same time.
Q: How important is it to see your teammates as friends?
A: When we talk about being brothers, I don’t think we reference each other like that lightly. Maybe you don’t need to have that in order to win, I don’t know—I didn’t have that experience on the teams I was fortunate enough to win with. Maybe you can win without that real tight level of friendship.
Q: How important is it to believe you’re going to win, and to be able to say that out loud?
A: I don’t think you can be afraid to fail. I think you really need to be forthright in your objective. For us in hockey at a professional level, you have a very defined goal of what success is. You can have smaller goals along the way and celebrate those goals, but ultimately you’re there for one reason and that’s to win a Stanley Cup. It might take some time to build a team and get some experience and put the pieces in place to do that. But you always have to have in the back of your mind on a day-to-day basis: are we closer to winning a Stanley Cup or are we further away?
And making sure that everybody in the organization, whether they’re on the ice as a player, or with a trainer or a doctor, physicians, therapists, equipment managers, managers, coaches, everybody is there with the same goal in mind, believing in the philosophy and the vision of the team and the culture the team created. Then you just start chopping wood and carrying water toward that goal.
Q: You probably get this question all the time, but is there a moment you would pick out as your ultimate career highlight?
A: To come to New York and win a championship that hadn’t been won in 54 years was incredible. And it’s pretty remarkable what happened in Edmonton, coming from an expansion team to winning the Stanley Cup, and going on to win five cups in seven years. I just can’t compartmentalize one moment in a career over 26 years. There’s too many special moments and they’re all different in their own rights.
Q: The game has changed a lot since you started playing, especially in the physicality. What do you think of how hockey has evolved?
A: I’m happy the game has evolved in so many ways. They’ve made changes to the game to get the speed and the finesse and the artistry back into the game, instead of hooking and clutching and holding and grabbing. They opened up the game to more excitement for the fans. It’s a better product when the game is played like that. There’s still plenty of physicality.
The equipment has changed. Technology has entered into hockey like every other sport, not only with the equipment but with the training. The players are making incredible use of science now to train all year round. So many things have advanced in the sport, but ultimately in the end the game is still won on the ice between the boards. It always gets down to a test of will, and that’s what makes hockey so great.
Q: There’s a scene in the book where your son is looking at old videos and he says something like, “You’d be in jail for some of those hits if they happened now.” How do you talk to your kids, and young people, about how things used to be and how much has changed?
A: I think we all recognize that as the game evolved and concussions started to enter into sports, if things didn’t change, the game wouldn’t last. So the game had to evolve and I’m glad both the NHLPA and the NHL took a collaborative effort to do that, and the players took the responsibility to change the way the game was played.
I don’t think anybody’s proud of some of the things that happened back in the day, but it was a different landscape back then. Intimidation was a huge part of hockey. [The game] evolved into something that is acceptable with all the social media applications and video reviews. You can’t get away with anything.
Some of our games back when I first started playing professional hockey weren’t even televised. There wasn’t even a camera in the rink. And we’ve brought the fans closer to the game. The fans are more knowledgeable about what’s going on, not only on the ice but also behind the scenes. The culture of professional sports is more exposed than ever.
Q: There seems to be no room for error with social media. What do you think about what young players are dealing with today?
A: There’s a different kind of pressure on the players now that we were never exposed to, socially, politically, and the choices they make and the way they represent not only the team but also the league and the community.
What it really boils down to is character becomes high-stakes, or of very high importance. To be able to handle it all. We don’t expect anybody not to make mistakes, mistakes are part of life, it’s how you learn, it’s how you grow, it’s how you evolve. So I think there’s some forgiveness for a mistake but there’s not forgiveness for a history of certain actions that aren’t acceptable anymore.
Q: Are you worried that forgiveness isn’t always extended to people who might deserve it? The online mob kind of picks its targets.
A: If you go down the rabbit hole of getting acceptance from people online, that’s a dangerous place to be. I don’t think it’s a good idea for anybody to be looking there for self-worth or validation, acceptance, because as we know there are people who just don’t have anything better to do who will be hurtful. It’s not a good place to be looking for that kind of information.
Q: Younger athletes are applauded today for talking about the pressure they’re under, and prioritizing their mental health even if it means taking time away from competing. Do you think that’s a good thing?
A: Everybody needs help no matter what position you’re in, no matter where you are in your own life. The biggest thing that has come out of all of this is that there’s no shame in admitting any problem, and seeking help has been very productive and helpful for a lot of folks.
Q: You talk in the book about conquering negative self-talk and learning to think positively about yourself. Were there times when that was hard for you?
A: I didn’t think about it much as a young player, to be honest with you. I had a lot of confidence. But everybody struggles. Even at the peak of my career I would struggle at times. I was fortunate enough that we had sports psychology seminars at a very early age, basically the first year of my career when I was 18 years old. I kept it with me my whole career.
Self-confidence is huge and a big part of that is self-talk—when things aren’t going well, not to be negative. You have to figure out what went wrong so you’re able to move on from any failure.
Q: You describe taking magic mushrooms at 19 as a transformative experience. Tell me more about how your perspective expanded.
A: Well that’s what it did for me. I had no idea the mind was that powerful. And how could eating a natural mushroom that was organically grown create that kind of stimulus? Obviously it turned out to be an amazing experience, but more important was the question afterwards: wow, how can I use my mind to empower myself to be a better player, to be a better person, to have more energy, to create a better aura?
So then I became interested in Eastern philosophy, meditation, Buddhism, the spirituality of Indigenous peoples. The power of the mind.
Q: Is spirituality still a big part of your life?
A: It’s always been a big part of my life. I grew up Catholic but was interested in a lot of Eastern philosophy. So I think spirituality became more important to me than the so-called religion I grew up with.
Q: You obviously took leadership lessons from these philosophies. You even end the book with a quote from a Hindu text.
A: There are so many powerful lessons to be learned about the goodness that lives in everybody’s heart. And creating a culture that is just so rich with humility and passion and creativity and all the things that make it fun to come to the rink, or to come to work. It’s the essence of a team that can go all the way. A unique environment with the diversity of the players, of where they come from, and their ideas. And really acknowledging that and letting people shine in their own ways.
Q: You talk about the importance of diversity and making people feel comfortable, but people of colour haven’t always felt comfortable in the NHL. What are your thoughts on that?
A: I know a huge mandate—from the NHL, the NHLPA and everybody involved with the league—is to grow the game. Diversify the game. Give more kids—more girls, more boys—access, opportunity. And it just makes sense. The Kingsbridge [Armory] project I was doing in the Bronx, that’s what it was for, to grow the game and its diversity by creating access and opportunity that are just not there right now. The NHL has immersed themselves in communities and they’ve taught boys and girls the game of hockey who’ve become fans and who are going to continue to get more people of colour involved in the game.
Q: Do you think that in the past there were failures of leadership on this?
A: I can’t speak to that myself. I don’t know enough to say yes or no. I think creating access and opportunity is a huge first step.
Q: Would you be tempted to get involved in the NHL again as a coach or a manager?
A: I think I’ve always felt I could help an organization in many ways. But it’s important to be with people who believe you can help. If it happens, great. If it doesn’t happen, that’s okay as well. If the occasion ever came where someone thought I could help them, I would be more than happy to have that conversation.
Q: If the New York Rangers called, would you go for it?
A: I don’t work in hypotheticals. If the right person thought I could help their team, I’d be more than willing to listen.
Story from – MacLean
Ketamine and psilocybin, better known as party drugs, showing promise for treatment of mood disorders
Chad Derrick, W5 producer and Avery Haines, W5 correspondent
Saturday, October 23, 2021
TORONTO — It’s been more than a decade since Bruno Guevremont returned to Canada from his military deployment to Afghanistan. Like so many other veterans, Guevremont’s combat experiences took a mental toll.
During his second tour in 2009, Guevremont was part of a team that dismantled IEDs, or improvised explosive devices.
One incident, in particular, changed him. Guevremont says he was the first Canadian soldier ever to defuse a suicide vest on a living person. But it wasn’t the high degree of danger in that situation that affected him.
“The suicide bomber was mentally challenged. He had been told that if he doesn’t do this, then they were going to kill his family,” Guevremont told W5 correspondent Avery Haines. “So that started playing with my mind.”
After his return to Canada, Guevremont suffered panic attacks and suicidal thoughts. He was diagnosed with PTSD, depression and anxiety.
When talk therapy and anti-depressants didn’t help, Guevremont sought alternatives in an attempt to recover his mental health. He joined an Arctic expedition with other veterans in 2014, captained Team Canada at the 2016 Invictus Games, and became a mental health spokesperson for Bell Let’s Talk Day.
Then, in March, 2020, the COVID-19 lockdown sent Guevremont into a tailspin, and he contemplated suicide again.
“I started getting really depressed, started getting dark thoughts,” he told W5.
That’s when Guevremont learned about an unconventional treatment for severe depression and PTSD, involving the drug ketamine.
Ketamine is notorious for being a hallucinogenic party drug nicknamed Special K, a veterinary tranquilizer and an anesthetic that’s been used in hospitals for over 50 years. But at sub-anesthetic doses, the drug has shown an ability to quickly reduce symptoms of depression and suicidal thinking, within weeks to hours.
“The magnitude of improvement on the symptoms approaches in many studies between 40 to 70 percent improvement within a couple of weeks,” noted Dr. Roger McIntyre, a professor of Psychiatry and Pharmacology at the University of Toronto. In 2018, McIntyre founded the Canadian Rapid Treatment Center of Excellence (CRTCE) – Canada’s first private clinic to offer ketamine treatments for depression.
The Canadian Mental Health Association reports that approximately five per cent of Canadians are affected by major depression and more than 4,000 Canadians died by suicide in 2019.
“This is truly a breakthrough,” said Dr. McIntyre.
In November 2020, after his bout with depression, Bruno Guevremont travelled from his home in Victoria, B.C. to Field Trip Health, in Toronto – for orally administered ketamine treatment.
While ketamine’s anti-depressant effects are well documented, therapists at Field Trip Health also aim to maximize the psychedelic qualities of the drug and combine it with psychotherapy.
“The transformation doesn’t happen within the session itself. That happens before and after, when you are working on your trauma, when you’re actually making sense of it,” said Guevremont.
In 2020, Health Canada approved a ketamine-derived nasal spray for treatment-resistant depression and has allowed off-label use of the drug when administered intravenously or orally by health care professionals.
But a host of other illegal psychedelics and party drugs are also being studied for their therapeutic value. Among them, psilocybin, the psychoactive ingredient in magic mushrooms. Clinical trials with psilocybin have shown an improvement in symptoms for patients battling a range of disorders including depression and anxiety.
Though scheduled as a controlled substance, in 2020 Health Canada started offering what are known as Section 56 exemptions to patients with end-of-life distress so they could undergo therapeutic sessions with the drug.
Meanwhile, clinics that treat depression with ketamine are opening up across Canada. There are currently at least 12 private facilities and several hospital-based programs.
But ketamine treatments are not a “cure” or even suitable for everyone with mood disorders. Patients may be ineligible for treatment if they exhibit a history of psychosis, hypertension or substance abuse.
A typical ketamine treatment regimen involves 4 to 6 sessions over a two-to three-week period. Patients often need booster doses and the long term effects are still unclear, though researchers say there is little evidence to support addiction to the drug when it’s administered under medical supervision.
Also, the cost of private treatment isn’t cheap — $750 per ketamine session and $250 for each psychotherapy appointment at Field Trip Health, and approximately $850 per intravenous infusion at the CRTCE.
But for patients like Bruno Guevremont, treatments with ketamine have offered a renewed outlook.
“Life is actually enjoyable, which is amazing,” he said. “I didn’t want to be here. Now I do.”
Story from – CTV website
Music an essential part of psilocybin assisted therapy, research suggests
Liam O’Dowd – October 6, 2021
Danish scientists at the European College Of Neuropsychopharmacology have found that psilocybin, the active ingredient in magic mushrooms, significantly changes the emotional state of people listening to music.
Psilocybin assisted therapy is being developed as a treatment for depression and other mental health conditions, with pre-selected music playlists being a common feature in therapy settings. The study, to be presented at the ECNP Congress in Lisbon, shows that enhanced emotional processing may be a positive outcome of combining psilocybin with music, suggesting that music should be an active component of psilocybin therapy.
In the study, 20 healthy participants were tested on their emotional response to music before and after given psilocybin. 14 of these participants were also tested after being given ketanserin, an anti-hypertension drug commonly used as a comparison in psychedelic experiments. Whether ketanserin or psilocybin was given first was randomly selected and each person was thus able to report on the changes effected by both psilocybin and ketanserin. At the peak of drug effects, participants listened to a short music program and rated their emotional response.
Lead researcher Associate Professor Dea Siggaard Stenbæk said: “We found that psilocybin markedly enhanced the emotional response to music, when compared to the response before taking the drugs. On the measurement scale we used, psilocybin increased the emotional response to music by around 60%. This response was even greater when compared to ketanserin. In fact, we found that ketanserin lessens the emotional response to music. This shows that [the] combination of psilocybin and music has a strong emotional effect, and we believe that this will be important for the therapeutic application of psychedelics if they are approved for clinical use. Psilocybin is under development as a drug to treat depression, and this work implies that music needs to be considered as a therapeutic part of the treatment.
“Our next step is to look at the effect of music on the brain while under the influence of psilocybin in data material we have already collected, using an MRI”.
While the results of the study are unlikely to surprise any recreational user of psychedelic drugs, it is significant in the development of clinical settings for psilocybin assisted therapy. Commenting on the study Professor David Nutt of Imperial College, London said: “This is further evidence of the potential of using music to facilitate treatment efficacy with psychedelics. What we need to do now is optimise this approach probably through individualising and personalising music tracks in therapy”.
The emotional response to the music in the study was rated according to the Geneva Emotional Music Scale. The music used was a short programme comprising Elgar’s Enigma Variations no 8 and 9, and Mozart’s Laudate Dominum, together lasting around 10 minutes. Interstingly, Elgar was encouraged to write some of the music used as a way out of depression by his close friend Augustus Jaeger. “We’re pleased to see it used again to help understand more about mental health” Professor Stenbæk added.
Story from Leafie UK
Alison Myrden submits to the Minister of Health a s. 56 application to grow 50 grams/ day of psilocybin mushrooms
September 28, 2021 LewinSagara
Cannabis & Psychedelics Law Group LLP have submitted a s. 56 application on behalf of Alison Myrden to the Minister of Health seeking a 50 grams/ day exemption which would also allow Ms. Myrden to grow her own psilocybin. Henria Stephens has done some terrific work in assisting with this application.
Ms. Myrden suffers from Bilateral Trigeminal Neuralgia which is a vicious condition that causes chronic and excruciating pain on both sides of her face, as well as painful facial tics. The trigeminal nerve is the source of the pain. It leads to eye pain that causes cluster migraines. Some sufferers describe it as getting electric shocks to the face. This condition “is one of the most characteristic and difficult to treat neuropathic pain conditions in patients with multiple sclerosis.” It has caused her to suffer from severe facial pain 24 hours a day which starts as soon as she is conscious in the mornings.
Ms. Myrden also suffers from Primary Progressive Multiple Sclerosis (PPMS) which is the worst type of MS. Her MS has gotten worse and worse. She suffers from constant nerve pain, fatigue, balance issues, vision problems and speech problems. The psilocybin helps with all of these.
Ms. Myrden has tried a long list of drugs and treatments. Many of these drugs have caused further health problems. Cannabis has helped. However, nothing is as effective at reducing the pain as psilocybin. This is similar to the cluster headache sufferers who have obtained relief through psilocybin. Ms. Myrden requires 50 grams of psilocybin mushrooms a day. She has developed somewhat of a tolerance to psilocybin mushrooms so she needs a bit more than the average person. She also needs psilocybin mushrooms all through the day as her pain is with her all through the day.
Ms. Myrden is seeking to grow her psilocybin herself. Psilocybin mushrooms do not grow in the wild where Ms. Myrden lives. Also, she is cautious about inadvertently picking mushrooms that are unsafe for human consumption. She would prefer to have control over her medicine. At the Ontario Court of Appeal found in Hitzig v. Canada, the right to use a drug is useless without a legal supply.
The decision to grant a s. 56 exemption must be made in a manner consistent with the Charter of Rights and Freedoms. The Supreme Court of Canada, in PHS Community Services Society v. Canada 2011 SCC 44, at para. 117, said
The discretion vested in the Minister of Health is not absolute: as with all exercises of discretion, the Minister’s decisions must conform to the Charter: Suresh v. Canada (Minister of Citizenship & Immigration), 2002 SCC 1, [2002] 1 S.C.R. 3 (S.C.C.). If the Minister’s decision results in an application of the CDSA that limits the s. 7 rights of individuals in a manner that is not in accordance with Charter, then the Minister’s discretion has been exercised unconstitutionally.
Ms. Myrden believes the Minister of Health will do the right thing and grant Ms. Myrden an exemption. As various courts have held over the years, no person should have to choose between their health and the law.
Alison gets great relief from Psilocybin found in various types of “Magic Mushrooms” …
Possessing And Cultivating Psychedelics Would Be Legalized In Michigan Under New Senate Bill
Michigan senators on Thursday introduced a bill to legalize the possession, cultivation and delivery of an array of plant- and fungus-derived psychedelics like psilocybin and mescaline.
The legislation, sponsored by Sens. Jeff Irwin (D) and Adam Hollier (D), would amend state statute to exempt people from criminal penalties for such activities so long as they are not “receiving money or other valuable consideration for the entheogenic plant or fungus.”
As such, commercial production and sales would not be legalized under the measure.
The legislation does clarify, however, that people can charge a “reasonable fee for counseling, spiritual guidance, or a related service that is provided in conjunction with the use of an entheogenic plant or fungus under the guidance and supervision of an individual providing the service.”
Irwin said in a tweet that “decriminalization of entheogenic substances makes sense.”
“There is medicinal value. These plants and fungi have religious significance. And these substances are relatively safe and not prone to abuse,” he said. “Let’s stop wasting time and money making more victims of the War on Drugs.”
The list of entheogenic substances that are covered under the proposal includes plants and fungi that naturally produce DMT, ibogaine, mescaline, psilocybin and psilocyn.
Notably, the inclusion of mescaline doesn’t specifically prohibit the substance from being derived from the cacti peyote, despite some concerns about overharvesting that have been raised by indigenous groups and have led to that specific plant being left out of other reform proposals across the country.
Michigan has become a unique hub for the psychedelics movement, with local chapters of the group Decriminalize Nature pushing their city councils to adopt reforms.
The Ann Arbor, Michigan City Council approved entheogenic decriminalization last year—and in July, local lawmakers passed a resolution to officially designate September as Entheogenic Plants and Fungi Awareness Month.
Efforts are also underway in Grand Rapids to enact a policy change for the psychedelic substances.
But the new bill, SB 631, is the latest example of how this local movement is expanding and reaching state lawmakers.
A California senator advanced a bill to legalize the possession of psychedelics through the Senate and two Assembly committees, but he recently put the effort on pause until next year to generate additional buy-in.
Activists in California are also hoping to place an initiative before voters in 2022 to legalize the possession and sale of psilocybin. And a legislative analysis of the proposal that was released this week found that it would reduce costs associated with enforcing laws against the substance.
Oakland and Santa Cruz have already enacted psychedelics decriminalization.
Oregon voters approved a first-of-its-kind initiative last year to legalize psilocybin for therapeutic use alone.
Meanwhile, Denver activists who successfully led a 2019 campaign to make the city the first in the U.S. to decriminalize psilocybin possession have their eyes set on broader reform, with plans in the works to end the criminalization of noncommercial gifting and communal use of the psychedelic.
Massachusetts cities that have enacted the policy change are: Northampton, Somerville and Cambridge. In July, state lawmakers heard testimony about a bill to create a task force charged with studying the implications of legalizing psychedelics like psilocybin and ayahuasca.
The governor of Connecticut recently signed legislation recently that includes language requiring the state to carry out a study into the therapeutic potential of psilocybin mushrooms.
Texas also recently enacted a bill to require the state study the medical benefits of psychedelics for military veterans.
A New York lawmaker introduced a bill in June that would require the state to establish an institute to similarly research the medical value of psychedelics.
In Oakland, the first city where a city council voted to broadly deprioritize criminalization of entheogenic substances, lawmakers approved a follow-up resolution in December that calls for the policy change to be adopted statewide and for local jurisdictions to be allowed to permit healing ceremonies where people could use psychedelics.
After Ann Arbor legislators passed a decriminalization resolution last year, a county prosecutor announced that his office will not be pursuing charges over possessing entheogenic plants and fungi—“regardless of the amount at issue.”
The Aspen, Colorado City Council discussed the therapeutic potential of psychedelics like psilocybin and proposals to decriminalize such substances at a meeting in May. But members said, as it stands, enacting a reform would be more better handled at the state level while entheogens remain strictly federally controlled.
Seattle lawmakers also recently sent a letter to members of a local task force focused on the opioid overdose epidemic, imploring the group to investigate the therapeutic potential of psychedelics like ayahuasca and ibogaine in curbing addiction. In response, the task force on issued a recommendation for the widespread decriminalization of all drugs. The group said psychedelics in particular could represent a promising treatment to address substance abuse disorders and mental health issues.
Meanwhile, Portland, Oregon activists are mounting a push to have local lawmakers pass a resolution decriminalizing the cultivation, gifting and ceremonial use of a wide range of psychedelics.
In a setback for advocates, the U.S. House of Representatives recently voted against a proposal from Rep. Alexandria Ocasio-Cortez (D-NY) that would have removed a spending bill rider that advocates say has restricted federal funds for research into Schedule I drugs, including psychedelics such as psilocybin, MDMA and ibogaine. However, it picked up considerably more votes this round than when the congresswoman first introduced it in 2019.
Report provisions of separate, House-passed spending legislation also touch on the need to expand cannabis and psychedelics research. The panel urged the National Institute On Drug Abuse (NIDA) to support expanded marijuana studies, for example. It further says that federal health agencies should pursue research into the therapeutic potential of psychedelics for military veterans suffering from a host of mental health conditions.
When it comes to broader drug policy reform, Oregon voters also approved an initiative in November to decriminalize possession of all drugs. This year, the Maine House of Representatives passed a drug decriminalization bill, but it later died in the Senate.
In May, lawmakers in Congress filed the first-ever legislation to federally decriminalize possession of illicit substances.
Story from Marijuana Moment
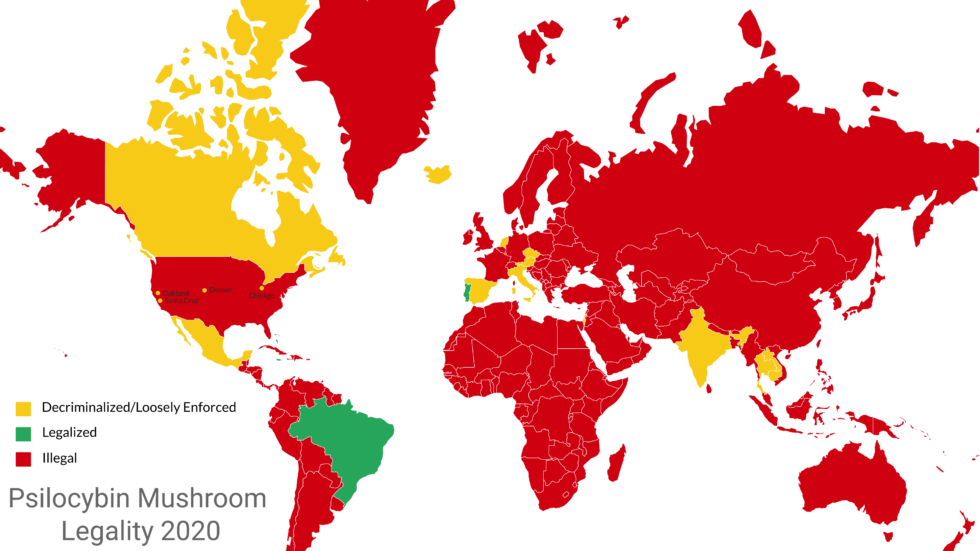
A comprehensive overview of psilocybin legality
Jeff C – February 16, 2020
Psilocybin is the active psychotropic compound found in mushrooms of the Psilocybe genus and a few others, frequently referred to as “magic mushrooms” or “shrooms”. The over 200 species that comprise these genera can be found growing naturally throughout the world on every continent with the exception of Antarctica.
These mushrooms are one of the most commonly known and universally recognized psychedelics – substances that induce a profound altered state of consciousness and are beginning to be recognized for their positive effects on overall mental health, and the symptoms of many psychological conditions. Despite the promising research regarding their safety and efficacy as atreatment for psychological conditions, and their long (not to mention safe) history of use by indigenous peoples, they are illegal in the majority of countries – with a few notable exceptions.
The legality of psilocybin, and the fungi that contain it
Psilocybin (the molecule) and psilocybin-containing fungi are NOT synonymous from a legal perspective. Prohibition of the psilocybin molecule was catalyzed by the UN’s 1971 Convention on Psychotropic Substances, a meeting that aimed to suppress the rising popularity of psychedelic drugs like psilocybin, LSD, and MDMA during the 1960’s.
The convention placed psilocybin in Schedule I, the most restrictive category (defined as having serious risk to public health, with no therapeutic value). However, the convention neglected to precisely define the legality of mushrooms or fungal mycelium containing the substance, and included a clause (Article 32) allowing nations to exempt certain traditional uses of substances from prohibition.
The convention neglecting to ban both psilocybin and psilocybin-containing mushrooms was perhaps an unintentional oversight, and therefore left the decision to prohibit the mushrooms up to member countries, many of whom applied differing legal interpretations and did not outrightly ban the mushrooms (although all agreed to prohibit the compound psilocybin).
This discrepancy has led to multiple loopholes and a confusing double standard that is in need of clarification and rectification, especially now after promising study results regarding the substance. This article serves to address these loopholes, and provide an overview of the current legal status of psilocybin and psilocybin-containing fungi worldwide.
Psilocybin legal status in the United States
The American Psychotropic Substances Act lists psilocybin and psilocybin-containing mushrooms in Schedule I (defined as having a high potential for abuse, no currently accepted medical use in treatment, and a lack of accepted safety for use of the drug under medical supervision) however there are notable exceptions.
It is legal in most states to purchase magic mushroom spores (“for research and microscopy purposes”), and legal to grow them in New Mexico — there is even a recognized religious group in this state which uses the mushrooms for sacramental purposes.
Recently there has been a nationwide push for decriminalization, led by cities such as Denver, Oakland, and Santa Cruz which have all decriminalized the picking and personal possession of psilocybin-containing mushrooms and other entheogenic substances (with the cultivation for commercial purpose and sale of these substances remaining illegal).
Activists in over 100 additional localities have initiated similar measures, while political figures like Andrew Yang and Rep. Alexandria Oscatio-Cortez have also declared support for policy reform around psychedelics.
Psilocybin legal status in Canada
Canada’s laws around psilocybin (the molecule) are mostly congruent with the UN Psychotropic Substances Act, however they classify the substance as schedule III (defined as posing some risks to public health in some situations). The legal landscape surrounding magic mushrooms and psilocybin in Canada (and most other countries) is rather hypocritical, and laws are lightly enforced.
It’s legal to purchase spores and pre-inoculated grow kits, legal to pick and possess fresh psilocybin-containing mushrooms, but illegal to possess dried mushrooms. Laissez-faire enforcement has spurred the creation of many small businesses offering mushrooms and mushroom infused products online. The most publicized case of this being pot activist Dana Larsen’s online Medicinal Mushroom Dispensary — he’s also set to open a storefront in Vancouver Q1 2020).
There is also a clause in the Canadian Controlled Drugs and Substances Act (Section 56) which exempts substances from illegality if medically necessary. A group of therapists in Canada (Thera-psil) have appealed to Health Canada for psilocybin to be exempted from illegality under this clause.
Psilocybin legal status in the United Kingdom
British law regarding the molecule psilocybin is consistent with the UN Psychotropic substances act. However, up until 2005, the possession and even sale of magic mushrooms were fully legal. The Misuse of Drugs Act amendment of 2005 rectified this discrepancy and made the possession, sale, and cultivation of these fungi illegal.
The UK now has more restrictive laws in this area than most other countries — perhaps a rebound effect — with the sale of mushroom spores and inoculated grow kits being illegal as well.
Psilocybin legal status in The Netherlands
Psilocybin (the compound) and magic mushrooms are both illegal in The Netherlands, however many ‘smart shops’ — specialized in ethnobotanical products — profit from one of the most widely known loopholes in the Dutch Drug Misuse Act.
Fungi consist of two main portions, mycelium and fruiting bodies. The Drug Misuse Act lists only the mushrooms as illegal, however it does not include the mycelium of the fungi which also contains psilocybin under certain conditions. Mycelial clumps or “Magic Truffles, along with spores and inoculated grow kits are sold throughout the netherlands.
Read our Amsterdam Travel Guide here!
Psilocybin legal status in Austria
Austria decriminalized the possession of psilocybin-containing mushrooms in January 2016. Offenders caught in possession of personal-use amounts will have to undergo a free therapy program instead of a trial. Cultivation is technically legal as long as the mushrooms are not intended for use as a drug. Grow kits and spores can be legally purchased, however the sale and possession of large amounts of dried magic mushrooms is still illegal.
Psilocybin legal status in Mexico
Both psilocybin and magic mushrooms are illegal in Mexico, however authorities often turn a blind eye to personal use, citing Article 32 of the UN Psychotropic Substances Act which states that exemptions can be made for religious or sacramental use.
Psilocybin legal status in Brazil
Psilocybin (the molecule) is illegal in Brazil, however magic mushrooms are legal to possess, cultivate, and distribute in all forms.
Psilocybin legal status in The British Virgin Islands
Psilocybin (the molecule) is illegal in the BVI, however naturally-occurring magic mushrooms are legal to pick and possess. The sale of psilocybin-containing mushrooms is prohibited, but laws are loosely enforced and they are openly sold throughout the country.
Read our BVI Travel Guide here!
Psilocybin legal status in The Bahamas
Psilocybin (the molecule) and magic mushrooms are fully legal to cultivate, possess, and sell in the Bahamas
Psilocybin legal status in Cambodia
Psilocybin (the molecule) and psilocybin-containing mushrooms are illegal in Cambodia, however laws are loosely enforced, especially in tourist areas.
Psilocybin legal status in the Czech Republic
Psilocybin (the molecule) is illegal in the Czech Republic however magic mushrooms are decriminalized and cultivation is allowed for personal use. Possession of large quantities, and the sale of dried mushrooms, is still illegal but loosely enforced.
Psilocybin legal status in Iceland
Psilocybin (the molecule) and dried magic mushrooms are illegal in Iceland, while picking and possession of fresh mushrooms is allowed.
Psilocybin legal status in India
Psilocybin (the molecule) and magic mushrooms are technically illegal in India. However, the laws are loosely enforced due to many police departments being unaware of the prohibition.
Psilocybin legal status in Israel
Psilocybin (the molecule) and magic mushrooms are illegal in Israel for the purpose of personal use. However, the purchase of spores and inoculated grow kits “for research or microscopy purposes” are allowed.
Psilocybin legal status in Italy
Psilocybin (the molecule) is illegal in Italy. However, magic mushrooms are decriminalized; grow kits and spores are also legal to buy, sell and possess.
Psilocybin legal status in Laos
Psilocybin (the molecule) and magic mushrooms are illegal in Laos. However, laws are loosely enforced, especially in tourist areas.
Psilocybin legal status in Portugal
The Drug policy of Portugal has decriminalized possession of all drugs.
Psilocybin legal status in Samoa
Psilocybin (the molecule) and magic mushrooms are legal in Samoa. However, there are government plans to make both illegal.
Psilocybin legal status in Spain
Psilocybin (the molecule) is illegal in Spain. However, the consumption of magic mushrooms is decriminalized. The cultivation and sale of psilocybin-containing mushrooms is still illegal. The legality of spores and grow kits are ambiguous and prosecution is dependent on intent.
Psilocybin legal status in Thailand
Psilocybin (the molecule) and magic mushrooms are illegal in Thailand. However, laws are loosely enforced, especially in tourist areas.
Psilocybin remains globally illegal
Any country not listed in this article has no ambiguity on the illegality of psilocybin or magic mushrooms in any form (including spores). Hopefully, in light of shifting public sentiment worldwide and promising research, this will soon change. Over the last 20 years (since the first post-drug-war psilocybin study was approved at Johns Hopkins University) the stigma and misinformation around psychedelics have been steadily decreasing.
We believe that within the next 20 years, psilocybin will become both legal and commonplace as a treatment for psychological conditions, and as a tool for personal growth.
Article from – Psillow
Magic mushrooms: UAB studying benefits for addiction and pain
Sarah Whites-Koditschek, al.com
Psychedelic drugs creating hopes for breakthroughs in depression, anxiety, pain and addiction are being tested at UAB. The university is one of a handful in the nation conducting trials with psilocybin, the active ingredient in hallucinogenic mushrooms.
Researchers at the University of Alabama in Birmingham do not know exactly what effect the isolated drug molecules from mushrooms have on the brains of people suffering from such maladies, but studies have shown promising results.
“My own hypothesis is that when, in the right circumstances, someone ingests a classic psychedelic, they experience an emotion we know of as awe,” said UAB’s Dr. Peter Hendricks, professor of public health, who is conducting trials to see whether psilocybin can help people overcome cocaine addiction.
“(Awe) fills you with a feeling of wonder and amazement in this moment, the stimulus, this vast thing outside of your understanding. It captures every ounce of your attention, and because it’s so outside of your understanding of reality, it ultimately requires that you change the way you view reality.”
Nationally, the pharmaceutical industry is ramping up investments in psilocybin in anticipation of eventual FDA approval, and major publications are hypothesizing a “shroom boom” in the United States.
According to Hendricks, psilocybin connects different regions of the brain in new ways, disrupting ruminative thinking in the default mode network, the part of the brain that engages in unfocused activities.
A national movement to legalize psilocybin is gaining momentum.
Oregon legalized the use of psilocybin therapy last year. Denver and Washington, D.C. have decriminalized the drug, and other proposals to legalize or decriminalize it have been put forward in the legislatures of Florida, Maine, Hawaii and California.
Last month, the director of the National Institutes of Health told the U.S. Senate he believes psilocybin holds promise for mental health treatment.
“There has been a resurgence of interest in psychedelic drugs, which for a while were sort of considered not an area that researchers legitimately ought to go after,” said Francis Collins, Director of the National Institutes of Health. “And I think as we’ve learned more about how the brain works, we’ve begun to realize that these are potential tools for research purposes and might be clinically beneficial.”
“I think the support and interest in the scientific community is really growing,” said Hendricks.
There is anthropological research going back tens of thousands of years showing humans have used hallucinogenic mushrooms, said Hendricks.
“I think even the earliest humans realized there’s something about psilocybin, and it’s not just a recreational good time, it’s something else, it’s something much more serious, much more potent, and in fact, in many cases, it was considered quite sacred.”
Psilocybin mushrooms induce a spiritual experience that expands people’s perception of reality and deepens their sense of meaning, said Hendricks. That can help people with ruminative, tunnel focused, obsessive thought processes, hallmarks of depression, anxiety, chronic pain and drug addiction.
“Suddenly your horizons are broadened, and broadened tremendously, and you’re thinking about something other than obtaining or using that drug (or worrying about your pain),” he said.
“It’s as though you’ve taken a step outside of yourself, and you’re able to perhaps see some patterns that you might not have otherwise seen, or you might have some insights you might not have otherwise had when you were in the state of tunnel vision.”
In his research at UAB, Hendricks found such changes appear to have lasting effects.
“Those randomized to receive psilocybin reported significantly fewer days of cocaine use compared to those who were randomized to receive the placebo,” he said about unblinding the first 10 participants in his study on cocaine addiction.
The first wave of exploration into hallucinogenic mushrooms in the United States began in the 1950′s when a New York City banker with a mycology hobby named R. Gordon Wasson traveled to Oaxaca Mexico to try psychedelic mushrooms with an indigenous “curandera”, or healer, named Maria Sabina, Hendricks said.
Wasson published an account of his experience in Life Magazine, setting off a wave of interest in hallucinogenic drugs that included Timothy Leary and Richard Alpert at Harvard, and eventually turned to LSD, a synthetic substance derived from fungus.
“LSD was sort of the primary psychedelic that was studied at a time, and a number of scientists and clinicians and the like were really quite excited. They noticed in themselves and their patients and their participants some pretty profound changes for the better,” said Hendricks.
But that era of experimentation came to an abrupt halt after about a decade, stopping exploration into possible uses for the drugs. Psychedelics were associated with counterculture, the protests against the Vietnam War and the civil rights movement. They came to be perceived as a threat by political leaders like Richard Nixon, said Hendricks.
In 1970 LSD and psilocybin were designated as Schedule 1 substances by the United States Drug Enforcement Agency, a category reserved for the most dangerous and harmful substances with high potential for addiction and abuse. Such a designation limited researchers’ ability to study the therapeutic potential and safety of mushrooms.
Dr. Hendricks said that void of research has begun to be addressed in recent years, as scientists have identified that psilocybin is not addictive and is relatively safe. People can experience “bad trips” on the drug, and it is not advised for those with a family history of schizophrenia because it has been known to precipitate a mental break for people with such a genetic propensity.
Dr. Hendricks decided to seek approval for trials with psilocybin after reading a 2006 landmark paper on the uses of psilocybin for mystical experiences that increase spiritual meaning. At the time, he was observing the failure rate of people trying to quit smoking, about 70 percent.
“My thought was, this could be a game changer. Maybe here’s something that could really boost the effectiveness of our existing treatments. I don’t know for certain, but there’s this really interesting trend here.”
The search for new ways to combat persistent mental health issues is partly a response to a trend of growing psychological problems in the United States, even prior to COVID-19.
In 2018, 19 percent of Americans had a mental health disorder, an increase of 1.5 million over the previous year, according to a study by the group Mental Health America.
Now UAB also plans to test the usefulness of shrooms on people with chronic pain conditions, such as fibromyalgia and opioid addiction.
“It has a very, very, very good safety profile, but like anything, it is not harmless or without risk. It certainly does confer risks,” said Hendricks of psilocybin, “but I myself would be much more concerned about alcohol consumption.”
Go to MSN.com
Why Canada Could Be Next To Allow Psychedelic Therapy (And How It’s Already Changing Lives)
December 30, 2020 – Amanda Siebert – Vices
‘The Unknown Of What Can Happen After You Die Doesn’t Feel So Unknown To Me Anymore’
One of the earliest studies to come out of the so-called psychedelic renaissance was conducted at Johns Hopkins University in 2016, and sought to examine how psilocybin would affect depression and anxiety in patients suffering from life-threatening cancers. It found that just a single dose of psilocybin left subjects with longstanding relief, with 78% experiencing lower rates of depression and 83% experiencing lower rates of anxiety six months after receiving the treatment.
Psychedelic Drug Company MindMed Applies For Nasdaq Up-Listing
Numinus Becomes The First Canadian Psychedelics Company To Legally Harvest Magic Mushrooms
Holiday Gift Guide 2020: What To Buy The Psychonaut On Your List
When Thomas Hartle, a 52-year-old Saskatoon resident with stage four colon cancer read the results of the study, he says he “felt like they were too good to be true.”
“But when you suffer from anxiety, you really look for whatever sources of relief you can get,” he says. Hartle enlisted the help of TheraPsil, a non-profit organization based in Victoria, B.C., to try and access psilocybin therapy for himself. Using a subsection of the Controlled Drugs and Substances Act that allows the health minister to grant an exemption for medical or scientific purposes, TheraPsil has so far assisted dozens of Canadians, including terminally ill and clinically depressed patients, as well as doctors and therapists, in the application process.
In August 2020, Health Minister Patty Hajdu granted the first exemptions to four Canadians suffering from end-of-life anxiety. One of them was Hartle.
The father, husband, and IT technician says his anxiety is “specialized to the existential kind and doesn’t extend to public speaking,” so he’s more than happy to share his experiences with psilocybin. Before his first treatment, he prepared extensively with a therapist, and has since undergone a subsequent session. Without hesitation, he says the experiences have changed his perspective on death and dying.
“What it’s changed the most for me, is that the unknown of what can happen after you die doesn’t feel so unknown to me anymore. Most of how we define ourselves is our experiences and memories and things like that. In the psilocybin experience, my consciousness existed in ways that had absolutely nothing to do with anything in this life,” he says.
“To exist in another state that has nothing to do with my identity here, and to feel comfortable and serene in that state tells me that it’s possible to have some sort of continuation of consciousness that goes beyond our experience here.”
Hartle adds he feels more empathy towards other people since his initial treatment, and says his family has noticed he uses more emotional words in his speech. As a naturally analytical thinker, he says he’s also welcomed a shift to a more creative mindset.
Beyond the positive mental benefits he’s experienced, Hartle says psilocybin also helps to relieve pain associated with migraines, which he’s suffered from since he was a child. “When I compare it to most of the other treatments that I have gone through over the last few years, psilocybin is like the opposite of side effects,” he says, laughing.
Doctors Can Access Psilocybin, Too
Dr. Emma Hapke is TheraPsil’s co-chair of research and one of 16 doctors, nurses, therapists and social workers recently granted exemptions to take psilocybin in preparation for work with patients. She is part of a committee at TheraPsil developing a training program for psychedelic assisted psychotherapy, which she hopes to kick off in 2021.
“We feel that it’s essential that therapists themselves have their own experiences in a non-ordinary state of consciousness, to be on the receiving end of that type of therapy so they can then guide others to do the same,” she says.
She emphasizes that while psychedelic substances have been shown to provide benefit for people suffering from an array of mental health conditions, it’s imperative that any psychedelic experience be paired with therapy for maximum and longstanding relief.
“The molecule in and of itself isn’t what’s healing—it’s the whole package of being in a healing relationship with a therapist and going into the non-ordinary state with psilocybin to access different parts of the psyche,” she says. “If the experience is not integrated, it’s hard for it to lead to lasting change, and so it’s really important that we’re not just talking about a psychedelic. We’re talking about psychedelic-assisted therapy.”
Spencer Hawkswell, TheraPsil’s CEO, says before August 4, seeking exemptions for terminally ill patients felt like an uphill battle. Today the mood has changed, and there is a greater sense of optimism among his team.
“I never thought I’d say that it was easy, or that Health Canada has been incredibly cooperative,” he says. “These [patients] are empowered Canadians, and we do have rights and systems that work for them. Just to have that affirmation is pretty amazing.”
Recognizing the utilitarian nature of Canada’s approach to mental healthcare and drug policy, Hawkswell says that while the current system tries to meet the needs of most, it falls short. “What TheraPsil is doing is showing that there are options beyond the current policy regulations and the norm of healthcare in Canada.”
Numinus Advocates For Special Access Program Reform
Health Canada’s Special Access Program (SAP) allows healthcare professionals to request restricted or otherwise unavailable drugs for patients who have tried existing treatments and found them to be unsuccessful. In theory, the SAP should allow doctors to request access to drugs like psilocybin, MDMA, and LSD. That changed in 2013, when under Conservative Prime Minister Stephen Harper, accessing restricted drugs through the SAP was prohibited. Since then, the only way for patients to access such substances is through clinical trials.
On December 12, Health Canada announced its intention to reverse the regulatory changes made in 2013, and initiated a 60-day comment period seeking public feedback. Dr. Evan Wood, chief medical officer at Numinus, has been advocating for changes to the program since early 2019.
Wood says by amending the SAP provision on restricted drugs, Health Canada will better align itself with the Helsinki Declaration, a set of international ethical guidelines that suggest (among other things) if a patient accesses a restricted drug through a clinical trial and finds it to be beneficial, they should be entitled to receive ongoing therapy. Currently, if a Canadian were to access a psychedelic substance or another restricted drug though a clinical trial, even with the support of a physician, they would not be able to continue to access it.
“In my view, it’s really just about stigma and the cultural baggage associated with these molecules,” Wood says. “This is bringing Canada in compliance with those international ethical guidelines, and kicking the door open a crack for Canada to be a real world leader in this area.”
While Wood acknowledges that the Covid-19 pandemic has rightfully taken the majority of Health Canada’s attention in 2020, he’s glad to see that psychedelic-assisted psychotherapy has risen to an area of needed focus, and gives full credit to the agency for proposing the regulatory reversal.
If the change to the SAP is made, Wood says access to novel psychedelic treatment has the potential to increase significantly, as interested patients would simply need to find a doctor willing to apply for access to the drug on their behalf. Applications would then be judged on an individual basis, but would be less arduous than applying for an individual Section 56 exemption, and perhaps even eliminate the need for that process entirely.
For companies like Numinus, Wood says the changes would enable them to better establish the physical infrastructure of their businesses, to train staff, and “to do all of the things that are necessary to do this kind of work safely.”
“When you put the known risks alongside the known safety of these substances, it’s a bit of a no brainer,” he says. “It’s not going to be a cure for everybody, but even to be talking about a ‘cure’ in the context of mental health challenges is a total paradigm shift.”
Some might argue that decriminalization is the obvious next step, however Health Canada isn’t alluding to that just yet. In an email, a spokesperson for Minister Hajdu said the agency “thoroughly reviews all requests for exemption and makes decisions after taking into account the risks and benefits.”
“We still have much to learn about the risks, which is why the sale and possession of psilocybin is still illegal. Until there is a sufficient evidence base, Health Canada will review each request for an exemption on a case-by-case basis.”
Article from – Forbes.com
Important Update from TheraPsil
Dear Friends of TheraPsil, the Government of Canada and the Canadian Public,
At TheraPsil, our primary mission is to help Canadians in medical need, access psilocybin therapy. Since August 4th, 2020, we have successfully supported 13 individuals across Canada who are now legally allowed to access psilocybin therapy through section 56 exemptions.
While TheraPsil has been focused on advocating for Palliative Canadians, we have also, unofficially, begun advocating to help a broader class of patients such as those who struggle with psychological trauma that can often cause symptoms such as depression and anxiety.
On October 4th, 2020, the first non-palliative Canadian was granted access to psilocybin by way of a section 56 exemption, to treat her unresolved trauma. On November 5th, 2020, this patient was successfully treated with psilocybin therapy by psychotherapist, TheraPsil’s founder, Dr. Bruce Tobin.
“Everyone has trauma, some experience it when we are small and absorb it and it sits in us as we mature into adults. Because of the traumas of my past, I have struggled with anxiety, depression, and addiction for years. During my psilocybin therapy, I went deep, way back to when I was a little girl, and all those things that happened to me. All the unresolved trauma, it came back and I was beyond terrified, shaking uncontrollably and crying, however with my therapist Dr. Tobin, I conquered those tough memories and after a while I realized…. I ain’t scared of Jack S**t….For the first time, I feel like I have won the battle in my mind and my anxiety and depression seem to be gone. The memories are not, but now I know they can’t hurt me.”
– Mona Streleaff, British Columbia, Canada’s First Non-Palliative Canadian to Access Legal Psilocybin Therapy
Mona’s exemption represents a historic moment in Canada and a groundbreaking progressive decision by Health Canada to broaden the class of patients who can access this treatment option, thus further enshrining the rights of Canadians.
While this is excellent news and represents a wealth of opportunities for the future of mental healthcare in Canada, it also represents an equal amount of challenges. TheraPsil has been backed-up with requests for support from patients, both palliative and non-palliative, since the initial August 4th decision, who are seeking access to legal psilocybin therapy. As a small, non-profit organization we need support to keep up with the anticipated increase in patient demand so we can facilitate an expanded mandate that upholds our high standards and protects the integrity of our process.
As such, in response to Health Canada’s groundbreaking decision to grant a section 56 exemption for one non-palliative individual, TheraPsil is seeking to fundraise. We will soon be launching a GoFundMe campaign with a goal to raise $250’000. We have already secured a generous donor who is willing to match with an additional $250’000 to reach our initial fundraising goal of $500’000, by December 31, 2020.
Part of the support we need is human resources and this is where we plan to dedicate most of the funds raised. We need nurses and physicians who can triage patients to ensure we are facilitating safe and equitable access to legal psilocybin therapy. We also need funding to help complete and launch our psilocybin therapy training program for Canadian clinicians, with an aim to roll out this program by January 1st 2021. If we are successful in our current advocacy campaign, clinicians and healthcare professionals will be granted section 56 exemptions by the end of this month, for training purposes. TheraPsil’s training program aims to be the first legal training program in Canada to offer experiential training – where trainees take psilocybin mushrooms and enter this non-ordinary state of consciousness first-hand.
Although one non-palliative individual has been granted access to psilocybin therapy, and we have been eager to share this with you all, we must be transparent about our current bandwidth and ability to support more non-palliative individuals, like Mona, at this time.
Unfortunately, at the current moment, we do not have the resources to broaden our inclusion criteria, and for the near future, we will remain open to only supporting palliative Canadians, those with a terminal illness or those in remission from a life-threatening illness (i.e Cancer survivors) who suffer from end-of-life distress, as our website indicates. We are a patient-first organization and in order to maintain the integrity of our process and maintain the high standards of support we provide to patients, we must ensure we expand our services in accordance with our means and ability to provide safe and equitable care.
However, rest assured, our full intention is that through meeting our fundraising goal, we will soon be able to announce new patient inclusion criteria and broaden access so we can support more Canadians, like Mona, who suffer from complex trauma and various mental health conditions and symptoms.
We are so grateful for the support of the psychedelic community, the Federal Government, many Canadian MP’s, the patients we have supported, our small but mighty clinical and operations team, and the hundreds of Canadians who have advocated alongside us. Your support has allowed us to get this far and there is so much work to still be done! Every small step forward and every patient who is granted an exemption, is a win for compassionate access and we are deeply dedicated to continuing the pursuit of our four pillar mission, for the benefit of all Canadians:
- COMPASSIONATE ACCESS: Establish safe, compassionate, and legal access to psychedelic-assisted therapy for those in medical need.
- PUBLIC EDUCATION: Increase awareness of the general public and health care professionals about the merits and limitations of psychedelic-assisted therapy.
- PROFESSIONAL TRAINING: Developing safe, simple, and effective protocols for credentialed health professionals across Canada to deliver psilocybin-assisted therapy, in collaboration with other active organizations.
- RESEARCH: Facilitate research and evaluation, in collaboration with Canadian and international partners.
Please stay tuned for updates by following us on Twitter and signing up for our newsletter so you can be informed when we launch our GoFundMe and have broadened our patient inclusion criteria.
If you meet our current criteria, please continue to contact us for support. We are here to help and want to hear from you.
To Psilocybin Therapy,
– Spencer Hawkswell, CEO of TheraPsil & The TheraPsil Coalition
UPDATE from TherPsil
Patient Spotlight: Alison Myrden
psilochancellor –
My name is Alison Myrden; I am a retired law enforcement officer, one of Canada’s 1st legally licensed medical cannabis patients from 1994, a global drug law reform activist and the world’s 1st legally authorized medical psilocybin patient for pain (in 2017). Here is a brief look at the journey of my natural health regime over the last 30+ years so that you, too, are informed in all things natural being studied around the world as medicine.
Let us talk Psilocybin – my fight has always been for all of us. Especially for those who choose to consume illicit substances for ANY reason; social, religious, or medical. We all deserve the opportunity to choose. From my experience, psilocybin or magic mushrooms are safer than cannabis; I PROMISE.
My battle for natural medicine began when I was in my early 20s due to the indication of being formally diagnosed with Primary Progressive Multiple Sclerosis at 28 years old. Then, fighting a violent pain located in both the left side of my head and face, which was diagnosed as Cluster Headaches and soon changed to Trigeminal Neuralgia. Described as “The worst pain known to medicine,” for reference on the excruciating scale. A few years later, my diagnosis was again changed, to Bilateral Trigeminal Neuralgia. My pain had then escalated to both sides of my face and head, now occurring 24 hours a day.
By my mid 20s (the 1980s), I was having an exceedingly difficult time finding anything anywhere to give me adequate relief. I had been given every medication known to the Canadian Pharmacopoeia by doctors for my illnesses when I was young and had reached out to doctors / scientists around the world for help being that pills were not helping me manage whatsoever. 32 pills, heroin, cocaine and 2,000mg of morphine daily for almost two decades – all doctor authorized and prescribed. I was consuming substances such as cannabis and psilocybin the entire time over the years, while reducing all those pharmaceuticals and learning with the assistance of doctors and scientists whom I met along the way. This arm’s length guidance taught me how to indulge in these nature-born meds safely and properly; both are extremely important.
Luckily, I also had several college courses under my belt which included pharmacology, anatomy, and physiology. I also acquired knowledge of appropriate harm reduction techniques involving issues of overdose. I started consuming psilocybin over 35 years ago, for fun. This changed quickly as I started taking psilocybin for pain relief because the cannabis, all the pills and everything else I was medicating with at the time were not helping the same way with the violent bouts of pain via my condition at that point. One night, when I just could not take the pain anymore – my girlfriend, the hostess of a party I attended, immediately brought me some “special” tea.
Little did I know, that was my 1st experience using psilocybin for the brutal neurological pain I was experiencing; the pain was astonishingly gone in minutes. I am living proof that macrodosing does indeed work! The energy psilocybin delivered to my body was unreal, no wonder they call the compound “magic,”. I will never forget the day I was at a federally licensed cannabis patient’s home when the vicious pain in my face came washing over. As luck would have it, this patient offered me 5 grams of “Blue Cambodian” psilocybin mushrooms. I ate all 5 grams and somehow, my pain was completely gone for the first time EVER – for almost five hours.
I was so desperate for relief and knew already the lethal overdose and toxicity levels were the lowest for psilocybin than for any other illicit substance. I returned to my neurologist the following week for “the world’s 1st authorization of psilocybin for excruciating pain” treatment ~ drinking and/or eating 50-60 grams of dried psilocybin a day; from April 3rd, 2017 til today. From my original consumption of 1 to 2 grams of dried psilocybin in tea and chocolate to 5 grams of dried psilocybin every two hours, the last 32 years has led me on a very magical journey.
Remember…I have had this silly pain 24 hours a day for over thirty years until 2017, when psilocybin changed my life for the better!”
#JoinTheJourney
Respectfully,
Alison Myrden
Retired Law Enforcement Officer
Global Drug Law Reform Activist
Federal Medical Cannabis Exemptee in Canada since 1994
http://www.AlisonMyrden.com/
Canadian Patient Representative for the IACM
International Association for Cannabinoid Medicines
http://www.cannabis-med.org/
Bonn, Germany
NDP Candidate for Oakville, Ontario 2004
New Democratic Party of Canada
http://www.ndp.ca/
Article From – Psilocybin Academy
UC Berkeley launches new center for psychedelic science and education
Yasmin Anwar –
Fifty years after political and cultural winds slammed shut the doors on psychedelic research, UC Berkeley is making up for lost time by launching the campus’s first center for psychedelic science and public education.
With $1.25 million in seed funding from an anonymous donor, the new UC Berkeley Center for the Science of Psychedelics will conduct research using psychedelics to investigate cognition, perception and emotion and their biological bases in the human brain.
The center is also developing a program for educating the public about this rapidly advancing field of research. Initial experimental studies will use psilocybin, the principal psychoactive compound in magic mushrooms.
“There’s never been a better time to start a center like this,” said UC Berkeley neuroscientist David Presti, one of the center’s founding members. “The renewal of basic and clinical science with psychedelics has catalyzed interest among many people.”
“We’re really interested in what psychedelics can teach us about consciousness, perception, creativity and learning,” said Pollan, who felt compelled to explore psychedelics in late middle age, instead of in his youth, and write about them.Other acclaimed co-founders of the center include psychologist Dacher Keltner, who studies the mental and physiological benefits of awe, and journalism professor Michael Pollan, whose 2018 bestseller, How to Change Your Mind: What the New Science of Psychedelics Teaches Us About Consciousness, Dying, Addiction, Depression and Transcendence, was one of the inspirations for the center.
“Psychedelics have a particular value later in life, because that is when you are most stuck in your patterns. They give you the ability to shake them loose,” he said.
The minds they are a-changin’
Research at the new center will complement ongoing clinical studies at other institutions — such as Johns Hopkins University in Maryland and Imperial College London — that are integrating psilocybin and other psychedelic compounds with psychotherapy to treat mental disorders, such as anxiety, depression, post-traumatic stress disorder and substance abuse.
“Some of these studies have produced striking results in cases that are otherwise resistant to more conventional medical treatment. This suggests that psychedelic compounds may offer new hope for people suffering from these disorders,” said UC Berkeley neuroscientist Michael Silver, inaugural director of the UC Berkeley Center for the Science of Psychedelics.
Yet, much remains unknown about the brain mechanisms behind the efficacy of psychedelic compounds in treating mental health disorders. Also poorly understood is the ability of these compounds to improve cognitive flexibility, alter visual perception, engender feelings of awe and change patterns of brain activity.
Addressing these questions will be a major part of the research at the UC Berkeley Center for the Science of Psychedelics, which will focus on healthy study participants, Silver said.
Over time, and with more funding, Silver’s hope is that researchers at Berkeley and other institutions will study psychedelics as part of the center’s activities not just in relation to psychology and neuroscience, but also philosophy, religion, anthropology, art, and even computer science and artificial intelligence.
“This is a pivotal time in history for a discussion about psychedelics and under what circumstances they should be used,” he said. “This has obviously been a very polarizing topic, but I think people’s minds are changing.”
Training psychedelic guides
One unique aspect of the new center is its emphasis on public education. It will produce a website offering rigorously vetted original and curated content covering scientific, political, business and cultural developments in psychedelics, Pollan said.
The center’s plan to explore ways of supporting healthy volunteer research participants as they undergo psychedelic experiences in the center’s studies is unique, too.
To do this, the center plans to collaborate with the Graduate Theological Union, an independent consortium of religious schools and theological institutes based in Berkeley and the larger San Francisco Bay Area, in the development of an immersive learning program on psychedelics and spirituality.
This program will eventually train guides, also known as facilitators, in the cultural, contemplative and spiritual care dimensions of psychedelics, working in partnership with the UC Berkeley Center for the Science of Psychedelics research studies. Given the rapidly growing number of psychedelic research studies, there are not enough trained facilitators to meet the demand, the center’s founders said.
“The training of facilitators is an indispensable part of this project,” said Sam Shonkoff, an assistant professor of Jewish studies at the Graduate Theological Union who is collaborating with the center.
Brian Anderson, a UCSF psychiatrist, and Celina De Leon, who has a master’s degree in divinity from the Graduate Theological Union, both have expertise in the ritual use of psychedelic plants and are involved in creating an immersive learning program for research participants and designing the training program.
Ancient healing precedes modern science
While hallucinogenic plants and fungi have been used for millennia in ceremonial rituals, they were not known to Western medical science until the late 19th century.
In 1938, Swiss chemist Albert Hofmann synthesized lysergic acid diethylamide (LSD) while investigating potential new pharmaceutical medications, and he discovered LSD’s mind-altering effects in 1943. Samples were sent to medical centers and universities worldwide to promote research into its possible benefits.
In 1966, states began to ban hallucinogens, and when the Federal Controlled Substances Act was implemented in 1971, LSD and other psychedelic drugs were classified as Schedule I controlled substances, and studies of their use in human subjects essentially ground to a halt that lasted until the recent renaissance.
“Together with societal changes during the 1960s, psychedelic drugs made people ask questions about the status quo and were seen as a destabilizing force, and the backlash to that suppressed psychedelic research with human subjects for decades,” Silver said.
More recently, psilocybin, LSD and dimethyltryptamine, a key psychoactive component of the ayahuasca brew, have received renewed attention, both in research settings and in society at large, along with MDMA (ecstasy) and ketamine.
Future investigations will include studying the neural mechanisms of visual hallucinations to better understand how the brain constructs our perception of the world around us, comparing psychedelic and non-psychedelic mystical-type experiences and measuring the long-lasting effects of psychedelic experiences on social and political attitudes, identity and resilience to stress.At the center, researchers will focus on the use of these ancient compounds to explore the unplumbed depths of the mind and to shed light on how these molecules can improve mental health.
“Psychedelic medicines can open a doorway to seeing one’s psyche and connection with the world in new and helpful ways,” Presti said. “That’s been appreciated by shamanic traditions for thousands of years. Science is now exploring new ways to investigate this.”
Story from Berkley News
Psilocybin Sessions: Psychedelics could help people with addiction and anxiety
Anderson Cooper – August 16, 2020
Study participants at some of the country’s leading medical research centers are going through intense therapy and six-hour psychedelic journeys deep into their minds to do things like quit smoking and worry less.
For most of us, psychedelic drugs conjure up images of the 1960’s – hippies tripping out on LSD or magic mushrooms. But, as we reported last fall, these powerful, mind-altering substances are now being studied seriously by scientists inside some of the country’s foremost medical research centers. They’re being used to treat depression, anxiety and addiction…
And early results are impressive, as are the experiences of the studies’ volunteers who go on a six-hour, sometimes terrifying, but often life-changing psychedelic journey deep into their own minds.
Carine McLaughlin: (LAUGH) People ask me, “Do you wanna do it again?” I say, “Hell no. I don’t wanna go do that again.”
Anderson Cooper: It was really that bad?
Carine McLaughlin: Oh, it was awful. The entire time, other than the very end and the very beginning, I was crying.
Carine McLaughlin is talking about the hallucinogenic experience she had here at Johns Hopkins University, after being given a large dose of psilocybin, the psychedelic agent in magic mushrooms, as part of an ongoing clinical trial.
Roland Griffiths: We tell people that their experiences may vary from very positive to transcendent and lovely to literally hell realm experiences.
Anderson Cooper: Hell realm?
Roland Griffiths: As frightening an experience as you have ever had in your life.
That’s scientist Roland Griffiths. For nearly two decades now, he and his colleague Matthew Johnson have been giving what they call “heroic doses” of psilocybin to more than 350 volunteers, many struggling with addiction, depression and anxiety.
Anderson Cooper: Can you tell who is going to have a bad experience, who’s gonna have a transcendent experience?
Roland Griffiths: Our ability to predict that is almost none at all.
Anderson Cooper: Really?
Matthew Johnson: About a third will– at our– at a high dose say that they have something like that, what folks would call a bad trip. But most of those folks will actually say that that was key to the experience.
Carine McLaughlin was a smoker for 46 years and said she tried everything to quit before being given psilocybin at Johns Hopkins last year. Psilocybin itself is non-addictive.
Anderson Cooper: Do you remember what, like, specifically what you were seeing or?
Carine McLaughlin: Yes. The ceiling of this room were clouds, like, heavy rain clouds. And gradually they were lowering. And I thought I was gonna suffocate from the clouds.
That was more than a year ago; she says she hasn’t smoked since. The study she took part in is still ongoing, but in an earlier, small study of just 15 long-term smokers, 80% had quit six months after taking psilocybin. That’s double the rate of any over-the-counter smoking cessation product.
Roland Griffiths: They come to a profound shift of world view. And essentially, a shift in sense of self that I think–
Anderson Cooper: They– they see their life in a different way?
Roland Griffiths: Their world view changes and– and they are less identified with that self-narrative. People might use the term “ego.” And that creates this sense of freedom.
And not just with smokers.
Jon Kostakopoulos: Beer usually, cocktails, usually vodka sodas, tequila sodas, scotch and sodas.
Jon Kostakopoulos was drinking a staggering 20 cocktails a night and had been warned he was slowly killing himself when he decided to enroll in another psilocybin trial at New York University. During one psilocybin session, he was flooded with powerful feelings and images from his past.
Jon Kostakopoulos: Stuff would come up that I haven’t thought of since they happened.
Anderson Cooper: So old memories that you hadn’t even remembered came back to you?
Jon Kostakopoulos: I felt, you know, a lot of shame and embarrassment throughout one of the sessions about my drinking and how bad I felt for my parents to put up with all this.
He took psilocybin in 2016. He says he hasn’t had a drink since.
Anderson Cooper: Do you ever have a day where you wake up and you’re like, man, I wish I could have a vodka right now or beer?
Jon Kostakopoulos: Never.
Anderson Cooper: Not at all?
Jon Kostakopoulos: Not at all, which is the craziest thing because that was my favorite thing to do.
Using psychedelic drugs in therapy is not new. There were hundreds of scientific studies done on a similar compound – LSD – in the 1950’s and 60’s. It was tested on more than 40,000 people, some in controlled therapeutic settings like this one. But there were also abuses. The U.S. military and CIA experimented with LSD sometimes without patients knowledge.
Fear over rampant drug use and the spread of the counterculture movement, not to mention Harvard professor Timothy Leary urging people to turn on, tune in and drop out, led to a clamp down.
In 1970, President Richard Nixon signed the controlled substances act and nearly all scientific research in the U.S. Into the effects of psychedelics on people stopped. It wasn’t until 2000 that scientist Roland Griffiths won FDA approval to study psilocybin.
Roland Griffiths: This whole area of research has been in the deep freeze for 25 or 30 years. And so as a scientist, sometimes I feel like Rip Van Winkle.
Anderson Cooper: And once you saw the results…
Roland Griffiths: Yeah. The red light started flashing. This is extraordinarily interesting. It’s unprecedented and the capacity of the human organism to change. It just was astounding.
Anderson Cooper: It sounds like you are endorsing this for everybody.
Roland Griffiths: Yeah, let’s be really clear on that. We are very aware of the risks, and would not recommend that people simply go out and do this.
Griffiths and Johnson screen out people with psychotic disorders or with close relatives who have had schizophrenia or bipolar disorder. Study volunteers at Johns Hopkins are given weeks of intensive counseling before and after the six-hour psilocybin experience; the psilocybin is given in a carefully controlled setting one to three times. To date, they say there’s not been a single serious adverse outcome.
We were told we couldn’t record anyone participating in the study while they were on psilocybin because it might impact their experience, but we were shown how it begins – without the psilocybin.
You lay on a couch, with a blindfold to shut out distractions and headphones playing a mix of choral and classical music – a psychedelic soundtrack with a trained guide, mary cosimano, watching over you.
Everything is done the same way it was for the LSD experiments scientists conducted in the 1950s and 60s. Some of the most dramatic results have been with terminal cancer patients struggling with anxiety and paralyzing depression.
Kerry Pappas: I start seeing the colors and the geometric designs and it’s like ‘oh this is so cool, and how lovely’ and, and then, boom. Visions began.
Kerry Pappas was diagnosed with stage III lung cancer in 2013. During her psilocybin session, she found herself trapped in a nightmare her mind created.
Kerry Pappas: An ancient, prehistoric, barren land. And there’s these men with pickaxes, just slamming on the rocks. So…
Anderson Cooper: And this felt absolutely real to you?
Kerry Pappas: Absolutely real. I was being shown the truth of reality. Life is meaningless, we have no purpose. And then I look and I’m still like a witness, a beautiful, shimmering, bright jewel. And then it was sound, and it was booming, booming, booming. Right here right now.
Anderson Cooper: That was being said?
Kerry Pappas: Yes. “You are alive. Right here right now, because that’s all you have.” And that is my mantra to this day.
Michael Pollan: It seemed so implausible to me that a single experience caused by a molecule, right, ingested in your body could transform your outlook on something as profound as death. That’s– that’s kind of amazing.
Author Michael Pollan wrote about the psilocybin studies in a bestselling book called “How to Change Your Mind.” As part of his research, he tried psilocybin himself with the help of an underground guide.
Anderson Cooper: The kind of things that cancer patients were saying, like, “I touched the face of God.” You were skeptical about when you hear phrases like that?
Michael Pollan: Yeah. Or, “Love is the most important thing in the universe.” When someone tells me that I’m just like, “yeah, okay.”
Anderson Cooper: So you don’t go for some of the phrases that are used?
Michael Pollan: No. It gives me the willies as a writer. And I really struggled with that cause during one of my experiences I came to the earth-shattering conclusion that love is the most important thing in the universe. But it’s, that’s Hallmark card stuff, right? And um, so…
Anderson Cooper: And yet while you were on it and afterward…
Michael Pollan: It was profoundly true. And it is profoundly true. Guess what? Um…
Anderson Cooper: There’s a reason it’s on a Hallmark card.
Michael Pollan: There is a reason. And one of the things psychedelics do is they peel away all those essentially protective levels of irony and, and cynicism that we, that we acquire as we get older and you’re back to those kind of “Oh, my God. I forgot all about love.” (Laugh)
Pollan said he also experienced what the researchers describe as ego loss, or identity loss – the quieting of the constant voice we all have in our heads.
Michael Pollan: I did have this experience of seeing my ego– burst into– a little cloud of Post-It notes. I know it sounds crazy.
Anderson Cooper: And what are you are without an ego?
Michael Pollan: You’re, uh… (Laugh) You had to be there.
Researchers believe that sensation of identity loss occurs because psilocybin quiets these two areas of the brain that normally communicate with each other. They’re part of a region called the default mode network and it’s especially active when we’re thinking about ourselves and our lives.
Michael Pollan: And it’s where you connect what happens in your life to the story of who you are.
Anderson Cooper: We all develop a story over time about what our past was like and who we are.
Michael Pollan: Right. Yeah, what kind of person we are. How we react. And the fact is that interesting things happen when the self goes quiet in the brain, including this rewiring that happens.
To see that rewiring, Johns Hopkins scientist Matthew Johnson showed us this representational chart of brain activity. The circle on the left shows normal communication between parts of the brain, on the right, what happens on psilocybin. There’s an explosion of connections or crosstalk between areas of the brain that don’t normally communicate.
Anderson Cooper: The difference is just startling.
Matthew Johnson: Right.
Anderson Cooper: Is that why people are having experiences of– seeing you know, repressed memories, or past memories, or people who have died or?
Matthew Johnson: That’s what we think. And even the perceptual effect, sometimes the synesthesia, like, the– the seeing sound.
Anderson Cooper: People see sound?
Matthew Johnson: Yeah, sometimes.
Anderson Cooper: I– I don’t even know what that means.
Matthew Johnson: Right, yeah. (LAUGH) It’s– it’s–
Michael Pollan: Maybe the ego is one character among many in your mind. And you don’t necessarily have to listen to that voice that’s chattering at you and criticizing you and telling you what to do. And that’s very freeing.
It was certainly freeing for Kerry Pappas. Though her cancer has now spread to her brain, her crippling anxiety about death is gone.
Kerry Pappas: Yeah, it’s amazing. I mean, I feel like death doesn’t frighten me. Living doesn’t frighten me. I don’t frighten me. This frightens me.
Anderson Cooper: This interview frightens you, but death doesn’t?
Kerry Pappas: No.
It turns out most of the 51 cancer patients in the Johns Hopkins study experienced “significant decreases in depressed mood and anxiety” after trying psilocybin. Two-thirds of them rated their psilocybin sessions as among the most meaningful experiences of their lives. For some, it was on par with the birth of their children.
Kerry Pappas: To this day, it evolves in me.
Anderson Cooper: It’s still alive in you–
Kerry Pappas: It’s still absolutely alive in me.
Anderson Cooper: Does it make you happier?
Kerry Pappas: Yeah. And– and I don’t necessarily use the word happy.
Kerry Pappas: Comfortable. Like, comfortable. I mean, I’ve suffered from anxiety my whole life. I’m comfortable. That, to me, okay. I can die. I’m comfortable. (LAUGH) I mean, it’s huge. It’s huge.
Story from 60 Minutes
The first Canadian to legally consume psilocybin for medical purposes shares his experience
“I had some ideas about what I thought I would get out of this, but the actual feelings and experience of it are so much better.”
By Sam Riches – August 21, 2020
On the night that Thomas Hartle became the first Canadian to legally consume psilocybin for medical purposes, Dr. Bruce Tobin, a psychotherapist and professor at the University of Victoria, shared a cab with filmmaker Randall “Peg” Peters.
The two men, along with John Simpson, a hospice companion and sitter, had spent the day with Hartle as he went through his first therapeutic dosing experience in the guest bedroom of his Saskatoon home.
Peters wasn’t sure if what had transpired over the previous six hours was a success. In the cab, he expressed his concerns to Dr. Tobin that perhaps Hartle hadn’t benefited in any significant way, but the doctor reassured him. “It’s like good tea,” he said. “You just need to let it steep.”
That night, back at the Hartle household, Hartle enjoyed the best sleep he’s had since receiving his terminal cancer diagnosis four years ago. In the week that has passed since that dose, Hartle hasn’t had a single anxiety attack, he said, a personal record.
- A Saskatoon dad in palliative care is still waiting to find out if he can legally use psilocybin for mental health
- Four Canadians receive medical exemptions for psilocybin therapy
- Forget taking a pill a day. Canada is using psychedelics to revolutionize the way we treat mental health and addiction
“I have had anxiety for so long, I had sort of forgotten what it feels like to not have it,” Hartle said during a webinar Thursday evening, speaking publicly about his experience for the first time. “To experience the lack of anxiety I have had this week is beyond words. It’s amazing. I have no idea how long this particular benefit will last, but so long as it’s here, it’s really, really amazing and good.”
Hartle, a father of two and an IT professional of 25 years, had never taken psilocybin — a psychedelic drug derived from magic mushrooms — in his life. He previously told The GrowthOp that he was interested in pursuing psilocybin therapy as a means to address the existential anxiety that accompanies living with a terminal diagnosis, something that traditional anti-anxiety medications don’t treat.
Hartle went through several preparatory sessions before consuming the dose, to best learn how the process would work and to form a relationship with the doctors and those involved. “Before this experience, I had some ideas about what I thought I would get out of this, but the actual feelings and experience of it are so much better,” he said during the webinar.
“I would highly recommend that Canadians consider it as an option. The psilocybin, for me, was very gentle and effective. Even if I didn’t have any more effects tomorrow, I would feel very comfortable having another session to boost it back up, and, worst case, that would still be only a single dose once a week — there isn’t any other medication out there that has that sort of efficacy.”
Earlier this month, four Canadians received Section 56 exemption to the Controlled Drugs and Substances Act, allowing them to pursue psilocybin therapy for end-of-life distress. The exemptions were granted by federal health minister Patty Hajdu, and the applications were completed with the help of TheraPsil, a B.C.-based, non-profit organization founded by Dr. Tobin and made up of a coalition of healthcare professions, researchers, advocates and policymakers.
For Dr. Tobin, Hartle’s experience is in line with research about the therapeutic benefits of psychedelics from institutions such as John Hopkins, Yale University and the University of Toronto. Multiple studies indicate that psilocybin can lead to significant and sustained decreases in depression and anxiety in patients with life-threatening cancer.
“A fundamental dynamic in this healing potential of psilocybin is that it allows our ego self to temporarily relax the grip of our negative and pain-producing belief systems, to relax and let go of that grip on our sense of who we are and what’s really important and what living is all about,” Dr. Tobin said. “With this relaxation of old habits of thinking, new perspectives and attitudes and assumptions are possible, leading to new possibilities for being in the world with our disease.”
Even with the four exemptions that have been granted, psilocybin remains a restricted medicine, making it illegal for doctors to use psilocybin as part of their training. Dr. Tobin emphasized that needs to change and that the organization will be working hard in the months ahead to fight for therapists to have legal access to psilocybin for training purposes.
“That (restriction) doesn’t really make any sense to any of us,” Dr. Tobin said during the webinar. “Imagine what it would be like to go to a sex therapist who you know has never had sex.”
Within the next few years, Dr. Tobin said he expects that “the face of Canadian psychiatry and clinical psychology is going to be transformed by these psychedelic medicines.” The organization is encouraging interested Canadians who believe they might benefit from psilocybin therapy to contact them.
Psychiatrist Dr. Crosbie Watler, former chief of psychiatry at Kenora, Ont.’s Lake of the Woods District Hospital, called Hartle’s experience “a call to action.”
“I’ve been despairing because I see the treadmill of care, but I also see that people are not healing in a comprehensive way. This is at a time when we are prescribing more than ever before, so what is missing?”
According to Dr. Watler, the potential to experience a different level of consciousness is a “gift” that psilocybin offers and can lead to lasting changes in patients facing end-of-life distress.
“There is the knowledge of who you are, which we can have at an intellectual level using various talk therapies, but then having the breakthrough of that experience of a different level of consciousness and seeing ourselves and our place in the universe through an entirely different lens, that, to me, is what medicine should be all about — healing, and not just painting the brown leaves green.”
Story from The GrowthOp
Chronic pain and psychedelics: a review and proposed mechanism of action
May 4, 2020
- PMID: 32371500
- DOI: 10.1136/rapm-2020-101273
Abstract
The development of chronic pain is a complex mechanism that is still not fully understood. Multiple somatic and visceral afferent pain signals, when experienced over time, cause a strengthening of certain neural circuitry through peripheral and central sensitization, resulting in the physical and emotional perceptual chronic pain experience. The mind-altering qualities of psychedelics have been attributed, through serotonin 2A (5-HT2A) receptor agonism, to ‘reset’ areas of functional connectivity (FC) in the brain that play prominent roles in many central neuropathic states. Psychedelic substances have a generally favorable safety profile, especially when compared with opioid analgesics. Clinical evidence to date for their use for chronic pain is limited; however, several studies and reports over the past 50 years have shown potential analgesic benefit in cancer pain, phantom limb pain and cluster headache. While the mechanisms by which the classic psychedelics may provide analgesia are not clear, several possibilities exist given the similarity between 5-HT2A activation pathways of psychedelics and the nociceptive modulation pathways in humans. Additionally, the alterations in FC seen with psychedelic use suggest a way that these agents could help reverse the changes in neural connections seen in chronic pain states. Given the current state of the opioid epidemic and limited efficacy of non-opioid analgesics, it is time to consider further research on psychedelics as analgesics in order to improve the lives of patients with chronic pain conditions.
Keywords: alternative therapies; chronic pain: central pain syndromes, fibromyalgia; chronic pain: neuropathic pain; pain medicine; pharmacology: other.
© American Society of Regional Anesthesia & Pain Medicine 2020. No commercial re-use. See rights and permissions. Published by BMJ.
Canada Will Let Terminally Ill Patients Use Psychedelic Mushrooms For End-Of-Life Care
By Ben Adlin –
Four cancer patients in end-of-life care will be become the first people in decades to legally possess and consume psilocybin mushrooms in Canada after a landmark decision Tuesday by the country’s Ministry of Health.
The patients petitioned Health Minister Patty Hajdu back in April for exemptions from the country’s laws against psilocybin in order to use psychedelic mushrooms as part of psychotherapy treatment. On Tuesday afternoon, Hajdu officially granted the patients’ request, according to the nonprofit TheraPsil, which assisted with the application.
The approvals mark the first publicly-known individuals to receive a legal exemption from the Canadian Drugs and Substances Act to access psychedelic therapy, Therapsil said, and the first medical patients to legally use psilocybin since the compound became illegal in Canada in 1974.
“This is the positive result that is possible when good people show genuine compassion. I’m so grateful that I can move forward with the next step of healing,” one of the patients, Thomas Hartle, said in a statement Tuesday.
Hartle and other patients personally thanked the health minister for what they described as an act of compassion. The applicants, as well as various advocates for psychedelic therapy, had personally appealed to Hajdu via a concerted social media campaign during the months their applications were pending.
In statements issued Tuesday, the patients thanked Hajdu and said they were optimistic that more patients will one day have safe, legal access to psilocybin for therapeutic use.
“I want to thank the Health Minister and Health Canada for approving my request for psilocybin use. The acknowledgement of the pain and anxiety that I have been suffering with means a lot to me, and I am feeling quite emotional today as a result,” said Laurie Brooks, an applicant from British Columbia. “I hope this is just the beginning and that soon all Canadians will be able to access psilocybin, for therapeutic use, to help with the pain they are experiencing, without having to petition the government for months to gain permission.”
TheraPsil said on Tuesday that it expects more patients to petition the government for exemptions following the first four patients’ approval. A separate request by the nonprofit to allow therapists to use psychedelics, was not addressed in Tuesday’s announcement, the group said.
All of the four patients have been diagnosed with untreatable cancer. Therapists who use psychedelics in their practices say that psilocybin-aided therapy sessions can help patients deal with issues such as depression and anxiety, allowing them to better accept death as a natural part of existence.
Health Canada did not immediately respond to Marijuana Moment’s request to confirm the TheraPsil announcement about the approved applications.
“At this point psilocybin is a reasonable medical choice for these individuals,” the group’s executive director, Spencer Hawkswell, told Marijuana Moment in an interview last month. “This is about the minister being compassionate and using her ministerial abilities to help give patients access to something that’s going to help them.”
The therapeutic potential of psychedelics has attracted attention in recent years from a growing number of academics, policy makers and even the U.S. government. In September of last year, Johns Hopkins University announced the launch of the nation’s first-ever psychedelic research center, a $17-million project to study whether psychedelics can treat conditions such as opioid use disorder, Alzheimer’s disease, depression, anxiety and post-traumatic stress disorder.
In June, the University of North Carolina (UNC) announced a $27 million project funded by the U.S. Department of Defense to research and develop an entirely new class of psychedelics-inspired drugs. The program, UNC said, “aims to create new medications to effectively and rapidly treat depression, anxiety, and substance abuse without major side effects.”
Meanwhile, activists in the United States have advocated for state- and local-level reforms to research, decriminalize and in some cases even legalize psychedelics.
In May 2019, Denver became the first U.S. city to enact such a reform, with voters approving a measure that effectively decriminalized psilocybin possession. Soon after, officials in Oakland, California, decriminalized possession of all plant- and fungi-based psychedelics. In January of this year, the City Council in Santa Cruz, California, voted to make the enforcement of laws against psychedelics among the city’s lowest enforcement priorities.
Reformers are pushing for similar changes in other jurisdictions. A proposal in Washington, D.C. would allow voters to decide this fall whether to decriminalize plant- and fungi-based psychedelic drugs, including psilocybin, ayahuasca and ibogaine. A decision on whether that initiative will make the ballot is expected later this week. In Oregon, voters in November will consider a measure that would decriminalize all drugs and expand access to treatment. A separate Oregon proposal would legalize psilocybin therapy—the same therapy sought by the Canadian cancer patients.
Lawmakers in Hawaii earlier this year approved a plan to study psilocybin mushrooms’ medical applications with the goal of eventually legalizing access.
Story from – Marijuana Moment
Pioneering Psychedelic Researcher Once Again Paves the Way with Historic Psilocybin Study for End of Life Patients
BY ANN HARRISON – AUGUST 3, 2020
Amild mannered, bespectacled professor, Dr. Charles S. Grob has been quietly pushing the envelope of psychedelic psychiatry and scholarship for decades.
A Lundquist Institute investigator and Professor of Psychiatry and Bio-Behavioral Sciences at the UCLA School of Medicine, Grob is also the Director of the Division of Child and Adolescent Psychiatry at Harbor-UCLA Medical Center.
Risking his own reputation in the medical community to conduct research that was at one time considered taboo, Grob carried forward the promising studies of the 1960’s and 1970’s which suggested that psychedelic substances had the potential to reduce the pain and anxiety of people approaching death.
Working in a modest office on the grounds of a county hospital in Los Angeles where he runs a mental health clinic for children and adolescents, Grob stepped up to continue meticulous clinical investigations to study the safety and feasibility of psychedelic medications.
Grob and his colleagues at the Harbor-UCLA Medical Center conducted pioneering research into the use of psilocybin as a mental health treatment for terminally ill cancer patients. Published in 2011 in the Archives of General Psychiatry, their Pilot Study of Psilocybin Treatment for Anxiety in Patients With Advanced-Stage Cancer was the first to show that psilocybin had a dramatic effect on the existential distress of people nearing death, improving their quality of life and offering psychospiritual epiphanies.
This early pilot study pointed the way for two following groundbreaking clinical trials published in 2016 that showed the promise of psychedelics to relieve emotional suffering at the end of life.
One set of clinical trials was led by Anthony P. Bossis, PhD, Clinical Assistant Professor of Psychiatry at New York University School of Medicine, and his fellow researchers at New York University. The second was carried out by Dr. Roland Griffiths and a team of researchers at Johns Hopkins University. Both investigations showed that psilocybin reduced anxiety and depression for patients with terminal cancer.
Grob is now practicing telemedicine due to the Covid-19 pandemic, but he and his fellow investigators continue the quest for a deeper understanding of how psychedelics can support people at the end of life.
The Lundquist Institute for Biomedical Innovation announced last month that Grob and Bossis will lead a new multi-site clinical trial to study the effectiveness and safety of psilocybin to treat terminally ill people with psychological distress.
The new clinical trial will be funded by an anonymous $1.75 million donation to The Lundquist Institute. The funds will also be used to develop education and outreach programs on the use of psilocybin for palliative care, a medical specialty that focuses on relieving suffering and improving the quality of life for people with a serious illness.
The Lundquist Institute study will be the first to investigate a psychedelic substance for palliative care and the first to conduct new clinical trials to move the findings of the 2016 trials forward. This research comes at a critical time as a wave of emerging companies and organizations are investigating the use of psychedelics for mental health treatments.
“We don’t die well in America and have few approaches to relieve end-of-life emotional suffering,” says Bossis in a statement from The Lundquist Institute. “Clinical research has demonstrated that psychedelic-generated mystical experience dramatically reduces depression, anxiety, and demoralization in end-of-life existential distress and can improve quality of life and a sense of personal meaning.”
Founded in 1952, the Torrance-CA-based nonprofit Lundquist Institute, supports more than 120 principal investigators working on over 1,000 research studies. The Lundquist Institute created the training for and coined the term “paramedics,” developed human growth hormone, and was involved in the early development of the profession of Nurse Practitioner. It is academically affiliated with the David Geffen School of Medicine at UCLA and works in partnership with the Harbor-UCLA Medical Center.
The editor of two influential books on psychedelics, Hallucinogens: A Reader and Higher Wisdom: Eminent Elders Explore the Continuing Impact of Psychedelics, Grob and co-editor Jim Grigsby will release in February 2021 the Handbook of Medical Hallucinogens, the first formal academic textbook on the topic of hallucinogens and psychedelics.
Grob spoke with Lucid News to reflect on The Lundquist Institute study and the history of research into the use of psychedelic substances for treating the mental health needs of people with terminal illness.
A $1.75 anonymous donation is significant. Who donated the funds for this study?
Dr. Charles S. Grob: I am sworn to secrecy. My lips are sealed. I haven’t even told my wife or daughter.
What makes The Lundquist Institute research unique in the study of psychedelic substances?
What makes this study different from preceding studies is that it has broadened the patient population, it will take place in palliative care settings, and it will train practitioners. There has been a strong level of interest in investigating the palliative treatment model at national and international palliative care conferences. We will be training different palliative care practitioners including doctors, nurses, chaplins, social workers and psychologists.
What also makes this research different is that in the pioneering investigations with psychedelics in the 1960’s and in the modern era, we looked at individuals with advanced cancer. In this study, we are opening it up to people with many additional medical illnesses that might be fatal and who are already enrolled in palliative programs.
When will the study start and how will it be structured?
I think it will start early next spring. We need to still finalize our protocols and submit them to regulatory agencies and go through an Institutional Review Board (IRB) presentation next spring or next summer. It will be a double-bind placebo controlled study and we have budgeted for 60 subjects, but we have been advised to estimate about 80 subjects.
We are not advocating that people use psychedelics in the dying process. The study subjects must have an estimated life expectancy of six months and a palliative care diagnosis for an illness that could lead to a potentially fatal outcome. The study will take place at four to five different sites around the U.S. using the same methodology, the same entry criteria, and the same outcome measures. I would imagine five to six researchers at each site. I can’t confirm the sites at this time.
Another potential complication is this strange world we live in with Covid. How are we going to administer psychedelic treatment in the age of Covid-19? This is going to be challenging because we will be in relatively close proximity to study subjects for many hours. We could be in a small space. Society needs to be in a much healthier place to do this kind of study and go through all the hurdles. I’m sure we will work this out and other groups working with psychedelics will work this out.
Why is this study needed now?
The study of psychedelic substances has gone from a small field to expanding rapidly into something that at times feels over the top. I am concerned that proper attention to establishing safety parameters – and the importance of that in this context – may not be a priority for some investigators. It’s good to see enthusiasm for this research, but people implementing these studies need to prioritize the need for safety and established ethical standards. I have written a paper with other researchers on the need for strong ethical standards and safety parameters which we will publish this year.
Is this study historically significant?
Yes. This is the first study of this sort since the 1960s or early 1970s. In the 1960’s, this was one of the most promising areas for psychedelic-assisted treatment. In the early 1960’s, Dr. Eric Kast, a pain specialist at the Chicago Medical School, conducted research administering LSD to hospital patients in chronic pain and recorded positive effects in pain reduction, improved mood, outlook and quality of life with less fear of death. This research was followed up by Walter Pahnke, Stanislav Grof, and Bill Richards who did work in the late 1960’s and early 1970s finding dramatic effects with the improvement of anxiety and the reduction of pain.
They found that the strongest predictor of positive therapeutic outcome was, during the course of the session, the patient having a powerful psychospiritual epiphany. Humphry Osmond, in the late 1950’s, also found that this predicted the best outcomes while studying the use of psychedelics to treat people with alcohol dependency.
Why did this research stop moving forward after the initial studies in the 1960’s and 1970’s?
The psychedelic research in the 60s and 70s was not halted due lack of positive outcomes or the safety of the research. It was stopped for cultural and political reasons. It got conflated with the culture wars of the 60’s and was identified with a politically active counterculture. In the 60’s, the divisiveness became a cultural divide and psychedelics became a sacrament for the counterculture. You were on one side or the other side.
Some leaders like Timothy Leary, who was a brilliant researcher, also had a penchant for being very provocative and the compounds were eventually considered too hot to handle. There was no approved research in the U.S. from the early 1970s to the early 1990s, when our team conducted the first clinical study with MDMA. Our Phase 1 study of MDMA was also around the same time as Rick Strassman’s investigation of DMT and Deborah Mash’s study of ibogaine. These three studies were the first approved investigations of psychedelics since the late 1960s and early 1970s.
What has changed culturally that has allowed this research to continue now?
The Archives of General Psychiatry, which published our pilot study in 2011, accepts a miniscule number of papers. Why did they accept ours? They recognized that psychiatry needs new and novel and more effective treatment models and after decades of quiescence, the world we live in has changed and investigating psychedelics has once again become accepted and respected. Our values have changed and we have a more mature manner in which this research is recognized. In the 60’s it was brand new and it took the culture by surprise.
By the late 1990s and the early 2000’s, we had weathered the tempest and were in a more open and receptive phase. There was recognition that conventional treatments in psychiatry are sometimes helpful, but sometimes lacking in efficacy. As healers and scientists, it is important to objectively examine new and novel treatments for people who do not get substantial relief from conventional treatments.
What researchers most influenced your work with psychedelic substances?
We were the first to work with an advanced cancer population and we basically took Stanislav Grof’s work and investigations from that era and adapted it, modernizing the protocol and changing some of the criteria. But the inspiration came from the pioneering research of Grof and Walter Pahnke, Gary Fisher, Bill Richards and others.
Those who came before these investigators were the true experts and authorities on psychedelic plants. The indigenous people throughout the world knew the plant life in their geographic areas and used these plants for healing and divination and spiritual purposes. I would like to credit not only the prior generation of investigators, but the indigenous people who have been historically mistreated. They kept the tradition of plant hallucinogens alive and concealed them from the Spanish and Portugese invaders.
What has most influenced your thinking about the dying process?
My views began forming early. Before I pursued my training in psychiatry and internal medicine, I grew up in a household where my father was a prominent internist. I grew up in that medical world and observed with patients and family members that the dying process is often associated with very severe psychological pain, isolation, alienation and existential distress.
I encountered Grof’s work in the early 1970s and his case reports of working with individuals not just undergoing physical suffering, but also psychological and psychospiritual pain and anguish. I would look at patients on medical floors and say, “there has got to be a better way.”
Aldous Huxley also had a beautiful image in his novel Island of how these compounds might help the passage from life to death. Grof’s work was very encouraging. I took his message to heart as I got my credentials and training and waited for a time to again do feasible human research with compounds that had been taboo for a long time.
What role do you see psychedelics playing in the future of palliative care?
We can see how they could endow palliatieve practitioners with additional tools. We developed our study with Dr. Ira Byock, a former director of palliative medicine at Dartmouth-Hitchcock Medical Center. He is a palliative care practitioner who really made a significant contribution to the evolution of Tony’s [Bossis] and my thinking on that issue. He helped us to embark on this study.
What else should we know about this study?
I’ve worked for 27 years with The Lundquist Institute and the Harbor-UCLA Medical Center. They have always been very collegial and supported research ideas that in some quarters were considered taboo. I explained our rationale and safety parameters and they heard me out. They knew I could be trusted to conduct the early MDMA and psilocybin research and take the data back to UCLA and Lundquist.
Although we have received a very generous grant for this study, it’s only half of what we think we will need in the bank to get this research off the ground. If a research program already has funding, it is easier for other funders to make generous donations. That is what we hope will happen here.
Terminally ill Canadians apply for legal access to ‘magic mushrooms’ drug
Monday, June 8, 2020
TORONTO — For Thomas Hartle, every day is a challenge because of his anxiety.
The 52-year-old from Saskatoon has terminal cancer and the thought of the future triggers his anxiety on a daily basis.
“It gives you a rapid heart rate. It makes you feel terrible,” he shared with CTV News’ medical correspondent Avis Favaro.
That is why he’s one of a handful of terminally ill Canadians who are appealing to the federal health minister for a special exemption on compassionate grounds that would allow them to use an illegal drug found in “magic mushrooms.”
The drug is called psilocybin and is a naturally occurring psychedelic compound produced by several species of mushrooms.
Growing research on the psychedelic appears to show that it has the potential to provide long-term relief for anxiety and depression, particularly among terminally ill patients suffering from “end of life” distress.
Scientists around the world have found the drug shows promise in being able to rewire the brain and boost mood in patients, with one study showing that up to 80 per cent of palliative patients reported reductions in depression and anxiety, and improved attitudes towards death.
In one U.S. study published in the Journal of Psychopharmacology in January, patients with cancer-related psychiatric distress continued to experience reductions in anxiety, depression, hopelessness, demoralization, and death anxiety more than four years after a single dose of psilocybin in combination with psychotherapy.
Researchers at the U.S. Center for Psychedelic and Consciousness at Johns Hopkins University in Baltimore are currently conducting Phase 3 clinical trials with the aim of having psilocybin approved for market as a prescription medication.
Roland Griffiths, the centre’s director, told CTV News earlier this year they initially faced a lot of skepticism about the safety of the drug. Since then, they have published multiple studies on the benefits of using one dose of psilocybin in a treatment that runs approximately six hours and has few side effects.
“Psilocybin produces conditions under which people report having a sense of increased efficacy, a change of world view, a sense of change of self, and that they’re able to re-engage in the world in very positive ways,” Griffiths said during an interview with CTV News in February.
That inner change is one of the reasons why Hartle is appealing to Health Minister Patty Hajdu to grant him legal access to psilocybin for compassionate reasons.
“Most people come out of this experience with a more spiritual connection to whatever it is they believe in. For me, that is an appealing thing,” he said. “What I am looking for is something that helps me deal with problems and anxieties that I just don’t have another mechanism of dealing with.”
LEGAL ACCESS
In order to legally possess and use psilocybin, Hartle has to apply for a Section 56 exemption of the Controlled Drugs and Substances Act and be approved by Hajdu.
Hartle isn’t the only one opting for this route, either.
In January 2017, Bruce Tobin, a psychotherapist and professor at the University of Victoria, applied to the minister of health for a special exemption that would enable him to legally possess and use psilocybin to treat patients experiencing end-of-life distress.
After three years, he said his application was rejected in early March on “the basis that there is insufficient evidence to demonstrate the medical need for psilocybin.”
Now, Tobin has pivoted his focus to helping individual patients apply directly to Hajdu for special exemptions with the assistance of his group TheraPsil.
TheraPsil is a non-profit coalition of health-care professionals, patients, and advocates who are working to gain legal access to psilocybin on compassionate grounds as well as provide public education, training for health professionals, and expanding research on the drug.
“If Canadians have the right to die acknowledged, surely they must have the right to try. The right to try a novel medicine. The right to try to have a better life before they finally do pass away.”
While there is enthusiasm for the use of psilocybin as a treatment for anxiety and depression, there are some scientists who say there isn’t enough proof yet to demonstrate the drug’s efficacy and safety for widespread use.
Dr. Martin Chasen, a palliative care physician and the medical director for palliative care at William Osler Health System in Ontario, noted that in studies on psilocybin, psychotherapy sessions are mandatory as part of the treatment, patients are carefully selected, and the drug is administered in a controlled environment.
“A multisite study in a larger and more diverse patient population should be conducted to establish the generality and safety of psilocybin treatment of psychological distress associated with life-threatening cancer,” he said.
Although there may be doubts about psilocybin’s use in medicine, Toronto lawyer Paul Lewin said medical cannabis was also once off-limits before the pressure grew from those who felt they had no other option.
“There’s a lot of peer-reviewed, rock solid research supporting it,” he told CTV News. “Hopefully, it is not necessary to have endless litigation as it was with cannabis.”
That’s what Hartle hopes as well, as he pushes to have his case pave the way for others behind him.
“Not everybody has terminal cancer, but there are a lot of people who also suffer from anxiety and depression out there,” he said. “If my going through the discomfort of having to apply for this and ask for permission to use this will benefit somebody else whose anxiety is stopping them from doing this… then that’s a purpose.
Everyone wants to have something that they can leave behind.”
Story From CTV
Psychedelic Drugs Can Improve Quality Of Life – And Death – For Older Adults
Abbie Rosner – Contributor
Vices – I cover how older adults are discovering and re-discovering cannabis.
Even before COVID-19 set off a global tsunami of anxiety and depression, psychedelic drugs were already showing exciting promise for treating these and other intractable mental health conditions.
Compass Pathway’s recent raise of $80M to expand research into the clinical uses of psilocybin only affirms that no coronavirus is going to dampen efforts to make these treatments legal and widely accessible. If anything, the need for an effective answer to COVID-era angst makes this work even more urgent.
Especially for Baby Boomers and their elders, developments in the psychedelic space are worthwhile following, particularly because of their potential to radically improve quality of life, up to its inevitable end.
Older Americans suffer disproportionately from chronic pain and its attendant ailments, anxiety, depression and insomnia. In the search for relief, they consume more pharmaceutical drugs than perhaps any comparable cohort on this planet.
Psychedelic therapies to treat mental health conditions offer a radical departure from current pharmaceutical models that wed individuals in a lifelong bond of drug-taking. Instead, the psychedelic therapy modalities currently under investigation combine a limited number of treatment sessions with a psychedelic substance, sandwiched between intensive pre- and post-treatment therapy sessions. The ideal, and realistic, outcome from this course of treatment is not mere symptom control but durable remission.
Story from Forbes
High Stakes: Will The Legalization Of Psychedelics Mimic That Of Cannabis? Will It Learn From Its Mistakes?
DoubleBlind Mag – March 10, 2020
By Double Blind‘s Madison Margolin, provided exclusively to Benzinga Cannabis.
The cannabis industry has drifted from its grassroots values. Will the psychedelic field learn from its mistakes?
I’m in the back corner of a Hollywood cafe and I just took a hit off my vape pen. For focus, mainly, and to get some creativity flowing. No one seemed to notice or care, plus the vapor smells more like rose than like weed. The pen itself is pink, now sitting in the front pocket of my purse with my earbuds, chapstick, car keys, and a small jar of cannabis salve for my tendinitis.
At home, I have a ziplock baggie of psilocybin mushrooms hidden in my bedroom. They’re tucked away with a square of tin foil wrapped around some MDMA powder. The baggie, the foil, the hiding spot—it’s the definition of a “drug stash.” The last time I treated cannabis this way was my freshman year of college nearly a decade ago.
Things have changed since then, at least here in California. My designer weed feels like an accessory to my makeup bag, and I can’t remember the last time someone gave me bud in a ziplock. I know it’s only a matter of time before psychedelics go the same way. But do we want them to?
Granted, microdosing psychedelics is on its way to becoming almost as socially acceptable as vaping cannabis before work. As of a 2013 National Survey on Drug Use and Health, nearly 7% of the American population had taken MDMA, while on any given weekend, dozens of ayahuasca ceremonies are happening in lofts, yoga studios, and private homes all over Brooklyn, Los Angeles, the Bay Area, and beyond.
Psychedelics are fast re-entering the mainstream, with prudent visionaries, scientists, and academics like Rick Doblin, founder of the Multidisciplinary Association of Psychedelic Studies, Michael Pollan, author of How to Change Your Mind, and Johns Hopkins’ researcher Roland Griffiths, among others, leading the way.
Some argue that the psychedelic movement is where the cannabis movement was only a decade ago—and they have a point. California pioneered medical marijuana in 1996 and, since then, 33 states have legalized cannabis for medical or adult use, the FDA has approved the first cannabis-based medicine for prescription, and cannabis has become a central issue for some candidates on the campaign trail. In many ways, the cannabis plant’s route to legalization serves as both a template for psychedelics, as well as an example of what not to do along the way.
In many ways, the cannabis plant’s route to legalization serves as both a template for psychedelics, as well as an example of what not to do along the way.
See Also: What You Need To Know About Publicly-Traded Psychedelics Companies
Though disproven as a gateway drug, cannabis indeed is a gateway plant, introducing consumers to a plant-based approach to wellness. Having experienced the power of cannabis therapy, those who may otherwise have feared psychedelic “drugs” are seeing their merit.
The approach to cannabis legalization has been threefold. The most obvious route has been local, with state measures to decriminalize or legalize cannabis for medical or recreational purposes. Key players in state markets like California’s, luring the brightest minds in marketing, have rebranded cannabis as a wellness and lifestyle product. Once embraced only by hippies, cannabis has been sterilized enough to lure even the most conservative squares (like John Boehner) into the industry. Congress is catching on, too, now considering a record number of bills to deschedule or otherwise promote cannabis law reform. The federal approach comprises the second route to reform.
Meanwhile, the third prong is through FDA rescheduling. Currently, Sue Sisley, president and principal investigator at the Scottsdale Research Institute, has partnered with MAPS to study cannabis flower as a treatment for veterans with PTSD. When the research is complete, the idea is for cannabis, in its organic form, to become an affordable, prescription medication.
“One of the things that the cannabis movement has done right is having operated in multiple levels of government,” says Noah Potter, author of The Psychedelic Law Blog and an attorney with cannabis firm Hoban Law Group. “There’s no central organizing on cannabis, but it has happened organically as people have stepped up in different capacities as journalists, as physicians, and as entrepreneurs, [while] for better and for worse, there’s a diversity of messaging on cannabis.”
Similar to organizations like the National Organization for the Reform of Marijuana Laws or the Drug Policy Alliance, MAPS, a nonprofit which has sponsored much of the recent, pioneering psychedelic research, has strong political leanings.
Yet MAPS and other research nonprofits are not alone in seeking to make psychedelics legal, as medications. There’s been concern among some key players in the psychedelic community that COMPASS Pathways—a for-profit company whose research has recently been put on the fast-track by the FDA to develop psilocybin therapy for depression—is an indication that people looking to profit from psychedelics, rather than ensure their accessibility, are getting into the space. The company is backed by major venture capitalists including Peter Thiel and Michael Novogratz.
We’re now seeing at least a two-pronged approach to psychedelics, mirroring cannabis. The first is government-approved research on MDMA for PTSD and psilocybin for anxiety, addiction, and other conditions. The second is state- and city-level initiatives in places like Denver and Oregon to decriminalize or legalize psilocybin. According to Oakland’s Decriminalize Nature campaign, more than 55 cities now want to replicate the city’s initiative, which passed in June, to decriminalize all naturally-occurring psychedelics.
But as Potter mentioned, the “diversity of messaging” has its drawbacks, too: Without a central tenant to either the cannabis or psychedelic movement, there’s no way to ensure these industries grow to be accessible or equitable.
How is it that in the cannabis industry, for instance, thousands of Drug War victims (mainly people of color) remain incarcerated for minor cannabis violations, while white men (those like Boehner) make headway in yet another increasingly corporate American industry?
“You combine cannabis with capitalism, in which cannabis is now just a consumer product, and it’s now just all about the money,” Potter says.
Consequently, we’re now in a place where even black market farmers and gray market dispensary owners, who for decades lived under the looming threat of having their livelihoods taken from them, are bemoaning legalization amid burdensome regulations and an inability to compete with Big Marijuana. And whereas women once comprised 36% of executives in the cannabis industry, the mainstreaming of pot has had the side effect of reducing that statistic by about 9%, according to a 2017 survey by Marijuana Business Daily. With a number of industry execs having never even gotten high themselves, it’s hard not to wonder how the cannabis industry digressed so far from the morals of its original, grassroots movement.
And that’s just the question we should be asking about the coming psychedelic industry: How can the commercial market uphold the values of community and compassion so often reinforced when a person is under the influence of these entheogenic plants?
While, admittedly, there are far fewer prisoners of the War on Psychedelics than the War on Weed, equity in the case of psychedelics means not only including marginalized groups in the nascent industry, but ensuring psychedelic medicine as a right, rather than a privilege. Also, says Potter, to go about psychedelic legalization solely for the purpose of providing medicine feeds into the prohibitionist paradigm that these substances may still be unsafe outside that paradigm; it neglects their merit in recreational or spiritual purposes, the line between both often being hazy.
See Also: Will Shroom Dispensaries Become A Thing Anytime Soon?
There remains a need, within the movement, to uphold the right to cognitive liberty, the pursuit of happiness, and the innate yearning for spiritual connection—all alongside the need for better medicine. At the same time, we need to ensure that the movement and industry give due respect to the indigenous cultures that have been using these substances, safely and wisely, for generations. “You now have potential exploitation of these substances for-profit and first-world psychedelic tourism,” says Potter.
Ultimately, psychedelic legalization would be preferable to decriminalization, Potter argues, because it would allow psychedelics to be regulated and make a larger dent in the Drug War. But, in order for psychedelics to actually become integrated into society, the medical-spiritual-commercial divide will have to shift, too. If done properly, says Potter, “that will have profound implications for everything we do.”
Story in Benzinga Magazine
The growing push for medical use of psilocybin in Canada
CTV News – February 15, 2020
TORONTO — Growing evidence about the powers of psilocybin, a naturally occurring psychedelic compound produced by several species of mushrooms, being used to treat anxiety and depression has inspired advocates to file a federal court challenge next month to allow its use to treat terminally ill patients.
Psychotherapist and professor at the University of Victoria Bruce Tobin has been on the forefront of those advocating to end the prohibition of the drug – highlighting its potential for cancer patients who often suffer from what is described by doctors as “end of life distress.”
End of life distress is a “nasty combination of anxiety, depression hopelessness and demoralization that often accompanies the diagnosis of a terminal illness such as cancer,” Tobin said in an interview with CTV News’ medical correspondent Avis Favaro. “My desire is to get the treatment to patients who are in need of it right now.”
Psilocybin found in what is colloquially known as “magic mushrooms” is illegal in Canada, but Tobin said he has witnessed patients undergoing psychotherapy feel calmer and less stressed by using the compound.
“We can see the results in many cases very quickly, as quickly as the next day,” he said.
Tobin says he has been waiting three years for Health Canada to respond to multiple applications for psilocybin’s compassionate use in terminally ill patients.
“My attitude now is treatment delayed is treatment denied,” Tobin said, explaining that he will continue to push for psilocybin to be exempted from the Controlled Drugs and Substances Act.
Three thousand patients per year in Canada are suffering from “end of life distress” and fit the criteria for so-called psilocybin-assisted psychotherapy, Tobin said.
His campaign is supported by a group he formed, entitled “TheraPsil: Therapeutic Psilocybin for Canadians,” which lists the scientific, legal and moral reasons the group believes the compound should be made legal for “end of life distress” cases.
Research into the medicinal uses of psilocybin has been growing exponentially.
A U.S. study published in the Journal of Psychopharmacology in January showed that cancer patients who were given the compound reported reductions in anxiety, depression, hopelessness, demoralization and death-related anxiety more than four years after receiving their doses in combination with psychotherapy.
A second study from the U.K. in the Journal of Psychopharmacology suggested that when given to patients with treatment-resistant depression, psilocybin affected “functional connectivity” changes in the brain which was evident in scans. The study suggested that “psilocybin therapy improves how the brain works and revives emotional responsiveness.”
The field of psychedelic research is “very exciting” according to professor Roland Griffiths, director of the Center for Psychedelic and Consciousness at Johns Hopkins University in Baltimore.
Griffiths’ centre was the first to obtain regulatory approval in the U.S. to restart research into psychedelics using healthy volunteers. Previous research into psychedelics met an abrupt end during the war on drugs in the 1970s.
“When we initiated this research there was a fair bit of skepticism on the part of many, my colleagues and certainly regulators, about whether or not this work is safe,” Griffiths said in an interview with CTV News.
Now his research group is publishing an array of studies on the benefits of using one dose of psilocybin in a treatment that runs approximately six hours and has few side effects and displays benefits to patients’ perceptions.
“Psilocybin produces conditions under which people report having a sense of increased efficacy, a change of world view, a sense of change of self, and that they’re able to reengage in the world in very positive ways,” Griffiths said.
Griffiths said that as patients reflect back on those experiences with psilocybin, they “often have this sense of a profound coming to an understanding of a deeper level of who they are.”
With many psychiatric disorders proving difficult to treat, Griffiths said the team at Johns Hopkins is expanding its testing of psilocybin and other psychedelics, such as LSD, for conditions including obsessive compulsive disorder, post-traumatic stress disorder, opioid use disorder, alcoholism and anorexia nervosa.
Other research is examining the benefits of microdosing, which uses small doses of psilocybin to treat anxiety and depression. A survey of people self-managing mental and substance use disorders by microdosing found 44 per cent of them perceived their mental health was “much better” as a result.
Some Canadians are not waiting for the studies.
Michael Ljubsa of Edmonton, Alta., struggled with depression when he left high school and began university, and said he was unable to find relief with the standard therapies or medications available to him.
“I just became like a zombie basically,” he said in an interview with CTV News. “It became just difficult to function.”
Ljubsa experimented with psilocybin in Jamaica, where it is legal, to try and help – not something doctors recommend – and described a change in self-perception he found “liberating” and boosted his mental wellbeing. He is now an advocate of further psilocybin research.
“Any sort of work that is being done to bring this medicine to people as fast as possible is the work that needs to be done,” Ljubsa said.
At least two centres in Canada are pursuing studies of psilocybin. The University of Toronto Mississauga has launched a Centre for Psychedelic Studies and will host the world’s first clinical trials on microdosing psilocybin. Other related research is planned at the University of British Columbia’s School of Population and Public Health.
“I think we are entering a new era in the treatment of mental health conditions,” Griffiths said.
“Psilocybin and these compounds have mechanisms unlike anything we have seen within our normal treatment options within psychiatry,” he continued. “The potential…to have efficacy across a range of conditions is absolutely remarkable. We just don’t understand the mechanisms of them yet.”
Story from CTV News
Cybin Partners With Toronto Centre For Psychedelic Science For Psilocybin Research Project
by Natan Ponieman – February 13, 2020
Cybin Corp., a Canadian life sciences company focused on psychedelics and mushroom-psilocybin research, announced a new partnership with the Toronto Centre for Psychedelic Science.
With this partnership, the centers’ co-founders, Rotem Petranker and Thomas Anderson will be appointed exclusive clinical advisors to Cybin.
“We feel many of the positive results that people have experienced with psychedelics require further scientific study with transparently-disclosed protocols and proper research study architecture to achieve repeatable results,” Paul Glavine, CEO of Cybin Corp. told Benzinga. “Rotem and Thomas’ commitment to open science echoes our philosophy. Together we expect to build a solid foundation and future for this industry, grounded in research and the scientific method.”
… from Benzinga
Psychedelics associated with reduction in problematic drug use: study
More research is needed to evaluate the connection between psychedelics and addiction.
By Emma Spears – February 4, 2020
A new study suggests psychedelics may have a place in the treatment of addiction.
The consumption of psychedelic drugs such as psilocybin is correlated with “persisting reductions” in the use of cannabis, opioids and stimulants, noted new research published this week in the journal Frontiers in Psychiatry.
Researchers from the John Hopkins School of Psychiatry and Behavioral Sciences and the Department of Neuroscience, The Ohio State College of Social Work and the Erowid Center contributed to the study.
“Observational data and preliminary studies suggest serotonin 2A agonist psychedelics may hold potential in treating a variety of substance use disorders (SUDs), including opioid use disorder (OUD),” researchers wrote.
The study recruited 444 adults via advertisements online who claimed to have overcome addictions to alcohol and/or drugs through the use of psychedelics. Each participant completed an anonymous survey that assessed a variety of factors, including problematic substance use.
Researchers discovered that the majority of subjects in the study self-reported using psilocybin (a compound in so-called “magic mushrooms”) or LSD to provoke a psychedelic experience.
On average, participants reported about 4.5 years of problematic substance use. Approximately 79 per cent of study participants met the retrospective criteria listed in the DSM-V (Diagnostic and Statistical Manual of Mental Disorders) for severe substance abuse disorder prior to consuming psychedelics, and 96 per cent met the criteria for substance use disorder.
After their “psychedelic experience,” researchers say that only 27 per cent met the criteria for substance abuse disorder.
Participants who consumed higher doses of psychedelic substances, and reported more “mysticism,” epiphanies or insight as a result of the consumption, had a tendency to report a more substantial reduction in the consumption of other drugs.
The study’s authors emphasize that more research is needed to evaluate the connection between psychedelics and addiction, but that the results offer a promising direction for further study.
“While these cross-sectional and self-report methods cannot determine whether psychedelics caused changes in drug use, results suggest the potential that psychedelics cause reductions in problematic substance use, and support additional clinical research on psychedelic-assisted treatment for SUD,” the authors noted.
Story from The Growth Op
‘Clinically reassuring’: Massive trial finds psilocybin safe for human consumption
Denver became the first city to decriminalize the drug earlier this year and a handful of cities have begun to follow suit.
Move over cannabis. Magic mushrooms are on the way.
Researchers at Kings College London in the U.K. have concluded the world’s largest controlled study of psilocybin and determined it to be safe for human consumption.
“The results of the study are clinically reassuring and support further development of psilocybin as a treatment for patients with mental health problems that haven’t improved with conventional therapy, such as treatment-resistant depression,” said James Rucker, the study’s lead researcher, according to the Independent.
Phase one of the study was meant to examine if psilocybin — the psychoactive component of mushrooms — is safe for consumption while phase two, currently underway, examines the therapeutic potential of the drug.
As part of phase one, 89 subjects were given 10 mg of psilocybin, 25 mg of psilocybin or a placebo during a six-hour session with a therapist. There were 25 dosing sessions and a follow-up period of six weeks.
While researchers found expected adverse effects related to mood and sensory perception, cognitive and emotional functioning were not negatively impacted.
“This study is part of our overall clinical development programme in treatment-resistant depression,” said Ekaterina Malievskaia, co-founder of Compass Pathways, the company behind the study. Phase two trials are taking place in Europe and North America using 216 patients to test psilocybin’s ability to treat depression.
With the legalization and decriminalization of cannabis making news and opening up new avenues of research around the world, the paradigm has already shifted on psilocybin mushrooms.
Denver became the first city to decriminalize the drug earlier this year and a handful of cities have begun to follow suit. California and Oregon organizers are hoping to get a legalization question prepared in time to make the 2020 ballot for a state vote.
Like cannabis, psilocybin has a long track record of relative safety among recreational users, and it is not toxic.
Unlike some drugs that treat anxiety and other mental conditions, psilocybin is not prone to dependence. But given its hallucinogenic effect, lawmakers may be reticent to allow distribution of the psychedelic drug without more restrictions.
Story from The Growth Op
Is psychedelic medicine the future of therapy?
Vogue speaks to psychiatry experts about the latest research into psilocybin, the active agent in ‘magic’ mushrooms, which is proving to be an incredibly effective mental health treatment.
Ellen Burney – 28 January, 2020
Could the hallucinogenic love drug of the 1960s soon be a regular feature in mainstream medicine? The prospect is not so far out. After decades of antidepressants failing to deliver ‘happiness in a pill’, neuroscientists and psychiatrists are now rooting for a dose of psilocybin – the active agent in ‘magic’ mushrooms – to treat depression, anxiety, addiction and more.
Psilocybin is the latest in a boomlet of party drugs finding new status on the world stage of mental health medicine. Esketamine (derived from ketamine) was licensed for supervised use in treatment-resistant depression by The US Food and Drug Administration (FDA) in March 2019, and the European Commission in December 2019, but with this drug critics warn of a potential for abuse. Studies into psilocybin, however, suggest its therapeutic benefits to be fast working, non-addictive and side effect-free.
The World Health Organization (WHO) estimates that more than 264 million people globally suffer from depression, and about one-third do not respond to antidepressants; while close to one billion people suffer from a mental illness or substance abuse disorder. “There has been a dearth of major breakthroughs in mental healthcare for several decades now,” says Dr Robin Carhart-Harris, head of the Centre for Psychedelic Research at Imperial College, London, which opened in April 2019 – the first of its kind.
“Despite record breaking increases in prescription rates of psychiatric medications, this is not impacting on rates of mental illness – indeed these are going up instead of down – so clearly something is very wrong,” Carhart-Harris continues. “My strong hope is that the development of psychedelic therapy will have a revolutionary impact on mental health care, bringing the ‘care’ component back and transforming societies and systems as a result.”
The psychedelic therapy research
Back in 1962, Dr Timothy Leary started the Harvard Psilocybin Project, but before long there was a backlash against LSD and in 1971, the United Nations made psilocybin mushrooms a Schedule I drug – like heroin. Signalling a seismic shift in gear since that shutdown, the FDA finally granted ‘Breakthrough Therapy’ status to psilocybin in 2018, meaning an accelerated review and development of the drug due to its potential to treat a serious condition.
“To date, the classic psychedelics like psilocybin and LSD have been most extensively studied for mood issues such as depression, existential distress related to serious illness and substance use problems,” explains Dr Albert Garcia-Romeu, an instructor at the Center for Psychedelic and Consciousness Research, which opened in September 2019 at Johns Hopkins University of Medicine in Baltimore.
“In each of these areas we’ve seen very promising early results in small trials that are currently being expanded on in larger studies at Johns Hopkins and around the world,” Garcia-Romeu continues. A research project at the University of San Francisco, California, is testing psilocybin for distress in patients with AIDS, and in addition to psilocybin, Johns Hopkins is also researching MDMA-assisted therapy for post-traumatic stress disorder and anorexia.
What does a day in psychedelic therapy look like?
“This treatment is a new paradigm of psychiatric medication,” says Dr Matthew Johnson, associate director at the US research centre. “The medication prompts an experience and therapeutic process from which the person can learn. In many ways it is more like medication-induced deep psychotherapy.” Or the medical equivalent of hallucinogenic healing under chaperone of an ancient spiritual shaman.
“High-dose psilocybin has pronounced psychoactive and mood-altering effects for most people within one hour of taking the drug, usually subsiding within six to eight hours of administration,” explains Garcia-Romeu. “These effects are largely mediated by activity at the serotonin 2A receptors, and likely other downstream mechanisms that we are just beginning to tease apart.”
In a day-long clinical session, supervised by two therapists, trial patients are given a dose of 20 to 30 milligrams of pure psilocybin. “This corresponds to, on average, about four to five grams of dried psilocybe cubensis mushrooms, the most common type in the illicit market,” Johnson tells Vogue. “They wear eye shades to focus attention inward, and headphones through which mostly classical music is played. They are told to ‘trust, let go, be open’ and not to resist the experience.” There’s no therapy during the session, but patients can discuss the experience afterwards and will have a follow-up psychotherapy session the next day.
“This is not ‘take two and call me in the morning,’” warns Johnson, stating that psilocybin will never be available over the counter. “[Treatment] would resemble our current research trials, which are much like outpatient surgery, but with even more preparation and follow-up care.” The treatment – which he expects to be FDA-approved for depression in a couple of years – will always be delivered alongside psychotherapy. So, around 12 one-hour sessions of talking therapy with two doses of psilocybin.
The psychedelic therapy side effects:
1. The anti-zombie effect
Rather than the notorious ‘zombie’ side effect of selective serotonin reuptake inhibitors (SSRIs, such as Prozac), therapy sessions incorporating psilocybin appear to expand rather than numb emotions. “People typically report feeling more connected as opposed to disconnected from their life,” Johnson notes.
Carhart-Harris agrees. “Most conventional drugs come with a bunch of side effects and if they work, they often do so through muting a person’s emotional range. Psychedelic therapy brings multiple advantages: it can work after just one or two sessions (unlike psychotherapy or standard drugs, which can take weeks or months to work) with minimal toxicity and people can remain well long after the drug has left their bodies, sometimes entirely transforming their sense of well-being and life satisfaction.”
2. The sense-of-self effect
“The on-going research on the efficacy and safety of psychedelic medicine is very promising indeed,” notes Dr Michalis Kyratsous, consultant psychiatrist at South London and Maudsley NHS Foundation Trust.
“Subjects using psilocybin have reported a profound alteration to their ordinary sense of self, known as self-dissolution,” “And this effect can be potentially used to address specific set of symptoms, such as excessive self-focus in depression.”
3. The enlightening effect
There also appears to be an enlightening effect. “It’s a deeply held spiritual experience that seems to connect people to themselves, to others around them, to the universe,” says Dr Alan K Davis, assistant professor at the US research centre, who also guides the psychedelic therapy sessions. “That type of experience also can include things like psychological insight, where someone is gaining new information or awareness about themselves, the world around them, their relationships or past experiences.”
“A reminder this is not a daily medication,” Davis emphasises. “It’s a medication that people take twice with therapy. The fact that we can see these long-term results, compared to medications that they will have to take every day for the rest of their lives, is pretty remarkable.”
Story from Vogue
City of Santa Cruz Decriminalizes ‘Magic Mushrooms’ and Other Psychedelics
January 30, 2020, By CNN Wire
The city of Santa Cruz, California, has become the latest city to decriminalize “magic mushrooms” and other natural psychedelics, including ayahuasca and peyote.
The Santa Cruz City Council voted unanimously to approve a resolution that makes investigating and arresting people 21 and older for using or possessing psychoactive plants and fungi among the lowest priorities for law enforcement.
Tuesday’s resolution doesn’t necessarily make it legal to use or possess natural psychedelics, but it does mean that the city won’t be using resources to investigate or arrest people for doing so. People could still face penalties for the sale or cultivation of those substances.
Santa Cruz is the third city to take such a step. Denver voted to decriminalize psychedelic mushrooms in May of last year, while Oakland decriminalized all psychedelic plants and fungi shortly after.
The resolutions or ordinances passed by Santa Cruz, Oakland and Denver don’t apply to drugs such as LSD or MDMA, which are synthetic.
Other places are considering similar measures
Chicago is among other cities considering a resolution to decriminalize certain psychedelics, and efforts to enact similar measures are underway in some states.
In Oregon, a campaign called PSI 2020 is lobbying for a measure on the ballot that could make the use of psilocybin, the hallucinogenic compound found in psychedelic mushrooms, legal statewide.
If the measure passed, the Oregon Health Authority would oversee a program that would allow psilocybin to be administered in licensed therapeutic environments and supervised by trained professionals. People would not need a mental health diagnosis to receive therapy, according to the language in the measure.
“We think that this novel approach could help alleviate the mental health crisis here in Oregon by addressing epidemics like suicide, treatment-resistant depression and anxiety, PTSD, and addiction to drugs, alcohol, and nicotine,” PSI chief petitioners Tom and Sheri Eckert say on the campaign’s website.
“Additionally, the measure would open doors for new research and create access to services for those interested in personal development.”
A campaign for a similar measure on the ballot in California is also underway, after it failed to get enough signatures last year. That measure would decriminalize personal possession, use and cultivation of psilocybin statewide for people 18 and older.
Last year, Iowa Republican state representative Jeff Shipley introduced two bills in the legislature to decriminalize psilocybin used for medicinal purposes, and remove it from the list of schedule I controlled substances.
Research suggests psychedelics have health benefits
Natural psychedelics have long been popular for recreational use, though many have been banned at the federal level for decades.
The US Department of Justice classifies psilocybin as a Schedule I controlled substance, which means that federal policy states that it has no currently accepted medical use and a high potential for abuse.
But a growing body of medical research suggests that psilocybin can be used to treat conditions such as anxiety and depression, in cases where drugs currently on the market cannot. It has also been found to have a low potential for abuse, and no potential for physical dependence.
A 2017 study published in the journal Nature showed that 47% of patients experiencing treatment-resistant depression showed positive responses at five weeks after receiving a psilocybin treatments.
And in 2018, researchers from Johns Hopkins University called for removing psilocybin from the list of Schedule I substances.
Story from CNN Wire/KTLA
Psychedelics: Can getting high improve your mental health?
By Sandee LaMotte, CNN – January 24, 2020
(CNN) Can the mind-blowing effects of psychedelics help heal our traumas?
“The Goop Lab,” Gwyneth Paltrow’s new Netflix mini-series, tackles the topic in their first episode by sending several Goop employees to Jamaica to ingest magic mushrooms under the careful guidance of psychotherapists.
One young woman, traumatized by her father’s suicide, declares she “went through years of therapy in about five hours.”
What does the scientific community say about the role of psychedelics on our psyche?
Despite the fact that psychedelics are illegal, the last decade has seen an explosion of research, with results so intriguing that governments are greenlighting studies around the world.
Scientists are busily exploring the role of hallucinogens on treatment-resistant depression, post traumatic stress disorder, cancer-related anxiety, addictions, and even anorexia.
But this is not the first time science became giddy over the potential benefits of psychedelics. That story began nearly a century ago.
The first trip on LSD
It was 1938 when Swiss chemist Albert Hoffman inadvertently synthesized lysergic acid diethylamide, or LSD, while trying to create a treatment for bleeding disorders. He shelved the compound for other research, then accidentally absorbed a small dose a few years later.
Intrigued by the feeling of euphoria, Hoffman tried it again, later realizing he had given himself five times the effective dose.
“The faces of those around me appeared as grotesque, colored masks,” Hoffman wrote in a first person account. “I sometimes observed, in the manner of an independent, neutral observer, that I shouted half insanely or babbled incoherent words. Occasionally I felt as if I were out of my body.”
Hoffman was tripping.
The golden era
Word spread quickly through the scientific community and soon researchers around the world began analyzing, then experimenting with LSD, both on themselves and their patients.
Their methods may not be considered state-of-the-art science today, but that didn’t stop the research. Science began to tackle other age-old hallucinogens: an extract from Mexican “sacred mushrooms” called psilocybin, and a naturally occurring psychoactive found in the peyote cactus called mescaline.
After all, these plant-based psychedelics have been in use by indigenous peoples and ancient cultures for hundreds, possibly thousands of years.
In the 1950s UK psychiatrist Dr. Humphry Osmond began giving LSD to treatment-resistent alcoholics: 40% to 45% of those who took LSD were still sober after a year. Other researchers duplicated his results.
Eager to label the effect of LSD on the mind, Osmond put together the Greek words psyche (mind) and deloun (show). The word psychedelic was born.
During the ’40s and early ’50s tens of thousands of patients took LSD and other psychotropics to study their effects on cancer anxiety, alcoholism, opioid use disorder, depression, and posttraumatic stress disorder or PTSD. Researchers began to see psychedelics as possible “new tools for shortening psychotherapy.”
Celebrity endorsements
Outside the control of a lab, people began touse psychedelics for their mind-bending effects, swearing the drugs improved creativity and made them happier long past the bliss of the high.
Celebrities helped spread the word: Gary Grant used LSD over 100 times in the late ’50s, according to the documentary film, “Becoming Cary Grant,” claiming it made him a better actor.
Grant was so taken with the drug that he decided to go public with his experience in the September 1, 1959, issue of Look magazine. Vanity Fair wrote about the article, entitled “The Curious Story Behind the New Cary Grant,” which was a glowing account of how LSD therapy had improved Grant’s life: “At last, I am close to happiness.”
Influential writer Aldous Huxley, best known for his 1932 novel “Brave New World,” took LSD during the last third of his life. In 1960 he told “The Paris Review”: “While one is under the drug one has penetrating insights into the people around one, and also into one’s own life. Many people get tremendous recalls of buried material. A process which may take six years of psychoanalysis happens in an hour — and considerably cheaper!”
The Leary impact
When Harvard psychologists Timothy Leary and Richard Alpert decided to open the Harvard Psilocybin Project in 1960, research on psychedelics was still in its golden era. That would soon change.
Leary and Alpert were fired in 1962 and their research shut down when Harvard discovered they had been giving LSD to their students. Alpert changed his name to Baba Ram Dass and became a best selling author and New Age guru. Leary began to speak out publicly, encouraging young people to take LSD recreationally. He quickly became the face of the drug counterculture movement with his signature message, “Turn on, tune in, drop out.”
“Drop out of school, because school education today is the worst narcotic drug of all,” Leary said. “Don’t politic, don’t vote, these are old men’s games.”
No longer administered in the relative safety of a lab or psychiatrist’s office, horror stories of bad “acid” trips at colleges and concerts shared headlines with images of anti-Vietnam protests and unclothed Woodstock attendees.
In 1966, LSD was declared illegal in the United States and research projects were closed or forced underground.
In 1970, President Richard Nixon signed the Controlled Substances Act into law. It classified hallucinogenics as Schedule I drugs — the most restrictive category — reserved for substances with “no currently accepted medical use and a high potential for abuse.”
A long dry spell is broken
Twenty five years passed. Then in the mid-’90s, a few scientists in Germany, Switzerland and the US again began to explore the mental and physical impact of psilocybin, mescaline, and a new player in the space: N-dimethyltryptamine or DMT. It’s the active ingredient in an ancient sludge-like brew called ayahuasca, which is used by spiritual healers in the Amazon.
Small, with very few participants and no randomization or other controls, the research was similar to “safety and tolerability” studies designed to prove no harm.
Trying to study illegal substances created challenges for researchers, but many persevered. As the years passed, the US Food and Drug Administration and the US Drug Enforcement Administration began to say “yes” more often than “no.”
Studies on psilocybin, DMT, and mescaline were approved, as were studies of the synthetic drug MDMA, more commonly known as “Molly” or “Ecstasy.”
Research on LSD, which had the worst reputation in the public’s eye, lagged behind until 2008. That’s when the Multidisciplinary Association for Psychedelic Studies, or MAPS, received FDA approval to study LSD-assisted psychotherapy on end-of-life anxiety. MAPS called the approval “a transformative moment.”
The study found “positive trends” in the reduction of anxiety after two sessions of LSD administered under the guidance of a psychotherapist.
Fears of any permanent damage from psychedelics were eased by a large 2015 study of 130,000 American adults, comparing users to non-users. The study found no link between the use of LSD, psilocybin or mescaline and suicidal behavior or mental health problems.
However, studies show a minority of people do experience “bad trips,” fueling speculation that the chance of negative experiences maydiffer depending on the type of hallucinogenic, the dose, even the type of mental disorder. In addition, research shows people who have used anti-depressants for a long time fail to respond well to some psychedelics, leading to concern about their use in chronic anti-depressant users.
To avoid negative experiences, MAPS and other organizations say having trained therapists on hand to guide one through the experience is key, along with a supportive setting, appropriate expectations and proper dosage.
A research renaissance
Today there is a true renaissance of research on the role of psychedelics on mental health.
“Gold-standard” double blind randomized trials have shown “rapid, marked, and enduring anti-anxiety and depression effects,” researchers say, in people with cancer-related and treatment-resistant depression after a single dose of psilocybin. Treatment with psilocybin has also improved obsessive compulsive disorder symptoms and alcohol dependence.
Dosage has become a focus of interest. “Micro-doses’ of shrooms and other psychedelics is a recent trend; users claim tiny, daily doses can improve mood and concentration without the commitment to a hours-long high. Research on micro-dosing is in the early stages.
MAPS is in the final phase of a gold-standard study administering MDMA [Ecstasy] to 300 people with severe PTSD from any cause. Results of the second phase showed 68% of the people no longer met the criteria for PTSD at a 12-month follow-up; before the study they had suffered from treatment-resistant PTSD for an average of 17.8 years.
The results are so positive that in January the FDA declared MDMA-assisted psychotherapy for PTSD a “Breakthrough Therapy.” MAPS hopes to turn the therapy into a FDA-approved prescription treatment by the end of 2021 to treat sexual assault, war, violent crime, and other traumas.
“We also sponsored completed studies of MDMA-assisted psychotherapy for autistic adults with social anxiety, and MDMA-assisted psychotherapy for anxiety related to life-threatening illnesses,” the group says.
Ayahuasca has been shown to significantly improve depression and appears to be helpful in treating alcohol, tobacco and cocaine addiction.
LSD has been shown to help anxiety, and studies find it provides a “blissful state” for the majority of users. Study participants report greater perceptiveness, insight, feelings of closeness to others, happiness, and openness. Some even say they experience long-term, positive restructuring of their moods and attitudes.
But some studies have found unpleasant effects from LSD, both during the high and after. People with negative reactions can have difficulty concentrating, dizziness, lack of appetite, dry mouth, nausea and/or imbalance for up to 10 to 14 hours after taking LSD; headaches and exhaustion can last up to 72 hours.
In the end, it’s too early for science to provide psychedelics a full seal of approval. One of the caveats of this research is that the drugs are administered with psychological support. When that is removed, studies found the benefits were minimal, and in rare cases, may even worsen mental health symptoms.
“Psychedelics amplify painful memories … and emotions,” said MAPS trained psychiatrist Dr. Will Siu in the Goop episode. Taking these drugs in unsupported settings, he said, can “be incredibly destabilizing, and you can actually feel worse in the short term.”
Long term, it appears research into psychedelics is here to stay. Perhaps one day soon a trip to the therapist will include a trip into your mind, and hopefully, a quicker path to healing.
Interesting Mushroom information (not a Psilocybin mushroom but has healing benefits …)
Lion’s Mane: A Mushroom That Improves Your Memory and Mood?
Mushrooms provide a vast array of potential medicinal compounds. Many mushrooms are well-known for these properties, but the lion’s mane mushroom, in particular, has drawn the attention of researchers for its notable nerve-regenerative properties.
By – Paul Stamets – Founder, Fungi Perfecti; Advisor, Program of Integrative Medicine at the University of Arizona Medical School, Tucson – 08/08/2012 – Updated December 6, 2017
Mushrooms provide a vast array of potential medicinal compounds. Many mushrooms — such as portobello, oyster, reishi and maitake — are well-known for these properties, but the lion’s mane mushroom, in particular, has drawn the attention of researchers for its notable nerve-regenerative properties.
Lion’s mane mushrooms are not your classic looking cap-and-stem variety. These globular-shaped mushrooms sport cascading teeth-like spines rather than the more common gills. From these spines, white spores emerge. Lion’s mane mushrooms also have other common names: sheep’s head, bear’s head and the Japanese yamabushitake. I like the clever name “pom pom blanc” — a reference to their resemblance to the white pom-poms cheerleaders use. The Latin name for lion’s mane is Hericium erinaceus; both names mean “hedgehog.”*
Lion’s mane mushrooms are increasingly sold by gourmet food chains. This nutritious mushroom is roughly 20 percent protein, and one of the few that can taste like lobster or shrimp (Stamets, 2005). Lion’s mane is best when caramelized in olive oil, deglazed with saké wine, and then finished with butter to taste. Lion’s mane can be bitter if not cooked until crispy along the edges. It takes some practice to elicit their full flavor potential.
Lion’s mane mushrooms are increasingly studied for their neuroprotective effects. Two novel classes of Nerve Growth Factors (NGFs) — molecules stimulating the differentiation and re-myelination of neurons — have been discovered in this mushroom so far. These cyathane derivatives are termed “hericenones” and “erinacines.” The levels of these compounds can vary substantially between strains, based on the measurements our team has conducted.
About a dozen studies have been published on the neuroregenerative properties of lion’s mane mushrooms since 1991, when Dr. Kawagishi first identified NGFs in Japanese samples. Since his original discovery, in vitro and in vivo tests have confirmed that hericenones and erinacines stimulate nerve regeneration. In 2009, researchers at the Hokuto Corporation and the Isogo Central and Neurosurgical Hospital published a small clinical study. Giving lion’s mane to 30 Japanese patients with mild cognitive impairment resulted in significant benefits for as long as they consumed the mushrooms:
“The subjects of the Yamabushitake group took four 250 mg tablets containing 96 percent of Yamabushitake dry powder three times a day for 16 weeks. After termination of the intake, the subjects were observed for the next four weeks. At weeks eight, 12 and 16 of the trial, the Yamabushitake group showed significantly increased scores on the cognitive function scale compared with the placebo group. The Yamabushitake group’s scores increased with the duration of intake, but at week four after the termination of the 16 weeks intake, the scores decreased significantly.” (Mori, 2009)
Recently, mice were injected with neurotoxic peptides in an experiment to assess the effects of lion’s mane on the type of amyloid plaque formation seen in Alzheimer’s patients. The mice were then challenged in a standard “Y” maze, designed for testing memory. Mice fed with a normal diet were compared to those supplemented with lion’s mane mushrooms. As the peptide-induced plaque developed, the mice lost the ability to memorize the maze. When these memory-impaired mice were fed a diet containing 5 percent dried lion’s mane mushrooms for 23 days, the mice performed significantly better in the Y maze test. Interestingly, the mice regained another cognitive capacity, something comparable to curiosity, as measured by greater time spent exploring novel objects compared to familiar ones.
The medical community is bracing for an increase of patients with Alzheimer’s and senile dementia as the baby boomer population ages. Mortality trends related to Alzheimer’s are outpacing death rates of many other diseases. This makes preventive and curative treatments of age-related cognitive diseases hot subjects of research. In the past 10 years, deaths from Alzheimer’s disease have surged roughly 66 percent, while deaths from other primary diseases have generally declined.
The influence of lion’s mane influence on neurological functions may also have other added benefits — making you feel good. In another small clinical study (n=30), post-menopausal women who consumed lion’s mane baked into cookies vs. those without showed less anxiety and depression yet improved in their ability to concentrate (Nagano et al., 2010).
Is this data conclusive thus far? No.
Is this data suggestive of positive outcomes? Absolutely.
In another small Japanese study with a randomized sample of 30 women, ingesting lion’s mane showed that “HE intake has the possibility to reduce depression and anxiety, and these results suggest a different mechanism from NGF-enhancing action of H. erinaceus.” (Nagano et al. 2010).
Lion’s mane may be our first “smart” mushroom. It is a safe, edible fungus that appears to confer cognitive benefits on our aging population. Unfortunately, lion’s mane is not available in most grocery stores. But you can buy kits to grow them at home, and organic lion’s mane supplements are available at some health food stores. If you are skilled enough and looking for adventure, you can forage for them by hunting in the hardwood forests of North America, Europe and Asia during the summer and fall.**
**Before consuming any wild mushroom, make positively sure that it is accurately identified. For a list of mycological societies, which may be able to help you, go to the North American Mycological Association website: www.namyco.org.
References:
Kawagishi, H., Ando, M., Sakamoto, H., Yoshida S., Ojima, F., Ishiguro, Y., Ukai, N., Fukukawa, S. 1991. “Hericenone C, D and E, stimulators of nerve growth factor (NGF) synthesis from the mushroom Hericium erinaceum.” Tetrahedron Lett 32, 4561-4564.
Mori, K., Inatomi, S., Ouchi, K. Azumi, Y and Tuchida T. 2009. “Improving effects of the mushroom Yamabushitake (Hericium erinaceus) on mild cognitive impairment: a double blinded, placebo controlled clinical trial.” Phytother Res. 23:367-372.
Mori, K., Obara, Y., Moriya, T., Inatomi, S., Nakahata, N. 2011. “Effects of Hericium erinaceus on amyloid β(25-35) peptide-induced learning and memory deficits in mice.” Biomed Res. 32(1):67-72.
Nagano, M., Shimizu, K., Kondo, R., Hayashi, C., Sato, D., Kitagawa, K., Ohnuki, K. 2010. “Reduction of depression and anxiety by 4 weeks Hericium erinaceus intake.” Biomed Res. 31(4):231-7.
Story from HuffPost
A Single Dose of Psilocybin Mushrooms Can Reduce Anxiety for Nearly Five Years
By Chris Moore | News | January 14, 2020
A 2016 study found that a single dose of shrooms can significantly reduce cancer patients’ fear of death, and a new follow-up study has found that these benefits can last for years.
Nearly five years ago, a team of researchers conducted a landmark trial exploring whether psilocybin, the compound in magic mushrooms that makes us trip balls, could reduce anxiety in patients suffering from lethal forms of cancer. Since then, researchers’ interest in exploring the therapeutic potential of Psilocybe cubensis has skyrocketed.
Several clinical trials in the last half-decade have concluded that psilocybin can effectively treat anxiety, depression, and other conditions. That’s why the federal government is now seriously considering legalizing this natural psychedelic as an adjunct to therapy.
In the original 2016 study, researchers gave a single dose of psilocybin to 29 people suffering from life-threatening forms of cancer. Each of these patients was previously diagnosed with anxiety and/or depression as a direct result of their illness. Six months after taking this single dose, between 60 and 80 percent of patients reported a significant reduction in symptoms of depression and anxiety.
Years later, the original research team followed up with patients from the original study to see if the positivity generated from the psilocybin experience was still in effect. Out of the surviving 16 patients, 15 agreed to take additional psychological assessments between 3.2 and 4.5 years after the initial study.
“Reductions in anxiety, depression, hopelessness, demoralization, and death-anxiety were sustained at the first and second follow-ups,” the authors wrote in the follow-up study, published in the Journal of Pharmacology. At the second follow-up, 4.5 years after the original study, 60 to 80 percent of patients still showed signs of decreased anxiety and depression. “Participants overwhelmingly (71-100%) attributed positive life changes to the psilocybin-assisted therapy experience and rated it among the most personally meaningful and spiritually significant experiences of their lives.”
The authors also asked participants to describe how their psychedelic experience changed their outlook on life. “I experienced such overwhelming love in my psilocybin experience that it gave me new confidence,” one subject responded, according to IFLScience. “I think the extreme depth of love I felt changed the way I relate to others. [It] gave me a feeling that I have a right to be here and to enjoy life.”
Another participant said that “the psilocybin experience changed my thoughts about myself in the world… I see myself in a less limited way. I am more open to life. It has taken me out from under a big load of feelings and past issues in my life that I was carrying around.”
“These findings suggest that psilocybin-assisted psychotherapy holds promise in promoting long-term relief from cancer-related psychiatric distress,” the study concludes.
The authors note that the study does have its limitations, especially due to its small subject pool. But that doesn’t take away from the study’s positive implications. “Nonetheless, the present study adds to the emerging literature-base suggesting that psilocybin-facilitated therapy may enhance the psychological, emotional, and spiritual well-being of patients with life-threatening cancer.”
Story from MerryJane
Johns Hopkins Scientists Give Psychedelics the Serious Treatment
The first research center of its kind in the country is bringing renewed rigor to the investigation of the drugs’ therapeutic uses
By Tanya Lewis on
Psychedelic drugs—once promising research subjects that were decades ago relegated to illicit experimentation in dorm rooms—have been steadily making their way back into the lab for a revamped 21st-century-style look. Scientists are rediscovering what many see as the substances’ astonishing therapeutic potential for a vast range of issues, from depression to drug addiction and acceptance of mortality. A frenzy of interest has captivated a new generation of researchers, aficionados and investors, triggering some understandable wariness over promises that may sound a little too good to be true. But late last year the highly respected institution Johns Hopkins University—the U.S.’s oldest research university—launched a dedicated center for psychedelic studies, the first of its kind in the country and perhaps the world’s largest. With work now underway, the center is aiming to enforce the strictest standards of scientific rigor on a field that many feel has veered uncomfortably close to mysticism and that has relied heavily on subjective reports. Early results have been promising and seem poised to keep the research on a roll.
Psilocybin (a psychoactive compound found in certain mushrooms) and LSD were widely studied in the 1950s and 1960s as treatments for alcoholism and other maladies. They later gained a reputation in the media and the public eye as dangerous and became strongly associated with the counterculture. Starting in 1966, several states banned their use. In 1968 LSD was outlawed nationwide, and in 1970 Congress passed the Controlled Substances Act, classifying that drug and psilocybin, along with several others, as having a high potential for abuse and no accepted medical use. But in recent years a rapidly growing number of studies reporting encouraging results in treating depression, addiction and post-traumatic stress disorder (PTSD) have brought them back out of the shadows, spurred on by positive media coverage.
In a major boost to the reviving field, Johns Hopkins’s Center for Psychedelic and Consciousness Research is exploring the use of psychedelics—primarily psilocybin—for problems ranging from smoking addiction to anorexia and Alzheimer’s disease. “One of the remarkably interesting features of working with psychedelics is they’re likely to have transdiagnostic applicability,” says Roland Griffiths, who heads the new facility and has led some of the most promising studies evaluating psilocybin for treating depression and alcoholism. The myriad applications suggested for these drugs may be a big part of what makes them sound, to many, like snake oil—but “the data [are] very compelling,” Griffiths says. And psychedelics may not only hold hope for treating mental disorders. As Griffiths puts it, they provide an opportunity to “peer into the basic neuroscience of how these drugs affect brain activity and worldview in a way that is ultimately very healthy.”
As author Michael Pollan chronicles in his 2018 best seller How to Change Your Mind, researchers were examining the therapeutic effects of psychedelics in the 1950s—a decade before then Harvard University psychologist Timothy Leary and his colleague Richard Alpert started their notorious study in which they gave psilocybin to students (ultimately leading to Leary’s and Alpert’s dismissal from the university). In the 1950s–1970s, studies conducted with LSD—which acts on the same brain receptors as psilocybin—reported strong results in treating substance use disorders, including alcohol and heroin addiction. But when LSD became illegal in 1968, funding for this work gradually dried up. Most psychedelics research stopped or went underground.
PSYCHEDELICS’ NEW WAVE
Griffiths and some of his colleagues helped revive the field around 2000, when they obtained government approval to give high doses of psilocybin to healthy volunteers. The researchers published a foundational study in 2006 showing a single dose was safe and could cause sustained positive effects and even “mystical experiences.” A decade later they published a randomized double-blind study showing psilocybin significantly decreased depression and anxiety in patients with life-threatening cancer. Each participant underwent two sessions (a high-dose one and a low-dose one) five weeks apart. Six months afterward, about 80 percent of the patients were still less clinically depressed and anxious than before the treatment. Some even said they had lost their fear of death.
Armed with these promising results, Griffiths and his colleagues turned their attention to other clinical applications. They decided to investigate tobacco addiction—in part because it is much easier to quantify than emotional or spiritual outcomes. Johns Hopkins researcher Matthew Johnson led a small pilot study in 2014 to see whether psilocybin could help people quit smoking. It was an open-label study, meaning the participants knew they were getting the drug and not a placebo.
The work followed a classic model for psychedelic therapy in which the participant lies on a couch and wears eyeshades while listening to music. Researchers do not talk to or guide subjects during the trip, but before each session, they do try to prepare people for what they might experience. In Johnson and his colleagues’ study, participants also underwent several weeks of cognitive-behavioral therapy (talk therapy aimed at changing patterns of thinking) before and after taking psilocybin. The drug was given in up to three sessions—one on the target quit date, another two weeks later and a third, optional one eight weeks afterward. The subjects returned to the lab for the next 10 weeks to have their breath and urine tested for evidence of smoking and came back for follow-up meetings six and 12 months after their target quit date.
At the six-month mark, 80 percent of smokers in the pilot study (12 out of 15) had abstained from cigarettes for at least a week, as verified by Breathalyzer and urine analysis—a vast improvement over other smoking cessation therapies, whose efficacy rates are typically less than 35 percent. In a follow-up paper, Johnson and his colleagues reported that 67 percent of participants were still abstinent 12 months after their quit date, and 60 percent of them had not smoked after 16 months or more. Additionally, more than 85 percent of the subjects rated their psilocybin trip as one of the five most meaningful and spiritually significant experiences of their lives. The team is currently more than halfway through a larger, five-year study of 80 people randomized to receive either psilocybin or a nicotine patch at the new Johns Hopkins center. Recruitment for the study is ongoing.
The exact brain mechanism by which the therapy appears to work remains unclear. At the psychological level, Johnson says, there is evidence that the sense of unity and mystical significance many people experience on psilocybin is associated with greater success in quitting, and those who take the drug may be better able to deal with cravings. At the biological level, he adds, scientists have hypothesized that psilocybin may alter communication in brain networks, possibly providing more top-down control over the organ’s reward system. A team led by Johns Hopkins cognitive neuroscientist Frederick Barrett is now investigating further by using functional magnetic resonance imaging to measure brain activity before and after patients undergo the therapy.
Like any drug, psilocybin comes with risks. People with psychotic disorders such as schizophrenia (or a strong predisposition for them) are generally advised against taking the hallucinogen. People with uncontrolled hypertension are advised to abstain as well, because psilocybin is known to raise blood pressure. Although it appears to be one of the safest “recreational” drugs and is not considered addictive, there have been reports associating it with deaths—but these may have been the result of multiple drugs, impure substances or underlying medical issues. In the smoking study, a third of participants experienced some fear or anxiety at a high dose of the psilocybin, Johnson says. But he adds that the risks can be minimized by carefully selecting participants and administering the drug in a controlled environment.
The smoking study results are promising, but Johnson says its relatively small size is a limitation. Also, subjects in such studies cannot comprise a completely random sample of the population, because it would be unethical to recruit people without telling them they may be taking a psychedelic drug. Thus, participants tend to be people who are open to this category of experience and, potentially, more apt to believe in its efficacy. And it is also hard to tease apart the effects of psilocybin from those of the cognitive-behavioral therapy in the smoking study, Johnson notes. He and his colleagues at the new center plan to conduct a double-blind, placebo-controlled study—the gold standard for medical investigations—in the future. Johns Hopkins researchers are also starting or planning studies using psilocybin therapy for a wide range of other conditions, including opioid addiction, PTSD, anorexia, post-treatment Lyme disease syndrome, Alzheimer’s disease and alcoholism in people with depression.
David Nichols, a professor emeritus of pharmacology at Purdue University, who was not involved in the recent Johns Hopkins studies but had synthesized the psilocybin used in Griffiths’s 2006 and 2016 papers, has been conducting research on psychedelics since the late 1960s. Back then, “you probably could have counted on one hand the number of people in the world that were working in this field. There wasn’t any money; there was no interest. [Psychedelics] were just looked at as drugs of abuse,” he says. Now “there’s a whole society set up to study these, with probably 150 international scientists working on it.”
Nichols says he has supported Griffiths’s and Johnson’s work since its early days, as they gathered the initial data that excited wealthy donors enough to fund the latest research. Philanthropic funding “is the way it’s going to be—until the National Institutes of Health decide that this is a field worth funding,” he says. “There are still too many political considerations that are keeping that from happening, but eventually, we’ll get there. We’ll get institutional support. We’re just not there yet.”
Story from Scientic American
Psychedelic Events Are Going Mainstream, Where The Much-Maligned Mushroom Industry Focuses On Mental Health
Sara Brittany Somerset
Sara Brittany Somerset – Contributor – Forbes- Jan 12, 2020
Psychedelics have been a mainstay for a millennia and appreciated in the counter-culture for decades. In 2020, whether consuming, investing, or both, mushrooms are having a moment.
PsychedeliTech, a ground-breaking new conference, incubator and discovery platform for psychedelic medicine will host Rick Doblin, Ph.D., Founder and Executive Director of the Multidisciplinary Association for Psychedelic Studies (MAPS) as the keynote speaker at the first-ever PsyTech Summit, a forum for psychedelic science, innovation and investment conference, in Israel.
The inaugural PsyTech conference will take place March 29-30, 2020 at the Hilton Hotel, on the Mediterranean Sea in Tel Aviv.
PsyTech is a division of iCAN: Israel-Cannabis, which together with CannaTech, its medical cannabis events platform, has been a global participant in education and innovation for cannabis therapeutics and products with conferences in London, Sydney, Hong Kong, Panama and Cape Town, to date.
Saul Kaye, iCAN founder and CEO, said, “Rick Doblin is an early pioneer and extremely effective advocate for the potential of psychedelics in the treatment of mental health disease and symptoms, including depression, anxiety disorders, and PTSD. We are thrilled he will join us at our first PsyTech Summit in Tel Aviv to share his enlightened vision and vast knowledge of the fast-developing therapeutic ecosystem that is about to explode as a wave of new information, research and consumer interest about psychedelics floods the market.”
For the first 30 years of MAPS’ dedicated research, there were virtually no for-profit psychedelic business opportunities, apart from a few ibogaine and ayahuasca clinics and mushroom sales in countries where the substances are legal.
Psychedelics have the potential to impact and improve mental health.
For-profit entities emerging in the field of psychedelics, such as Cybin with microdosed psilocybin products and Mind Med with synthetic ibogaine, are directly due to the success of non-profit psychedelic therapy research, including the lifelong work of MAPS and other advocates.
Story From Forbes
Will Shroom Dispensaries Become a Thing Anytime Soon?
With the decriminalization of psilocybin, it’s hard not to wonder whether magic mushrooms will follow the path of cannabis.
Miro Tomoski – January 6, 2020
Imagine the sinking feeling that would barrel down your gut at the sight of DEA agents waiting at your door as you leave for work in the morning. Count the things they seized from your apartment: a notebook, an iPhone, a computer tower, a few graphic t-shirts, 906 live psilocybin mushrooms, and just over 20 ounces of dried shrooms. Late for your job in the legal cannabis industry, you begin to wonder what’s so bad about selling some homegrown medicine? After all, the city had just decriminalized psilocybin (the main psychoactive compound in magic mushrooms), and it’s only a matter of time before it’s sold in storefront shroomeries just like cannabis.
That is how Kole Milner spent one September morning, just five months after citizens voted in May of 2019 to decriminalize the possession of psilocybin mushrooms in his hometown of Denver. The agents never arrested Milner, though he knew exactly what he was doing: By his own admission he’d been selling psilocybin mushrooms, on a publicly accessible Venmo account—long before the Denver Psilocybin Initiative had them deemed the lowest level crime he could commit in the city. He had even told reporters at the Denver Post, NPR, VICE, and Westword what was growing mushrooms in his closet, while wearing a shirt branded with his own one-of-a-kind logo for a company called Happy Fox Edibles.
Even so, Milner still hasn’t been charged with a crime, despite having led law enforcement right into his living room. The investigation is still ongoing according to Jeff Dorschner, a spokesman for the US Attorney’s Office for the District of Colorado. This leaves open the possibility that Milner could face criminal charges, but his non-arrest in a city that now considers the possession of magic mushrooms to be a minor offense leaves us wondering when—if ever—psilocybin will be legal enough to sell.
“I believe it will be a long time until we see psilocybin dispensaries,” says Kevin Matthews, the architect of the ballot initiative that decriminalized psilocybin in Denver County last spring. “Anything is possible, but we have a tremendous amount of public education and data-collection to do before we can start having a serious dialogue about retail psilocybin.”
A synthetic version of psilocybin has already been granted “breakthrough therapy” status by the FDA to accelerate its route to market as a prescription medication for use in assisted-psychotherapy for depression. The nonprofit organization Usona and the for-profit company Compass Pathways are behind this drug development. Meanwhile, scientists at institutions like Johns Hopkins or New York University are also researching psilocybin for addiction, mysticism, anorexia, and various other applications.
The pharmaceutical model, with all its exclusivity, encourages people like Milner to continue growing mushrooms at home in order to avoid high price tags and to circumvent the need for a prescription, especially without a qualifying diagnosis. It may even push those who don’t qualify for the FDA-approved treatment to seek out people like Milner as caregivers to facilitate access to the psilocybin they need.
Story From DoubleBlindMag
There’s Now a Federal Psychedelic Lobby
They started in Denver—and they’re taking the movement nationwide
Miro Tomoski – October 21, 2019
Kevin Matthews let out a laugh when asked if psilocybin—the primary psychoactive component in magic mushrooms—had ever helped him. “It saved my life,” he says. The former cadet had high hopes for his time at West Point, one of the world’s finest military academies, but service-related depression forced him to be honorably discharged. It wasn’t until he discovered psilocybin that he found relief—and was catapulted back into public service, but, this time, of a very different nature.
In May, Matthews led the nation’s first successful effort to decriminalize psilocybin in the county of Denver. Initiative 301, which made the use and possession of psilocybin the lowest priority for law enforcement, passed by a nail-biting margin of 50.6 percent to 49.4 percent. Now more than 90,000 Denver residents are counting on Matthews to make sure that their hard-won victory doesn’t end at the ballot box.
Always projecting one step ahead, Matthews had registered a nonprofit in Colorado a full year before the vote: the Society for Psychedelic Outreach, Reform, and Education. Otherwise known as SPORE, the group is considered to be the new psychedelic lobby—joining the ranks of other suits on Washington DC’s K Street who push for influence among the powerful.
“We’re not going to be lobbying, but we’re definitely going to be supporting groups and organizations that are doing that,” Matthews says. SPORE’s main focus is education, he adds, as well as filling in the gaps between what the voters want the law to look like and what policy is realistic in a world with competing interests. At the moment, SPORE is focused on ensuring that decriminalization works as it was intended to in Denver.
To many of us, drug legalization or decriminalization seems as if it should be rather straightforward. Voters cast their ballots, and the very next day they can no longer be arrested for possessing that substance. But while we’d all like to believe democracy is as simple as voting for or against something (or someone), each election day is often followed by a mad scramble of public officials, law enforcement, bureaucrats and business interests working behind the scenes to define the new normal.
When a previously illegal substance is added to that mix, a county like Denver becomes saddled with awestruck community leaders who now must grapple with something they’ve spent most of their lives avoiding. The best example we have of these behind-the-scenes negotiations has been the legalization of cannabis, forcing state officials all over the country to consider possession limits, retail licensing, zoning provisions, and other unprecedented questions around possession, sale, and production of the substance.
SPORE hopes to accelerate this process by coordinating with legal experts, medical professionals, and lawmakers in order to put these changes into practice in a way that’s faithful to what voters envisioned when they cast their ballots.
In Denver, the decriminalization process begins with a Psilocybin Policy Review Panel, which was written into Initiative 301 and includes members of city council, medical experts, law enforcement, and a representative of the team who wrote the initiative. The panel, which is expected to be formed by the end of October, is meant to ensure that the measure is implemented without restrictive roadblocks. (See Massachusetts which took more than two years to open a dispensary after voters legalized recreational cannabis.)
Having met with officials in the mayor’s office and twice with the District Attorney since election day, Matthews is now thinking about everything from roadside ads for responsible use to training first responders in harm reduction tactics. And that’s not to mention possession limits, which he hopes to eliminate entirely when it comes to personal use.
In essence, SPORE is Matthews’ attempt to give the people of his community exactly what they voted for—but it also offers assistance and expertise to anyone who’s looking to replicate Denver’s success across the country. The idea is to bring together proponents of decriminalization into one cohesive political force.
With the exception of cannabis, which has found unifying political voices in national organizations like NORML (the National Organization for the Reform of Marijuana Laws), DPA (the Drug Policy Alliance), and the Marijuana Policy Project, efforts to decriminalize other psychoactive substances have largely been organized on a local level. These grassroots activists have had to build their organizations from the ground up and rely on research-based evidence coming out of organizations like MAPS (the Multidisciplinary Association for Psychedelic Studies).
Among these individuals is Ryan Munevar, campaign director of Decriminalize California, who now faces the colossal task of convincing nearly 20 million registered voters throughout the state to turn out in support of psilocybin decriminalization. While the city of Oakland already passed an all-plant decriminalization measure, and while Denver has shown that an election can be won with a paper-thin margin, California is often feared as the most expensive state in which to run a political campaign. (Moreover, a 2018 attempt at a similar initiative failed to gather enough signatures.)
Matthews learned the same hard lessons when his first two petitions to put a decriminalization question on the ballot in November of 2018 were denied by elections officials in Denver before they even reached voters. But Munevar is still optimistic, having consulted with Matthews and drawn inspiration from his success.
“Honestly we might even be able to swing a lot of Republicans to our side,” Munever says, pointing out that right-leaning voters were a base of support for the Denver initiative. In fact, garnering support from more conservative voters could be another important part of SPORE’s mission. Where evidence from FDA-approved psilocybin research from institutions like Johns Hopkins provides the data to support decriminalization, SPORE could mobilize the electorate to vote for it.
By the end of the year, SPORE aims to conduct statewide polling in Colorado to determine how residents feel about psilocybin decriminalization on a larger scale. But for now, Matthews has focused his efforts on finishing what he started in Denver with an eye toward taking SPORE to Washington DC and creating a nationwide movement.
Just like any other successful lobby, from the NRA to the AARP, identifying voters who will show up for the cause is a crucial part of convincing Congress to act.
“It’s unlikely that Denver city councilors were going to wake up one morning and say ‘I think we really need to look at the therapeutic benefits of psilocybin’ without the voters telling them to do so,” says attorney Noah Potter, a legal advisor to the Decriminalize Denver campaign and founder of the New Amsterdam Psychedelic Law blog.
Potter calls this group of voters the “psychedelic constituency,” and the advantage is that they play on both sides of the political spectrum. That’s good news for SPORE because it means that voters who otherwise favor one party all the way down the ballot might stop to consider a decrim question.
“I’ll say it this way, we got endorsements from the Green Party and the Libertarian Party,” says Matthews, suggesting that folks with various political beliefs support decriminalization—at least in Colorado. “From our experience we’ve seen that people from all walks of life are interested in this.”
It also means that SPORE could have a wide base of donors to back their efforts. With an eye toward a national decriminalization campaign, they are currently applying for 501(c)(3) status with the IRS, which would allow them to collect donations as a charitable organization with the potential to one day become a 501(c)(4), or an organization that can take direct political action and receive unlimited anonymous donations.
Matthews wouldn’t be the first to take this route of activism—in fact, the Oregon Psilocybin Society has already been approved by the IRS under the 501(c)(3) category—but his national aspirations make SPORE unique.
“We intend to get in contact with federal policymakers and learn more about what each party is focused on in terms of psychedelics, whether it be economics or social justice,” Matthews tells DoubleBlind, expressing a bit of frustration with the current field of presidential candidates. “I want to see a drug policy debate during this election cycle.”
Still, while presidential hopefuls have so far kept their distance from the issue, New York Rep. Alexandria Ocasio-Cortez has not shied away and even tried to add an amendment to a broader government spending bill which would have made it easier to study psychedelics. “From the opioid crisis to psilocybin’s potential w/ PTSD, it’s well past time we take drug use out of criminal consideration + into medical consideration,” the freshman Congresswoman tweeted after introducing her amendment in June.
Her efforts were blocked by members of Congress, but the attempt showed that there is an appetite for reform among what Matthews calls the Psychedelic Caucus—a group of potential allies on Capitol Hill composed of AOC, as well as Democrat Reps. Rho Khanna and Lou Correa of California, and even Republican Rep. Matt Gaetz of Florida.
“Our victory in Denver was a clear indication that there is now a political foundation for the psychedelic renaissance,” Matthews says. And in the coming months, if SPORE is able to demonstrate that enough voters care about decriminalization, Denver could be just the beginning.
Story From DoubleBlindMag
Title
