We won. The Federal Court overturned Health Canada’s refusal to allow psilocybin for cluster headache patient, Jody Lance.
The decision was “unreasonable”, lacking intelligibility, justification, and transparency, and it failed to engage with arguments about the patient’s s. 7 Charter rights.
The Court ordered a redetermination by a different decision maker, giving strong directions to Health Canada that they must meaningfully grapple with Charter submissions.
So far, the Special Access Program has consistently ignored any and all Charter arguments made by doctors and patients, simply pretending they do not exist. This decision should put an end to that. The Court also criticized Health Canada for failing to grapple with the numerous other submissions made.
It’s a first step forward for medical psilocybin, but not the last.
Full decision and written legal arguments are posted – Follow this LINK
Nicholas Pope
Lawyer at Hameed Law | Federal Admin Law and Charter
Calgary man could get assisted death but can’t get access to medical ‘magic mushrooms’
Health Canada has been ordered to reassess cluster headache patient Jody Lance’s request for psilocybin, a compound in ‘magic mushrooms’
Lance and his legal team took the matter to the Federal Court of Canada, which last week overturned Health Canada’s decision, ruling the refusal to grant Lance access to psilocybin was unreasonable and lacked the “requisite degree of justification, intelligibility and transparency.”
Among other transgressions, the judge said Health Canada “wholly disregarded” legal arguments that Lance has a Charter right to access the psychedelic.
Cluster headaches are rare. They attack suddenly, “like a clap of thunder,” causing sharp, stabbing pain on one side of the head. They can last anywhere from 15 minutes to three hours, recur multiple times a day and come on in clusters lasting weeks or months. Symptoms include droopy eyelids, facial swelling, fever, nausea and vomiting. It’s not clear what causes the attacks, but psychedelics have been gaining traction as a potential therapy.
Over the years, Lance has tried “tonnes of different treatments” prescribed by multiple specialists, “but was basically told, ‘There’s nothing we can do; we can’t figure this out,’” Pope said.
Lance eventually found his way to Calgary neurologist William Davenport, who, after numerous unsuccessful attempts to treat his cluster headaches with conventional therapies, suggested Lance try hallucinogenic mushrooms. Another patient of Davenport’s found they helped.
It’s absurd: If he couldn’t get access to this treatment, then MAID really would be a legitimate possibility
Lance experimented with different dosages, eventually setting on a regimen that works. He doesn’t get high, or experience hallucinations. Magic mushrooms haven’t cured his headaches, but they make them bearable and help abort some attacks.
Health Canada has authorized 153 requests for psilocybin, a restricted drug, under the SAP since 2022, though none for cluster headaches.
In addition to Davenport, Lance’s request was supported by a specialist in pain medicine and a clinical pharmacist.
In 22 pages of Charter arguments, Pope, an Ottawa-based human rights lawyer and legal advisor for TheraPsil, a B.C.-based non-profit that helps people secure legal access to psilocybin for medical needs, argued that his client has a right to access the drug under Section 7, which guarantees the right to life, liberty and security of the person. Pope argued Lance’s liberty was engaged based upon his right to make reasonable medical choices, his security of person was threatened by any delay in gaining access to an effective treatment and his life was at risk “due to his suicidal ideation and potential eligibility for MAID,” Fothergill wrote.
Fothergill found Health Canada “failed entirely” to consider the Charter arguments.
Health Canada’s assessors also argued that other “modalities” hadn’t been ruled out — specifically, a monoclonal antibody that is administered via injection that Pope said is “ridiculously expensive” and ineffective. In one study, 70 per cent of people saw no benefit.
Davenport testified that he couldn’t ethically require Lance to “impoverish himself” by trying a treatment that isn’t likely to work and that carries a considerable risk of side effects “when he has already found a treatment that is affordable, efficacious and has no side effects.”
A Health Canada senior manager commented that the Special Access Program doesn’t factor in cost “when ruling out marketed alternatives.”
At one point, government lawyers argued that psilocybin’s safety remains an open question, citing a case involving a man, high on magic mushrooms, who stabbed his father to death with a knife. Charged with manslaughter, he argued his actions were involuntary because of his state of intoxication.
But Fothergill said the “uncontested evidence” in Lance’s case is that the dose of psilocybin he’s seeking wouldn’t cause him to experience hallucinations of any kind, “let alone render him intoxicated to the point where his actions would no longer be voluntary.”
In addition to ignoring the Charter arguments, the judge said Health Canada’s senior assessor didn’t “meaningfully grapple” with other key issues raised by Lance and his neurologist, “calling into question whether he was fully alert and sensitive to the matter before him.”
The court ordered a “redetermination” by a different decision-maker. Health Canada has 14 days to render its decision.
Story from – National Post
Health Canada must reconsider man’s bid to use magic mushrooms for cluster headaches, Federal Court rules
Ministry’s denial of Calgary man’s request for medical grade psilocybin ‘unreasonable,’ judge says
A 51-year-old Calgary man who suffers debilitating cluster headaches has won a Federal Court battle forcing Health Canada to reconsider his bid for legal access to psilocybin to treat his extreme pain.
Ottawa Federal Court Judge Simon Fothergill, on May 24, granted an application for judicial review of Health Canada’s denial of Jody Lance’s bid for legal access to medical grade psilocybin — the active ingredient in hallucinogenic mushrooms — to manage pain associated with the headaches, which is so bad they have earned the nickname “suicide headaches.”
That decision — which also highlighted the need to consider a patient’s Charter rights — is being hailed by others fighting to access psilocybin for medical reasons.
Requests to access controlled substances in special medical circumstances are filed through Health Canada’s Special Access Program (SAP). In their July 12, 2023, SAP application Lance and his Calgary neurologist, William Jeptha Davenport, requested legal access psilocybin to help treat pain. Health Canada denied the request due to lack of research into the efficacy of the drug to treat cluster headaches.
Ruling a major step forward, advocate says
Last week’s ruling gave the health ministry 14 days to reconsider Lance’s request and to take his Charter rights into more careful consideration. Fothergill called the decision to deny Lance access to the drug “unreasonable” and “unintelligible.”
Health Canada told CBC News via email that it has noted the court’s decision and will comply with the judgment.
In an email to CBC News, Lance said he hopes this ruling helps others like him who are seeking safe, legal options to avoid what he called an “unnecessarily difficult journey.”
“It’s a first step in the right direction,” wrote Lance, a former land surveyor.
Spencer Hawkswell, president of the psychedelic advocacy group TheraPsil, described the ruling as a major step forward that makes clear that “what these patients are asking for is not ridiculous.”
“This is the first time that we’ve actually had the courts and a judge say a [Health Canada] decision lacks that justice and intelligibility,” he said.
Pain from cluster headaches
The Mayo Clinic describes cluster headaches as a rare, painful form of headache often involving “extreme sharp or stabbing pain” often around the eyes, in the head or neck that can last for weeks. According to experts, the exact causes remain unclear.
Ottawa human rights lawyer Nicholas Pope, who helped prepare Lance’s exemption application, described cluster headaches as “one of the most painful conditions known to humanity.” He noted that some studies comparing pain levels of different conditions suggest they are more painful than gunshot wounds, kidney stones or childbirth.
Fothergill cited experts in his ruling who described cluster headaches as “capable of inflicting the most severe pain known to science.”
In recent years there’s been emerging evidence suggesting psilocybin can help relieve pain for some who suffer from the headaches, with at least one clinical trial observing a small reduction in cluster headache attacks in participants who were given the drug.
Health Canada is facing pressure to speed up research into the therapeutic potential of magic mushrooms to help people facing significant mental health issues, including PTSD. CBC’s Joel Ballard visits a legal psilocybin grow-op and breaks down the demand, the potential benefits and the red tape.
In 2022, Peter McAllister, the medical director of the New England Institute for Neurology and Headache, wrote then Health Minister Jean-Yves Duclos in support of Canada allowing legal exemptions for the use of psilocybin for cluster headaches, which he described as an “agonizingly painful condition that can push patients to suicide to escape the suffering.”
McAllister wrote that in his experience, “many cluster headache patients obtain outstanding results using psilocybin-containing mushrooms,” which he said helped prevent episodes with little danger or side effects.
Pope, the human rights lawyer, says it was the same for Lance.
“He tried a whole laundry list of medications and dozens of different combinations,” Pope said. “Some worked for a brief period of time and then stopped working, or even made the headaches worse.”
He argued that by denying Lance access to psilocybin, federal authorities infringed on his Charter right to make reasonable medical choices regarding his physical and mental wellbeing.
The ruling noted that this infringement was exacerbated by delays and risked Lance’s life due to his suicidal ideation and the fact that he could potentially be eligible for medical assistance in dying (MAID).
Pope says the process for becoming approved to use psilocybin legally in Canada seems more difficult than applying for MAID.
“He’s found a treatment that works for him and makes life bearable. But it’s absurd: If he couldn’t get access to this treatment, then MAID really would be a legitimate possibility.”
“Mr. Lance should be allowed to use this for medical purposes with dignity and not be called a criminal for it,” Pope said.
Psilocybin controls
Psilocybin has been legal for Canadians to access in a limited way under the Special Access Program since 2022. As of November 2023, Health Canada had authorized 153 requests for 161 patients.
Ian MacKay, the SAP manager for Health Canada’s office of clinical trials, told federal court he has a 13-member team that handles about 1,000 requests and 800 phone calls per month, many of which are medical emergencies.
Lance has suffered from cluster headaches for seven years and has tried to treat his condition with prescribed medications. When they failed, the neurologist suggested other patients had found relief using hallucinogenic mushrooms, which was when Lance first tried them himself, his lawyer explained.
Lance will know within a few weeks if he will finally be able to get legal doses of the controlled substance. If he is denied, his legal team plans to return to court to fight.
“I would much prefer if I could put all my focus toward trying to get better rather than on court proceedings, but I am doing this in the hope that others in my situation will not need to go through this,” Lance wrote to CBC on Wednesday.
The Canadian Medical Association and the Canadian Neurological Sciences Federation declined comment on the case.
Story from – CBC News
Mushroom Joe? How President Biden could reschedule psilocybin like marijuana
President Joe Biden’s revolutionary proposal to move marijuana to Schedule 3 of the Controlled Substances Act might mean the end of more than 50 years of “failed policy” as well as new opportunities in science and business.
But such a move wouldn’t change the federal government’s classification of psilocybin as more dangerous than the fentanyl fueling the country’s overdose crisis.
Rescheduling Mushrooms
The Controlled Substances Act still classifies psilocybin mushrooms as a Schedule 1 drug – the same designation currently shared by marijuana.
And in the same paradox that’s bamboozled marijuana researchers and reform advocates, it is hard to conduct the necessary research proving psilocybin’s relative safety and therapeutic potential until restrictions are relaxed.
Could President Biden or the U.S. Congress turn to psilocybin rescheduling after the marijuana job is completed (whenever that might be)?
They absolutely could, says Andrew Livingston, the Denver-based director of economics and research at the Vicente law firm, but the formula won’t be the same as it’s been for marijuana.
That’s because the way states are legalizing psychedelic therapy is different from how marijuana has been legalized, with consequences that policymakers and advocates should consider when shaping state and local reform.
“Psychedelics and cannabis share similarities,” said Livingston, a keynote speaker at The Emerald Conference, set for April 1-3 in San Diego.
“They are both Schedule 1 drugs burdened by cultural stigma and drug war hysteria. They have clear medical benefits but are also used for recreational and spiritual purposes.
“Psychedelics and cannabis are also simultaneously undergoing state and federal policy reform. But their method of regulation is starkly different.”
‘Breakthrough therapy?’
The cornerstone of the emerging legal psychedelics industry, mushrooms were declared a “breakthrough therapy” for major depressive disorder and treatment-resistant depression by the U.S. Food and Drug Administration in 2018 and 2019.
Scientists at prestigious universities such as Johns Hopkins University are pursuing psilocybin’s potential for treating addiction, obsessive-compulsive disorder, PTSD and other mental-health conditions.
Notably, these institutions are relying almost entirely on philanthropic funding rather than federal research grants.
After successful voter-led campaigns, psilocybin became legally available in Oregon in 2023 as part of licensed, regulated therapy sessions, and they will be available in Colorado starting in 2025.
It’s an important distinction that states have legalized psychedelic therapy sessions and not products for consumers to take home and use unsupervised.
Legalization by 2034
Though law enforcement is turning a semi-blind eye to mushroom sales in Oakland, California Gov. Gavin Newsom last fall vetoed a bill that would have legalized psychedelics possession and personal use.
In an analysis of state-level reform progress published in late 2022 in JAMA Psychiatry, researchers predicted “a majority of states will legalize psychedelics by 2034 to 2037.”
That’s a solid decade or more behind marijuana, which has been legalized in some form in 40 states as well as Washington DC.
As for the “future of psychedelics in the United States,” the researchers added that it “hinges upon several factors: the outcome and FDA decision on ongoing clinical trials, the potential decisions by the (U.S. Drug Enforcement Administration) or governing bodies to change the classification of psychedelics and legislative reform at the state level, which has been the primary driver of cannabis legalization.”
It’s considered unlikely that the DEA will initiate drug decriminalization without influence from the White House or Congress.
As for the FDA, which is under the Department of Health and Human Services, that agency’s recommendation to move marijuana to Schedule 3 was based in large part on data from state-regulated MJ programs as well as published research.
That indicates states need to craft psychedelics legalization in a way that will provide the same trail of breadcrumbs for federal reform to follow.
And so far, they’re not.
While patients and therapists are excited about the potential of psychedelics therapy, there simply isn’t the same demand for psychedelics as there is for cannabis, where the regulated market generates billions of dollars and the FDA’s rescheduling recommendation was informed by data.
“Cannabis is regulated as a retail consumer product, while psychedelics are following a path of in-person therapeutic facilitation,” Livingston said.
“These differences are important when we consider how data from state-level programs is used to support rescheduling.”
“Years of state-level medical cannabis regulation demonstrated ‘currently accepted medical use’ as thousands of health care practitioners were licensed to recommend the drug to hundreds of thousands of patients,” Livingston continued.
“To generate similar data for psychedelics, we must consider policies that ensure these programs will be economically functional while empowering participation from healthcare practitioners and patients.”
More information about The Emerald Conference is available here.
Chris Roberts can be reached at chris.roberts@mjbizdaily.com.
Story from – MJ Biz Daily
Federal government grants B.C.’s request to recriminalize hard drugs in public spaces
Spencer Van Dyk – CTV News Parliamentary Bureau Writer
The federal government is granting British Columbia’s request to recriminalize hard drugs in public spaces, nearly two weeks after the province asked to end its pilot project early over concerns of public drug use.
Mental Health and Addictions Minister Ya’ara Saks made the announcement Tuesday on Parliament Hill.
“We have said yes, and it is effective immediately,” Saks told reporters.
B.C. is little more than a year into a three-year pilot project to decriminalize the possession of a small amount of certain illicit drugs, including heroin and cocaine.
But citing safety concerns from public consumption of those drugs, the B.C. government asked the federal government on April 26 to make illicit drug use illegal in all public spaces, including in hospitals, on transit and in parks.
Saks said the issue is a “health crisis, not a criminal one,” but that “communities need to be safe.”
According to a statement from Saks’ office, exemptions in the Criminal Code for possession of small amounts of illicit drugs for personal use will still apply in private residences, certain health-care clinics, places where people are lawfully sheltering, and overdose prevention and drug checking sites.
B.C. Mental Health and Addictions Minister Jennifer Whiteside said at a press conference Tuesday those exemptions will give people using at home the ability to “call for help without fear of being arrested.”
“The vast majority of people who die from toxic drug poisoning are dying at home alone,” she said.
“The intention of decriminalization was never about providing space for unfettered public drug use. That was not the intention. The intention was to ensure that people felt that people should not be afraid to reach out for help wherever they were using.”
When asked by reporters why the federal government took more than a week and a half to make the decision to abandon the pilot program, Saks said it is “the illegal toxic drug supply,” and not decriminalization, that is causing overdose deaths.
“Moving forward to any kind of pilot like the one in B.C., we know that we have to have a balance, public safety and public health,” she said. “That means there needs to be sufficient health services in place, scaled out to meet people where they’re at, and also law enforcement to have the tools that they need to ensure that public safety is a priority.”
The issue sparked tense debate in the House of Commons last week, when Conservative Leader Pierre Poilievre pressed the Liberals to accept B.C.’s request. One fierce exchange saw Poilievre ejected after calling Prime Minister Justin Trudeau “wacko” for his drug decriminalization policy.
Poilievre and Trudeau were back on the topic Tuesday following Saks’ press conference, with the Conservative leader pressing the prime minister over whether he will “try to impose the same radical and extremist policy” in other jurisdictions, paving the way for people to legally
“smoke crack in children’s soccer fields.”
“Obviously no one in this House does,” Trudeau responded.
“That is why we agreed with the British Columbia government to modify their pilot project to better suit their concerns,” he added, before accusing Poilievre of politicizing the issue.
Story from – CTV News
What psychedelics legalisation and decriminalisation looks like around the world
Psychedelics see increased legalisation and decriminalisation globally as treatment usages expand.
Research continues to progress on the potential mental and physical health benefits of psychedelics used in a therapeutic context. Yet psychedelic substances remain illegal around much of the globe, with notable exceptions.
As of 2024, some psychedelics have been given a legal or decriminalised foothold in: parts of Central Africa (Equatorial Guinea, Cameroon and Republic of the Congo), South Africa, Australia, the Bahamas, Brazil, the British Virgin Islands, Canada, the Czech Republic, Costa Rica, Israel, Jamaica, Mexico, Nepal, the Netherlands, Panama, Peru, Portugal, Samoa, Spain, Switzerland and the United States.
Psychedelics include psilocybin (which can be found in “magic mushroom”), MDMA (“ecstasy” or “molly”), LSD (“acid”) ayahuasca, peyote and ibogaine among others. The legal landscape of these substances is changing globally amidst continuous emerging research on the various benefits of their therapeutic use. Psychedelics have been shown to help with mental health conditions, such as treatment-resistant depression and post-traumatic stress disorder (PTSD). They’re also being studied for the relief of physical health conditions, such as those related to chronic pain.
“Psychedelics are not only very effective at treating a wide range of indications that currently lack treatment options but are also proving, when used responsibly, very safe,” says Grace Blest-Hopely, a neuroscientist and psychedelic researcher affiliated with King’s College London, in the UK.
In some countries, various psychedelics have full legalisation. In other countries, certain psychedelics have been legalised only under specific contexts. And still in other areas, some psychedelics have been decriminalised. “Decriminalisation” can mean different things; generally it implies that people can possess or use a personal amount of the substance despite it being illegal, although sometimes minor fines apply.
“It literally means that they’re not going to put resources behind arresting and prosecuting people,” says Mason Marks, a visiting professor at Harvard Law School and the senior fellow and lead of the school’s Project on Psychedelics Law and Regulation.
Marks says that criminalisation of drugs, including psychedelics, creates more harm than good.
“What happens when you criminalise something is that people don’t want to talk about it with their doctors,” he says. “People can’t talk amongst themselves. It’s quite plausible that when something is criminalised, people might hesitate to call for emergency medical services.”
Blest-Hopely agrees. “I believe that legalisation of all drugs”, she says, “allows for the removal of criminal activity from the supply chain and adults to make decisions on what they put in their bodies. That is also true for attaining products that are assured for quality.”
But she adds a note of caution. “Psychedelics are extremely powerful substances,” she says. “Any change in legislation towards better access, I would welcome greatly. However, it must come with education around psychedelics in their totality. Not just the positives, but also the risks, the effects and the enormity of impact that using large doses of substance can have, acutely and long term.”
Arguments against legalisation and decriminalisation include concerns over any potential increase in substance use disorders. However, psychedelics are currently being studied as a potential treatment for substance use disorders and are not considered addicting themselves. Other concerns include potential increases in psychedelic-related emergencies, such as emergency department visits for “bad trips.” However, emergency department visits tend to be rare for LSD and psilocybin, though more common for MDMA.
Here’s a closer look at the status of psychedelics around the globe, including the ever-changing landscapes of legalisation, decriminalisation and drug review agency approvals.
Are psychedelics legal in the United Kingdom?
“Psychedelic substances are still very much controlled in the UK,” says Blest-Hopely, who is also the founder of Hystelica, a UK-based community of researchers aimed at investigating psychedelics and their effects on female biology.
“Psychedelics like LSD and psilocybin are both still Schedule 1, defined as having ‘no therapeutic benefit’ and requiring a licence from the home office (government), plus considerable security and cost implications to conduct research,” she says.
Advocacy groups are pushing for change in the UK. “There have been movements within government lobbying groups to allow access to psilocybin for therapeutic relief in end-of-life cancer patients and military veterans,” Blest-Hopely adds. “Sadly, all discussions brought to the [parliamentary] chamber and the government have been swiftly done away with, stating no plans of the government to review or change the status.”
Central Africa: Gabon, Equatorial Guinea, Cameroon and Republic of Congo
Ibogaine, which is being studied for opioid use disorder and PTSD, comes from the sacred iboga plant, native to Central Africa, where it is used by Indigenous communities for ceremonial purposes in Gabon, Equatorial Guinea, Cameroon and Republic of the Congo. In these areas, ibogaine generally lacks a legal framework regulating it. It is, however, legal in Gabon, where it is protected.
South Africa
In South Africa, ibogaine is considered a medication and can be provided by licensed professionals.
Australia
In 2023, Australia’s Therapeutic Goods Administration (TGA), the agency responsible for regulating medicines, decided to allow authorised psychiatrists to prescribe some psychedelics for certain mental health conditions. The TGA permits the prescribing of MDMA for PTSD and psilocybin for treatment-resistant depression. Ibogaine can also be prescribed to treat addiction in Australia.
“The decision acknowledges the current lack of options for patients with specific treatment-resistant mental illnesses,” the TGA wrote in a press release.
The Bahamas
Psilocybin is legal to possess and use, but not to sell, in the Bahamas.
The British Virgin Islands
Psilocybin is also legal to possess and use, but not to sell, in the British Virgin Islands.
Peru
Ayahuasca is also legal in Peru, which in 2008, designated the psychedelic a part of Indigenous heritage.
Mexico
In Mexico, psychedelics are generally considered illegal. However, there is an exception that has made the country a hotspot for psychedelic retreats: Article 195 bis of the Federal Penal Code states that people cannot be prosecuted for spiritual or ceremonial use of psilocybin or 5-MeO-DMT. The latter is secreted by a gland in the Sonoran Desert toad and is also found in some plants. Ibogaine is unregulated in Mexico, making the country a place where people seek treatment. Peyote is legal in Mexico only for Indigenous ceremonies and traditions.
Costa Rica
Though not legal, personal drug use is not prosecuted in Costa Rica. And ibogaine is unregulated in Panama.
Psychedelics in the European Union
The European Union classifies psychedelics as Schedule I, meaning they are highly controlled and illegal except for “scientific or limited medical purposes.” The European Medicines Agency, the agency’s Central Nervous System Working Party and representatives from the European College of Neuropsychopharmacology recently issued commentary in the journal Lancet.
The authors acknowledge that mental health issues affect one in six people in the EU. “There is a need for effective, safe new treatments for mental disorders,” the commentary says. “In the past decade there has been a renewed interest worldwide in psychedelics as potential treatments for various mental health conditions.”
The Czech Republic
Despite the illegality of psychedelics across the EU, some countries within Europe have moved to either legalise or decriminalise certain substances. The Czech Republic, for example, decriminalised personal possession of small amounts of psilocybin, MDMA, LSD and peyote.
The Netherlands
In The Netherlands, psilocybin truffles are legal, though other forms of the compound are not. And ibogaine is unregulated in the country. Other psychedelics remain illegal.
Germany
In Germany, ibogaine is unregulated, except for pharmaceutical rules under the German Medicinal Products Act. The country has several ibogaine treatment centres.
Portugal
Portugal, at the start of the 21st century, decriminalised the personal possession and use of all drugs. Spain has also decriminalised drug use.
Switzerland
Switzerland has decriminalised substance use in general. The psychedelic LSD was accidentally synthesised in the country by chemist Albert Hoffman. Switzerland now allows for restricted compassionate use in a medical context of LSD and some other psychedelics. The Federal Office of Public Health must grant permits for such use. The agency says roughly 70 physicians have permits.
Switzerland has had the exceptional use program in place off and on since the 1980s, Calder adds, and the most recent law has been in effect since 2014. “This makes them the first country in the modern era to have legal psychedelic therapy, albeit only on official request,” she says. “I doubt there are any plans to legalise psychedelic therapy more broadly until there is more research on safety and efficacy.”
Israel, in 2019, approved a compassionate use programme for the therapeutic use of MDMA in people with PTSD and for several other patients.
Jamaica
Jamaica is a popular place for psychedelic tourism, thanks to its lack of a law surrounding psilocybin. Magic mushrooms have never been illegal in the country.
Nepal
In Nepal, psychedelics such as psilocybin are not explicitly mentioned in the country’s Narcotic Drugs (Control) Act 2033. The UC Berkeley Center for Psychedelic Sciences reports that psilocybin is legal in the country.
Canada
Canada and the US have been slowly expanding access to psychedelic substances. In Canada, most psychedelics are illegal based on their classifications under the Controlled Drugs and Substances Act, with a few exceptions.
The psychedelic compound 5-MeO-DMT is legal for personal use and possession in Canada. And although mescaline is listed as a Schedule III controlled substance, peyote is not. Mescaline is extracted from peyote. In 2022 Health Canada, the government’s department responsible for health policy, added a special amendment to its Special Access Program (SAP). The amendment allows physicians to request access to psilocybin, MDMA, DMT, LSD and other psychedelics.
“The SAP is only available for certain serious medical conditions, is meant for emergency basis only, and patients cannot possess [the substance] but must be administered it by the doctor or psychotherapist. It is not meant for long-term access,” says Harrison Jordan, the founder of Substance Law, a firm focusing on regulatory compliance regarding psychedelics and other controlled substances.
Health Canada added ibogaine to its Prescription Drug List in 2017, but the agency does not recognize its medical use. Therefore SAP requests are unlikely to be granted.
The Canadian province of British Columbia has decriminalised small amounts of illicit drugs. And Alberta, in early 2023, implemented a framework for regulating and licensing some health care providers to administer some psychedelics for mental health treatment.
The United States
In the US, psychedelics are considered illegal under the Controlled Substances Act. However, Native American ceremonial use of peyote is protected under federal regulation and in at least 28 states.
The Food and Drug Administration (FDA), however, granted breakthrough therapy designation for MDMA for PTSD in 2017. In 2018, the agency first granted the same designation for psilocybin for treatment-resistant depression. These designations helped allow psychedelic research to progress.
In 2024, the FDA is considering MDMA for therapeutic use in conjunction with psychological intervention in people with PTSD, now that the agency has accepted an application from Lykos Therapeutics. In addition to small changes at the federal level, some states and cities have moved to legalise psychedelics for medical purposes or decriminalise them for personal use.
The state of Oregon decriminalised most drugs in 2020 via Measure 110. However, the governor is set to sign a bill to recriminalise. Republican opposition to Measure 110 grew after a spike in fatal opioid overdoses. Research published in 2023 found that Measure 110 was not associated with the increase in the short term. But longer-term research is needed.
A group of business and political leaders in the state called for a ballot measure to repeal or alter the law, and many Democrats who were once in favour of Measure 110 changed their position. Opponents of recriminalisation note that Measure 110 was supposed to direct cannabis tax revenue towards addiction services. However, the pandemic hindered the process. If the governor signs the new bill, the state’s legalisation of psilocybin use at licenced psilocybin service centres will remain in effect.
A growing list of cities across the US have also made changes to their laws surrounding psychedelics. “Decriminalisation has been a very popular approach at the local level,” Marks says. “There are about two dozen cities across the country that have decriminalised to one extent or another.”
The list includes Washington, DC, which in 2020, decriminalised the personal use of psilocybin. “So far it’s only successfully been done through a ballot initiative by voters,” Marks adds.
In one exception, the California state legislature passed a bill to decriminalise the personal use and possession of psychedelics. “But the executive branch said no,” Marks says.
Samoa
In the region of Oceania, psilocybin is legal in Samoa.
New Zealand
Ibogaine can be legally prescribed in New Zealand.
Story from – BBC.com
With Germany legalising cannabis, Europe is reaching a tipping point. Britain, take note.
Regulating cannabis use is no longer radical but an increasingly normalised strategy. The ‘tough on drugs’ approach is archaic
The Guardian – Steve Rolles – March 29, 2024
Germany’s cannabis reforms were approved this week, overcoming the final legislative hurdle when the Bundesrat, Germany’s upper house, voted through the bill that passed with a huge majority in the Bundestag (lower house) last month. Germany is a significant addition to the growing list of countries defecting from the drug war consensus that had held for more than half a century. More than half a billion people now live in jurisdictions establishing legal adult access to cannabis for recreational use.
When Germany’s new law comes into force on 1 April, it will decriminalise possession of up to 25g of cannabis for personal use (and up to 50g in the home), allow requests to remove criminal records for past possession offences, legalise home growing of up to three cannabis plants for personal use, and establish a regulatory framework for not-for-profit associations within which cannabis can be grown and supplied to members.
Instead, Germany has opted for a form of “legalisation-lite” that provides channels for legal access via home growing or not-for-profit associations while, it hopes, avoiding the minefield of international law that a commercial market would have led to. A similar retrenchment has occurred with reforms in the Czech Republic and Luxembourg. All three countries have moderated their plans and essentially copied Malta, Europe’s unlikely cannabis reform pioneer, whose groundbreaking non-commercial home-grow and cannabis association model passed in 2021, becoming the blueprint for the new wave of EU reforms.
But as the debate about the merits of different cannabis policy models plays out in a globe-spanning natural experiment, from 24 US states, Canada and Uruguay to South Africa, Mexico and parts of Australia, Germany’s move feels particularly consequential. More than 100 times the population of Malta or Luxembourg, and sitting at the heart of the European establishment, Germany has the economic and political influence to significantly reorient laws and thinking about drug policy in the EU and the wider international stage.
This influence is inevitably being felt in the UK as well. As longstanding arguments for reform move from theory into reality in respected neighbour states, they become harder to ignore and increasingly permeate the national consciousness. Why continue to waste billions on failed enforcement when we could generate billions in tax revenue like Colorado? Why drive 100% of cannabis users towards organised crime groups and street dealers, when about 70% of cannabis users in Canada buy their cannabis from licensed stores? Why should people have to buy dodgy street cannabis of unknown potency, when they can join a legal association and buy quality controlled products with mandated information on contents and risks, as in Malta or Germany? Why maintain policies that disproportionately criminalise Black people and overload our creaking criminal justice system, when we could redirect enforcement spending and tax revenue into community programmes benefiting those most affected by the “war on drugs”, as they do in New Jersey or Massachusetts?
Endorsement of responsible cannabis regulation is increasingly normalised and mainstream. It is no longer a radical position but a pragmatic one, with real-world examples to prove it. And while Labour and the Tories, with an election looming, lack the courage to move beyond tired “tough on drugs” posturing, public backing for legalisation continues its inexorable rise, with polling now indicating majority support. As support for a reform platform becomes a political asset rather than a political liability, positions long held in private by those in power will increasingly emerge in public.
With London’s support for cannabis legalisation topping 60%, for example, its mayor, Sadiq Khan, has started openly exploring reforms. In the absence of principled political leadership from the government, change may boil down to this cold political calculus. We are fast approaching the tipping point and Germany’s reforms can only add to the momentum.
Steve Rolles is the senior policy analyst for Transform Drug Policy Foundation.
Story from – The Guardian
Most medical cannabis users aren’t going the prescription route, raising safety concerns: Manitoba-led study
More than half of Canadians who use medical cannabis don’t have authorization from doctor
Toronto wants to expand drug decriminalization to cover all ages and substances
Updated request asks Ottawa to go further than exemption recently granted to B.C.
Jordan Omstead– The Canadian Press –
Toronto updated its 14-month-old decriminalization request to the federal government Friday, clarifying it wants a Health Canada exemption to cover young people as well as adults, and all drugs for personal use.
The city’s submission, an update to its initial January 2022 request, indicates Toronto wants the federal agency to go further than the exemption it recently granted to British Columbia under the Controlled Drugs and Substances Act.
It makes clear the city wants its exemption to apply to all drugs for personal use and shield young people from criminalization, a departure from the B.C. exemption, which only applies to adults and lists a select number of substances.
Medical Officer of Health Dr. Eileen de Villa says the submission sent to Health Canada, co-signed by the city’s police chief and city manager, is a “made-in-Toronto” model reflective of a months-long consultation process.
“We’re talking about a matter of health and a matter of human rights, not one that really is meant to be addressed or is best addressed with a criminal justice approach,” she said in an interview. “That’s why we’re pursuing this route.”
B.C.’s three-year exemption under the Act was granted in June and came into force Jan. 31. While that exemption caps possession at 2.5 grams, the Toronto submission does not outline a specific threshold for what constitutes personal use.
Pace of approval process has garnered criticism
Drug use and purchasing patterns are “exceptionally diverse,” the submission said, and can vary based in part on a person’s tolerance. All trafficking and drug production would remain illegal.
Whereas the B.C. exemption only applies to people 18 and older, the Toronto model would also apply to young people. A 2019 survey conducted by the Canadian Association of Mental Health indicated around 11 per cent of Ontario students in Grades 7 to 12 reported the nonmedical use of opioids in the past year.
Eight people aged 12 to 17 died from opioid overdoses in Toronto between 2019 to 2021, the submission said.
“Health issues are health issues regardless of the person involved,” said de Villa.
“That’s why we feel that this is something that does have to apply to all so that we’re sure that even the youngest members of our community are having their health issues looked at and addressed through a health lens rather than through something like a criminal justice lens.”
The pace of the approval process has garnered criticism from drug users and advocates who say it fails to match the urgency required of an overdose crisis that has kills hundreds of people every year in Toronto.
“They’re moving way too slowly. So, it’s nice to see movement. It’s just whenever you see a little bit of movement, I think, for me at least, it hits home just how slowly this process is going — how much we’re dragging our feet,” said Dan Werb, director of The Centre on Drug Policy Evaluation at St. Michael’s Hospital.
Decriminalization will not make the street supply any less toxic, Werb says, but it could reduce the barriers people face to accessing services that help prevent them from dying of overdoses.
Policy only works if it covers all drugs: advocate
He says a decriminalization policy only works if it covers all drugs, since the street supply is often cut with substances not covered by B.C.’s exemption.
“But if we all agree that the primary driver of overdose death in Canada is the unregulated toxic market and all the contaminants that are circulating within it, then it seems to me that the most rational choice would be to engage, directly, intervene on that unregulated market,” Werb said.
Health Canada did not immediately respond to a request for comment Friday.
Better access to services, including 24-7 harm reduction and substance use supports will be “part and parcel” of making the model successful, said de Villa, the medical officer of health. She said there is “no question” that more services are needed.
The submission says the city intends to have several new services in place by the time decriminalization is implemented, including at least one 24-7 support location in the downtown core, to serve as an alternative to emergency departments.
Story from – CBC
Germany announces plan to legalise cannabis for recreational use
Minister says legalisation could set precedent for rest of Europe, though plan is still subject to EU approval
Philip Oltermann in Berlin – Wednesday 26 Oct 2022
“If this law comes to pass, it would be the most liberal project to legalise cannabis in Europe, but also the most regulated market”, the Karl Lauterbach said at a press conference in Berlin on Wednesday. “It could be a model for Europe.”
The overriding goal of making it legal to buy and smoke cannabis in Germany, the Social Democrat politician said, was to better protect young people, who were already consuming the drug in increasing numbers after obtaining it on the black market.
“We don’t want to expand cannabis consumption but to improve the protection of youth and health,” Lauterbach said. With about 4 million people in Germany having tried cannabis at least once over the last 12 months, he added, the current prohibitive model “isn’t working”.
Chancellor Olaf Scholz’s three-party coalition announced its intention to legalise cannabis for recreational use when it took office at the end of the year, but progress on a law has been slowed down by fears that such a step could contravene EU law and international treaties.
In the hope of minimising the risk of a cannabis law being challenged by European courts at a later stage, Germany is planning to submit an outline of its plans to the European Commission this week and seek an opinion.
If the commission made it unequivocally clear that the German model was not compatible with EU law, Lauterbach said, the government would not try to proceed to legalise cannabis on that basis. If Brussels gave it the green light, he said, a draft law would be presented in the first quarter of 2023.
The outline of the plans foresees it becoming legal to purchase and possess a maximum amount of 20g to 30g of cannabis for recreational use, and to consume it in private or in public. Privately growing up to three plants would also become legal.
Lauterbach said a legalisation of cannabis edibles, such as gums or baked goods, was still being looked into but was unlikely, as was the introduction of a general upper limit on the content of THC, the main psychedelic constituent of cannabis. An upper THC limit for 18- to 23-year-olds, however, is considered likely.
Advertising cannabis products would be banned. “A general ban on advertising recreational cannabis applies,” the outline document says. “Recreational cannabis is sold with (neutral) outer packaging without advertising design.”
The sale of cannabis products would likely take place in licensed establishments such as pharmacies, though the association of German pharmacists has spoken out against legalising the drug, warning this week it could be forced into competition with other commercial providers.
Lauterbach said the German path to legalising cannabis ran counter to that of the Netherlands, which technically still criminalises the growth and sale of the drug.
The Dutch model, Germany’s health minister said, had “combined two disadvantages: liberal use but not a controlled market”. “What we have learned from the Dutch experience is that we don’t want to do it that way”, he added. “We want to control the entire market.”
The normalisation of far right rhetoric has gone far enough. For decades, Guardian journalism has challenged populists like this, and the divisions that they sow. Fiercely independent, we are able to confront without holding back because of the interests of shareholders or a billionaire owner. Our journalism is always free from commercial or political influence. Reporting like this is vital for democracy, for fairness and to demand better from the powerful.
And we provide all this for free, for everyone to read. We do this because we believe in information equality. Greater numbers of people can keep track of the events shaping our world, understand their impact on people and communities, and become inspired to take meaningful action. Millions can benefit from open access to quality, truthful news, regardless of their ability to pay for it.
Whether you give a little or a lot, your funding will power our reporting for the years to come.
Article from – The Guardian
In move toward decriminalization, Biden pardons thousands for ‘simple possession’ of marijuana
WASHINGTON –U.S. President Joe Biden is pardoning thousands of Americans convicted of “simple possession” of marijuana under federal law, as his administration takes a dramatic step toward decriminalizing the drug and addressing charging practices that disproportionately impact people of colour.
Biden’s move also covers thousands convicted of the crime in the District of Columbia. He is also calling on governors to issue similar pardons for those convicted of state marijuana offenses, which reflect the vast majority of marijuana possession cases.
Biden, in a statement, said the move reflects his position that “no one should be in jail just for using or possessing marijuana.”
According to the White House, no one is currently in federal prison solely for “simple possession” of the drug, but the pardon could help thousands overcome obstacles to renting a home or finding a job.
“There are thousands of people who have prior Federal convictions for marijuana possession, who may be denied employment, housing, or educational opportunities as a result,” he said. “My action will help relieve the collateral consequences arising from these convictions.”
The pardon does not cover convictions for possession of other drugs, or for charges relating to producing or possessing marijuana with an intent to distribute. Biden is also not pardoning non-citizens who were in the U.S. without legal status at the time of their arrest.
The announcement marks Biden’s reckoning with the impact of 1994 crime legislation, which he supported, that increased arrest and incarceration rates for drug crimes, particularly for Black and Latino people.
The Department of Justice is working to devise a process for those covered by Biden’s pardon to receive a certificate of pardon, which they can show to potential employers and others as needed.
“The Justice Department will expeditiously administer the President’s proclamation, which pardons individuals who engaged in simple possession of marijuana, restoring political, civil, and other rights to those convicted of that offense,” the department said in a statement. “In coming days, the Office of the Pardon Attorney will begin implementing a process to provide impacted individuals with certificates of pardon.”
Biden is also directing the secretary of Health and Human Services and the U.S. attorney general to review how marijuana is scheduled under federal law. Rescheduling the drug would reduce or potentially eliminate criminal penalties for possession. Marijuana is currently classified as a Schedule I drug, alongside heroin and LSD, but ahead of fentanyl and methamphetamine. The White House did not set a timeline for the review.
But Biden said he believes that as the federal government and many states ease marijuana laws, they should maintain limitations on trafficking, marketing and underage sales.
Advocacy groups praised Biden’s announcement, with Kassandra Frederique, the executive director of the Drug Policy Alliance, saying the organization was “thrilled.”
“This is incredibly long overdue,” said Frederique. “There is no reason that people should be saddled with a criminal record — preventing them from obtaining employment, housing, and countless other opportunities — for something that is already legal in 19 states and D.C. and decriminalized in 31 states.”
It remains to be seen whether governors follow Biden’s lead. Erik Altieri, executive director of the National Organization for the Reform of Marijuana Laws, said extending the action to states could help millions of Americans.
“Since 1965, nearly 29 million Americans have been arrested for marijuana-related violations — for activities that the majority of voters no longer believe ought to be a crime,” he said.
Chris Goldstein, 46, was arrested after smoking half a joint during a marijuana legalization protest at Independence Hall in Philadelphia in 2013. He paid a $3,000 fine and spent two years on probation.
“As someone who voted for President Biden, I’ve been expecting this from the first day he came into office,” Goldstein said. “This was a campaign promise.”
As a writer and activist who has been public about his conviction, he’s not sure that his criminal record was an obstacle to him getting a job, but he knows that it shows up in his background checks. And he’s shied away from visiting other countries because convictions can complicate international travel.
“I’m thrilled, and everyone like me is going to be just as thrilled,” he said.
Rev. Al Sharpton, the president of the National Action Network, said Biden’s “righteous action today will give countless Americans their lives back.” But he added, “The United States will never justly legalize marijuana until it reckons with the outdated policies that equated thousands of young Black men with hardened drug pushers.”
The move also fulfills one of the top priorities of the Democratic nominee in one of their party’s most critical Senate races, as Pennsylvania Lt. Gov. John Fetterman has repeatedly pressed Biden to take the step, including last month when they met in Pittsburgh.
Fetterman, in a statement, took credit for elevating the issue on Biden’s agenda and praised the decision, calling it “a massive step towards justice.”
“This action from President Biden is exactly what this work should be about: improving people’s lives. I commend the president for taking this significant, necessary, and just step to right a wrong and better the lives of millions of Americans,” he said.
AP writer Colleen Long contributed.
Story from CTV News
Canada’s officials are facing a possible lawsuit over the right of dying patients to access psilocybin therapy.
Before “magic mushrooms” became synonymous with hippies and flower power, scientists used them for cutting-edge medical research and treatments. But, unfortunately, prohibition quickly drove common usage of mushrooms and other psychedelics to the fringes and all but cancelled all studies into these entheogens. Now, in stark contrast to this recent history, researchers worldwide are ramping up the testing of psilocybin as a treatment for some psychiatric conditions. Even the Australian government is on board, to the tune of $15 million in research funding.
Thanks to Canada’s activists, lawyers, lobbyists, researchers, and the media, the country seems to be at the forefront of psychedelic drug reform. However, there are still many several complex hurdles to overcome before Canadians have real access to psilocybin as a medicine.
The Fight for Medical Use of Psilocybin Is Moving to Canada’s Courts
Journalist, Curt Petrovich, wrote about the potential for a Canadian psilocybin medicine court case for The Tyee and spoke to several of the people involved in persuading Federal Health Minister Patty Hajdu to issue more exemptions under Section 56 of the Controlled Drugs and Substances Act, which gives the Minister discretion to issue such exemptions so that patients can legally access psilocybin for medical purposes.
The legal challenge is being marshalled by TheraPsil, the B.C.-based non-profit that last August helped a cancer patient secure the first exemption under Canada’s drug laws to use psilocybin for psychotherapy.
In a letter to Hajdu, TheraPsil’s lawyer says they intend to challenge the constitutionality of the Controlled Drugs and Substances Act’s provisions on psilocybin-containing mushrooms.
See TheraPsil’s Media Kit for more information.
Health Canada dragging feet on approving magic mushrooms for therapeutic use, patients and advocates say
Permission to use psychedelic drug in therapy stalls after brief wave of approvals
Curt Petrovich – CBC News – Jul 27, 2021
Nathan Kruljac was a young man of 25 when he experienced some shortness of breath while out for a drive in Surrey, B.C. He went to a walk-in clinic. Minutes later, he was taken to hospital. After a week of tests doctors had a diagnosis: follicular non-Hodgkins lymphoma. While treatment eventually put the cancer into remission, Kruljac says he never truly recovered.
Fifteen years later, he still suffers from trauma and PTSD.
“I still see [the cancer] as a time bomb rather than a success,” he said. “I’m scared and fearful of reoccurrence.”
Kruljac says conventional antidepressants and counselling only did so much to help. Now a husband and father, he feels he’s often failing his four-year-old daughter.
“I want to feel human again. I want to be able to look at my front door and not be terrified,” he said.
Last August, Kruljac got a sliver of hope when he read that Health Minister Patty Hajdu had granted a legal exemption to Saskatchewan cancer patient Thomas Hartle, allowing him to use psilocybin as an adjunct to psychotherapy.
It was the first of several dozen exemptions Hajdu would grant, to patients and even some therapists, for the psychedelic compound in what are commonly called magic mushrooms. Psilocybin was banned in Canada in 1974. It and the mushrooms which contain it remain illegal under the Controlled Drugs and Substances Act (CDSA).
But psilocybin is also, now, at the forefront of a renaissance in psychedelic therapy, due in part to persuasive research at institutions such as Johns Hopkins University and the University of California.
Some peer-reviewed studies have found that psilocybin has antidepressant effects and can allow patients, with the help of trained therapists, to confront fears and feelings that are otherwise too traumatic.
Patients granted an exemption typically take a one-time five-gram dose, enough to induce a full-on psychedelic experience, in tandem with planned therapy the day before, during and after the dose is taken.
Kruljac applied for an exemption in March, with help from TheraPsil, a B.C.-based non-profit group that convinced Hajdu to grant that first psilocybin exemption.
“What’s the worst that can happen?” he said. “It doesn’t work, and I’m back to square one.”
But more than four months later, Kruljac has heard nothing back from Hajdu or her department. Scores of other applications seem to have also gone into limbo.
Most of the previous exemptions were granted in a matter of weeks, with at least one approved in a couple of days, according to TheraPsil. Most of the 64 exemptions granted to date were issued last year. They went to 45 patients and 19 health professionals, according to Health Canada.
“What upsets me is that there are 50 other people in this country that have been given the exemption to choose their own path to healing. I am being treated differently which goes against our Charter of Rights and Freedoms,” he said. “And that’s what’s really upsetting me right now because there’s not only myself, but there are other people.”
One of them is Jim Doswell. The 67-year old from Victoria has survived colon cancer and T-cell lymphoma. But he lives with the after-effects of both that battle and some difficult years as a negotiator and a senior adviser to a federal deputy minister.
“I suffer from anxiety and depression and post-traumatic stress disorder,” Doswell said. “I have quite disabling anxiety.”
Two months ago, Doswell applied directly to Hajdu for an exemption to use psilocybin. He’s still waiting for a reply.
“With all due deference to the minister, I don’t need her for this,” Doswell said. “I can go down the street in Vancouver to [black-market] dispensaries and buy this product.”
But, Doswell says, without the minister’s permission, no therapist is likely to help him.
Even some who have an exemption feel as if they’re doing something wrong. In St. John’s, a teacher who was successful says the system for approving the exemptions is opaque and arbitrary, leaving him fearful to reveal his name.
“My biggest apprehension, I guess, is my career,” he confided, because the exemptions seem to be in a grey area — legal only under certain conditions, and because the minister says so.
“I would expect some potential repercussions,” he said.
Neither Hajdu nor spokespeople for Health Canada have been able to explain why the application approvals have stalled.
In a recent statement Health Canada said it is “committed to thoroughly reviewing each request for an exemption … on a case-by-case basis, taking into account all relevant considerations.”
Kruljac isn’t satisfied. On Monday, lawyers paid by TheraPsil served the government a notice of application, filed a federal court, seeking to compel an answer from Hajdu.
TheraPsil’s CEO Spencer Hawkswell says there’s a bigger issue at stake than one person’s ability to legally use psilocybin.
TheraPsil wants to see psilocybin and the mushrooms removed from the CDSA, and have it regulated much like medicinal cannabis was 20 years ago.
“We want to make sure that we’re doing justice to those who need access. Because, you know, you can always fight the government in courts. But that’s not what an effective government does. Effective government listens to people.”
Hajdu’s office didn’t respond to an interview request about TheraPsil’s legal manoeuvre. A spokesperson for Health Canada said it needed more time before commenting.
Story from CBC.ca
Biden Finally Grants Relief To People With Federal Marijuana And Drug Convictions After More Than A Year In Office
April 26, 2022 – By Kyle Jaeger
After more than a year in office, President Joe Biden on Tuesday granted clemency to dozens of people with non-violent federal drug convictions on their records.
The president commuted the sentences of 75 individuals who were previously released to home confinement amid the coronavirus pandemic. This marks the first clemency action from Biden—a move that advocates and lawmakers have long awaited and that the administration has repeatedly been pressed on.
While it’s not the mass pardon for people criminalized over cannabis that activists have been pushing for—with White House descriptions of only nine of the people newly receiving clemency mentioning marijuana—it’s a step toward fulfilling a campaign pledge that Biden repeatedly made while running for president.
“America is a nation of laws and second chances, redemption, and rehabilitation,” Biden said in a statement. “Elected officials on both sides of the aisle, faith leaders, civil rights advocates, and law enforcement leaders agree that our criminal justice system can and should reflect these core values that enable safer and stronger communities.”
The president said that many of the people he is granting relief to “would have received a lower sentence if they were charged with the same offense today, thanks to the bipartisan First Step Act” signed into law by his predecessor, President Donald Trump.
In addition to the 75 sentence commutations, Biden also issued three pardons.
Late last year, there were signals that the administration might be moving toward clemency for certain people with federal convictions. The federal Bureau of Prisons (BOP) started asking eligible individuals to get the process started by filing out clemency applications.
Now that preliminary step appears to be getting executive results.
The president continues to oppose adult-use marijuana legalization, despite increasing bipartisan support for the policy change, but it seems the White House is finally willing to take unilateral action to provide some level of relief for those caught up in the war on drugs that Biden as a senator helped perpetuate.
The commutations are generally being granted to people with low-level drug offenses with up to four years left in their sentence and who were eligible for home confinement under the Trump-era Coronavirus Aid, Relief, and Economic Security (CARES) Act.
About 8,300 federal inmates were allowed to temporarily transition to home confinement amid the coronavirus pandemic in 2020.
Biden has received about a dozen letters from lawmakers, advocates, celebrities and people impacted by criminalization to do something about the people who remain behind federal bars over cannabis. After months of inaction, some members of Congress like Sen. Elizabeth Warren (D-MA) have even sent follow-up letters demanding a response.
Among those pushing for reform is Weldon Angelos, a person who received a president pardon from Trump in 2020 and has since become a key advocate for criminal justice reform who has worked with both the Trump and Biden administration of furthering relief.
“We recently had an impactful meeting at the White House to discuss clemency matters, especially for those incarcerated for cannabis offenses, and also those out on CARES Act,” Angelos told Marijuana Moment. “The meeting was very encouraging, and we believe President Biden will keep his campaign pledge to grant categorical clemency for cannabis offenders.”
The advocate noted that Biden recently appointed someone with experience as a federal defender to serve as pardon attorney—a position usually held by a prosecutor or military judge—calling the move “a breath of fresh air.”
“I believe the president is moving in the right direction by putting the right people in these positions,” Angelos said. “Today was a large grant of clemencies, and to do this in his first term strongly suggests many more are coming.”
“We will continue urging the president to grant clemency to the 2,700 people incarcerated for cannabis only offenses, as he promised when he was running for president. And we are grateful for the opportunity to meet with the president’s team to share our ideas.”
Biden, in his statement, said that “while today’s announcement marks important progress, my Administration will continue to review clemency petitions and deliver reforms that advance equity and justice, provide second chances, and enhance the wellbeing and safety of all Americans.”
Along with the acts of clemency announced on Tuesday, the administration also announced a series of moves to expand opportunities for formerly incarcerated people, including job training, grants for workforce development programs, expanded access to capital, improved reentry services and support for health care, housing and education.
A report published by the Congressional Research Service (CRS) last year affirmed that the president has it within his power to grant mass pardons for cannabis offenses. It also said that the administration can move to federally legalize cannabis without waiting for lawmakers to act.
Despite having the authority to unilaterally issue a mass pardon for people with federal cannabis convictions, however, Biden had previously only ceremonially pardoned turkeys around Thanksgiving since taking office.
Following that ceremony, The New York Post’s Steven Nelson pressed the president on cannabis clemency, asking him if there were plans to pardon “any people in addition to turkeys.” Biden jokingly replied, “you need a pardon?” and didn’t respond to a follow-up question about marijuana prisoners.
The White House has been asked about the issue several times. But while Press Secretary Jen Psaki has said that the president has “every intention of using his clemency power” and is “looking at” relief for non-violent drug offenders, no meaningful action has been taken until this point.
Advocates may be encouraged to see this latest action, but they’re committed to getting the president on board with broader reform that they hope will be sent to his desk, including bills to end federal marijuana prohibition.
After the House passed a cannabis legalization bill earlier this month, Psaki told reporters that the president agrees that “our current marijuana laws are not working,” but she declined to directly address whether the president supports the specific legislation.
The press secretary, who is reportedly planning to leave the administration later this year, said that “we look forward to working with Congress to achieve our shared goals—and we’ll continue having discussions with them about this objective.”
Do those “shared goals” include the main components of the MORE Act to holistically end prohibition? Psaki didn’t get into detail. It’s another example of the marijuana policy schism that’s divided not just congressional lawmakers along partisan lines but also the Democratic president and a supermajority of voters in his party.
Biden himself hasn’t made a substantive public comment about cannabis policy since entering the Oval Office, beside making a quick, dismissive comment to the reporter who asked about clemency for current federal marijuana prisoners.
Vice President Kamala Harris, for her part, said last year that the Biden administration isn’t focused on following through on its marijuana reform pledges because it’s too overwhelmed with other issues.
Advocates have been losing patience. This latest action represents a concrete steps toward righting the wrongs of the drug war, but the administration has also made moves that subvert reform efforts.
For example, in Biden’s latest budget proposal for Fiscal Year 2023, he again proposed the continuation of a rider blocking Washington, D.C. from legalizing cannabis sales. To the relief of advocates, however, he again kept a separate rider intact to protect legal medical cannabis programs from federal intervention.
Early in 2021, the Biden administration came under fire after it was reported that it had terminated or otherwise punished dozens of staffers who admitted to prior marijuana use as part of their background check process.
Psaki previously attempted to minimize the fallout, without much success, and her office also stressed that nobody was fired for “marijuana usage from years ago,” nor has anyone been terminated “due to casual or infrequent use during the prior 12 months.” However, she’s consistently declined to speak to the extent to which staff have been suspended or placed in a remote work program because they were honest about their history with marijuana on the federal background check form.
For what it’s worth, a poll released in January found that more than half of Americans feel that Biden has made little to no progress on his campaign pledge to decriminalize marijuana during his first year in office—and most people also aren’t betting on him doing more to advance the reform in 2022.
Story from – Marijuana Moment
House Passes Bill to Decriminalize Marijuana
The legislation, which faces an uncertain outlook in the Senate, would also establish a process to expunge prior marijuana-related convictions.
By Kaia Hubbard – April 1, 2022
The House passed legislation on Friday to decriminalize marijuana at the federal level.
The Marijuana Opportunity Reinvestment and Expungement Act passed 220-204 in a vote largely along party lines and is only the latest in a series of efforts to decriminalize the substance after a version of the measure cleared the chamber in December 2020 but stalled in the then Republican-controlled Senate.
Democratic Rep. Jerrold Nadler of New York, who sponsored the bill, argued that the legislation is a key step toward correcting “injustices of the last 50 years.”
“The MORE Act is long-overdue legislation that would reverse decades of failed federal policies based on the criminalization of marijuana,” Nadler said. “It would also take steps to address the heavy toll these policies have taken across the country – particularly among communities of color. For far too long we have treated marijuana as a criminal justice problem instead of as a matter of personal choice and public health. Whatever one’s views are on the use of marijuana for recreational or medicinal use, the policy of arrest, prosecution and incarceration at the federal level has proven both unwise and unjust.”
But Republicans criticized the timing of the legislation, insinuating that Democratic priorities are askew amid crises overseas and at home.
Others argued that the legislation is incomplete. Republican Rep. Cliff Bentz of Oregon cited the situation in his home state, where marijuana has been legalized, arguing that its shortcomings shed light on how national legislation should address things like funding for law enforcement ahead of a nationwide decriminalization.
The House on Friday voted in favor of an amendment to provide the National Highway Traffic Safety Administration the resources to conduct a study on driving under the influence of marijuana and another to conduct a federal study to look at the impact of legalizing marijuana on the workplace. But the lawmakers narrowly voted down another amendment that would have established that the use of marijuana should not be among the reasons to deny or rescind a security clearance.
The movement to legalize marijuana has in recent years garnered strong public support. More than two-thirds of Americans support legalizing marijuana, according to a November 2021 Gallup poll, maintaining the record-high level reached in 2020.
At least 18 states already permit the recreational use of marijuana, while 37 states allow the substance’s use for medical purposes, according to the National Conference on State Legislatures.
At present, marijuana is listed as a Schedule I substance under the Controlled Substances Act, meaning that it has “a high potential for abuse, no currently accepted medical use in treatment in the United States, and a lack of accepted safety for use under medical supervision,” according to the Drug Enforcement Administration. Democratic Rep. Steve Cohen of Tennessee argued on Friday that keeping the substance within the classification among the likes of methamphetamines and heroin is “absurd.”
Thailand To Legalize Recreational Cannabis
In 2018, Thailand legalized medical marijuana and became the first Southeast Asian country to do so and is now close to legalizing recreational marijuana. The country’s Food and Drug Administration is inching closer to removing cannabis from its list of controlled drugs. If the Narcotics Control Board approves the proposal, it moves on for final approval from Health Minister Anutin Charnvirakul before it will be official.
If passed, the new ruling would remove the threat of lengthy prison sentences and significant fines for cannabis convictions.
Because the plant is categorized as a category-5 narcotic, anyone convicted of producing, exporting, or importing cannabis faces two to 15 years in prison and fines of up to 1.5 million baht (USD 45,000).
Those caught in possession could serve up to five years in jail and a maximum penalty of 100,000 baht (USD 3,000).
Once the plant is delisted, all of those punishments are eliminated.
Thailand has previously pursued a piecemeal approach to marijuana legalization. Parts with low psychoactive components, such as leaves and stems, were cut from the list in December 2020.
But many laws continued to maintain strict controls on the growing, harvesting, and processing of cannabis. While possession of marijuana has been illegal, businesses have had access to the plant. This latest proposal would decriminalize buds and flowers, both of which are rich in psychoactive THC.
Chaiwat Sowcharoensuk, an analyst at Krungsri Research, concedes that while all parts of cannabis could be bought, sold, and used, it’s likely that extracts with higher THC levels will continue to be tightly regulated.
“Producers of soaps, beauty products, and cosmetics from marijuana will likely be the ones to benefit the most from decriminalization,” said Chaiwat.
Withid Sariddeechaikool, deputy secretary-general of the FDA, envisions several economic benefits from legalizing marijuana.
“If we’re able to decriminalize marijuana, we will be able to benefit from all of the plant and not just parts of it,” said Withid. “The flower buds and seeds could be used economically and in compliance of the law.”
Anutin Charnvirakul, a deputy prime minister and the public health minister, has strongly supported legalizing cannabis.
During the 2019 general elections, he pledged to legalize cannabis and allow households to grow up to six plants. This promise helped the Bhumjaithai, a political party, secure 51 seats, making it a core member of the ruling coalition. As the next general elections approach, Anutin has been pressing to keep his pledge.
There is also the hope and expectation that legalizing cannabis will revitalize Thailand’s tourism industry, which struggled during the coronavirus pandemic.
In the U.S., tourism in Colorado and Washington rose after they legalized recreational marijuana and people could purchase cannabis supplies.
Internationally, Uruguay and Canada (the only sovereign states that allow both consumption and sale of cannabis) have seen an uptick in tourism.
The push to scrub cannabis from the country’s narcotics list comes after kratom, a Southeast Asia native plant whose leaves are used as a painkiller and mind stimulant, was decriminalized in 2020.
The more highly addictive drugs such as cocaine, heroin, and methamphetamine remain illegal in Thailand, with heavy punishments.
Story From – The Consumer
Canada Regulators Ease Access to Psychedelic Drugs
Canada health regulators announced that the government would allow physicians to request access to restricted drugs including psychedelics for their patients.
A.J. Herrington – January 6, 2022
Health Canada, the nation’s health department, said that drug regulations were being amended based on new research into the therapeutic benefits of psychedelics.
“There has been emerging scientific evidence supporting potential therapeutic uses for some restricted drugs, most notably psychedelic restricted drugs such as MDMA and psilocybin,” Health Canada noted in the Canada Gazette, an official government publication.
Under the amendment to federal food and drug regulations, physicians will be able to request access to restricted drugs on behalf of their patients through Health Canada’s Special Access Program. Previously, restricted drugs including psychedelics were not available through the program.
The Special Access Program permits health care professionals to request permission to use unapproved treatments for patients with serious or life-threatening medical conditions. The program applies only in cases where conventional therapies have failed, are unsuitable, or not available in Canada. Patients are not permitted to request access to treatment through the program on their own behalf.
Psychedelic Research Continues
Research into psychedelics including psilocybin, MDMA and ketamine has shown that the drugs have potential therapeutic benefits, particularly for serious mental health conditions such as depression, addiction and anxiety. A study published in the journal JAMA Psychiatry in 2020 found that psilocybin-assisted psychotherapy was a quick-acting and effective treatment for a group of 24 participants with major depressive disorder. Separate research published in 2016 determined that psilocybin treatment produced substantial and sustained decreases in depression and anxiety in patients with life-threatening cancer.
Before Wednesday’s announcement, patients could gain access to psychedelic drugs through two legal avenues. The first method would be to participate in a clinical trial, which only accepts patients on a limited basis and are not available nationwide. Patients could also gain access to restricted drugs by personally requesting a special exemption to regulations from Canada’s Health Minister.
Easing Access for Patients
Regulators noted in the announcement that “the regulatory amendments will not create large scale access to restricted drugs and they do not signal an intent towards the decriminalization or legalization of restricted drugs. The Special Access Program is for emergency treatment only.” But the move should make it easier for patients with an exceptional need to access psychedelic drugs.
Dr. John Huber, a clinical forensic psychologist and the CEO of Tripsitter Clinic, a publicly-traded ketamine therapy telemedicine provider that is listed on the Canadian Securities Exchange, applauded the Canadian government for continuing to advance and acknowledge the benefits of psychedelic therapy.
“This breakthrough decision will expand access to MDMA and psilocybin therapy and help save the lives of those with life-threatening mental health conditions,” Huber wrote in an email to High Times. “We hope Canada’s success pushes the U.S. government to follow a similar pathway while awaiting FDA approval for MDMA and psilocybin.”
Greg Rovner, CEO of Heally, a telemedicine platform for psychedelic clinics and patients looking for alternative medicine treatment, said the decision by Canadian regulators to ease access to psychedelics should spur new research into the drugs.
“Health Canada’s recent decision is a ringing endorsement of MDMA and psilocybin’s therapeutic potential,” Rovner wrote in an email. “It recognizes the growing body of research into the benefits of psychedelics and expands access to psychedelics for patients in serious and life-threatening conditions. We hope to see more studies on the safety and efficacy of psychedelics that will spur further regulatory reform.”
Story from – High Times
Pharmaceutical-grade psychedelics are coming to your medicine cabinet
Abigail Klein Leichman – January 3rd 2022
“The world urgently needs a new way to treat mental health issues, and at PsyRx we believe psychedelics are a big part of the solution,” says Itay Hecht.
Hecht is CEO and co-founder of this Israeli company, which is developing standardized pharmaceutical-grade psychedelics from natural sources — not synthetics — as active pharmaceutical ingredients.
Using an agro-medical bioreactor invented at the Hebrew University Faculty of Agriculture, PsyRx produces psychedelic botanic extracts psilocybin (from “magic” mushrooms) and ibogaine (from the root bark of the iboga shrub).
Psilocybin has been shown to have positive effects in treating depression, anxiety and addiction, and has been suggested as a potential treatment for obesity, PTSD, cluster headaches and more.
Ibogaine has shown promise as an anti-addiction drug, among other indications. PsyRx is focusing on its potential to improve current SSRI (selective serotonin reuptake inhibitor) antidepressants.
“SSRIs have some very bad side effects on libido and appetite, and patients often stop using them. We believe adding a microdose of ibogaine will counter those effects and make a better drug,” Hecht says, emphasizing that microdoses of psychedelic substances do not cause hallucinations.
“We are starting small animal trials soon to check safety and efficacy. Hopefully, in a year’s time, we can start human trials” to test this ibogaine application, he tells ISRAEL21c.
ON-TREND
Adding psychedelics to mainstream drugs may seem a bit “out there,” but in fact it’s on-trend.
According to market intelligence report CB Insights, funding for psychedelic medicine companies is growing rapidly as traditional pharma giants see declines in return on investment for drug R&D and are interested in exploring alternative products. Consumer interest in hallucinogenic drugs also is growing, according to this report.
Synthetic versions of psychedelic substances are easier to manufacture uniformly according to industry standards, but they may not work as well as natural versions.
We believe there’s a big difference between biological and synthetic molecules, especially in how they interact with receptors in the brain,” says Hecht. “Synthetics are not as successful as a ‘key’ fitting into the ‘lock.’ But it is complicated to work with biological molecules.
That’s where the bioreactor comes in. This innovative machinery is what may enable PsyRx to transform the growing psychedelics market.
FROM CANNABIS TO PSILOCYBIN
Hecht started his career 20 years ago in The Netherlands, managing cannabis dispensaries and seed companies. He moved back to his native Israel in 2007 to study water and soil engineering to better understand the world of botanicals.
He then moved on to another cannabis enterprise, Stickit Labs. The president of Stickit, Asher Holzer, is a serial biotech entrepreneur whose successful ventures have included InspireMD, TheraCoat and UroGen. He was also part of the management team of Biosense, an Israeli company acquired by Johnson & Johnson in 1997.
“Two and a half years ago, we saw an opportunity in the psychedelic sector; there were no licensed companies in Israel,” says Hecht, so PsyRx became the first.
Holzer is PsyRx’s chairman and co-founder. CTO and co-founder Kobi Buxdorf is a microbiologist with a PhD from Hebrew University.
Buxdorf developed tissue-culture bioreactors for producing cannabis at a pharmaceutical standard and founded Cannadorf to commercialize this technique.
“He then developed a bioreactor for psilocybin and moved it forward to the commercial stage,” says Hecht.
There are not yet standards for the regulation of psilocybin, so we expect it will take at least a few months to receive GMP [good manufacturing practices] designation for the pharma industry,” he says. “Hopefully by the end of next year, we’ll have the ability to sell our psilocybin worldwide for clinical research and drug development.
PsyRx has about 10 employees and has raised “a couple of million dollars” from private investors. “We want to go public,” says Hecht. “We really believe in what we do.”
Story from – Zenger News – CBS Austin News
Civil society organizations release drug decriminalization platform for Canada
OTTAWA — Twenty-one organizations across the country have released Canada’s first civil society-led policy framework for drug decriminalization and redistributing resources from police to services that help communities most affected by the harms of policing.
The collaboration includes groups of people who use drugs, families affected by drug use, drug policy and human rights organizations, front-line service providers and researchers.
Their framework calls for funds that would flow to police to be invested instead in community-based organizations, services that promote harm reduction and address mental health issues, safe supply programs, and other forms of healing.
Donald MacPherson, executive director of the Canadian Drug Policy Coalition, one of the contributors to the platform, says the framework’s proposed policy shift would help change a “historically cruel” application of criminal law that has harmed Canadians.
This national call comes days after the federal government tabled Bill C-5, which would repeal mandatory minimum penalties for drug offences and some gun-related crimes, and would require police and prosecutors to consider alternative measures for cases of simple drug possession.
This report by The Canadian Press was first published Dec. 9, 2021.
‘Magic’ Mushrooms, Ecstasy and Other Psychedelics Could Become Legal in California
Mari Payton, Meredith Royster and Mike Dorfman – December 5, 2021
Coronado resident Marcus Capone has trouble talking about 13 years of deadly combat tours he experienced as a U.S. Navy SEAL.
It left scars, both physical and mental, and resulted in his medical retirement.
“It seemed like every time I got back from a deployment it would get worse. I was just numb and cold and hard,” Capone said. “I think that what affected me more was individuals that I served with, or I was really close with, that we lost in the war. Those were tough and are still tough.”
“I was keeping it all together through the many prescriptions I was being given by the doctor, psychologists, and whoever else I was seeing,” he admitted.
He was diagnosed with post-traumatic stress disorder. At times, he says he was suicidal.
“I didn’t care about anything… If I crash (my truck) ‘great’. Like, maybe I don’t wake up and all this goes away,” Capone said.
Capone’s wife, Amber, suggested he try psychedelic treatment outside the United States where it’s legal. At first, he was not on board. “The first reaction was, ‘This is nuts, this is crazy,’” he said.
But after doing his own research, he traveled to Mexico to try ibogaine. The drug is made from the root bark of a West African shrub and taking it causes intense hallucinations.
“You can’t hide from the medicine. It’s going to reach down and it’s going to pull out everything that is affecting you. Some of that is really uncomfortable when you are talking to your dead dad or talking to your dead buddy,” Capone recalled.
But almost immediately, he says he felt a huge weight had been lifted. After years of frustration and hopelessness, he says he got his life back.
“You felt like your brain was rebooted like a new operating system,” he said.
Marcus supports Senate Bill 519, introduced by State Sen. Scott Wiener, a Democrat from San Francisco. It would give veterans access to psychedelic therapies, but it also decriminalizes several drugs like LSD, ecstasy, mescaline, psilocybin “magic mushrooms” and more.
Anyone 21 years of age or older would be able to keep a certain amount of each, grow them, or give them away to another adult. The bill would allow for their use and research without criminality.
Other cities have already made changes. Denver became the first city to decriminalize psilocybin in May 2019. The California cities of Oakland and Santa Cruz followed.
SB-519 narrowly passed the State Senate and is now in the State Assembly. It could get changed along the way to the governor’s desk.
The 38th Senate District encompasses a large portion of San Diego County. Senator Brian Jones represents the 38th Senate District. He voted against SB519.
“The Senate Bill goes way too far as far as decriminalizing psychedelic drugs and making them completely legal on the street. I can’t support that,” he said.
But Jones says he does support the potential use of psychedelic treatment for military veterans.
“My dad is a veteran, my grandfather was a POW in World War II, he suffered PTSD. They didn’t call it that then, but he had issues his entire life. I know that we need to treat that and find solutions to that,” he said.
Joseph Schuermeyer is a San Diego psychiatrist. He is more skeptical of psychedelic treatments for therapeutic purposes.
“We are still a long way from approving these interventions. There are risks that could be very harmful and we have to assess those risks with those benefits,” he said.
Schuermeyer doesn’t support either side of the bill and says we’re nowhere close to making psychedelics a mainstream therapy. He says more data is needed, and just because many drugs are considered “natural” it doesn’t make them safe.
“There can be risks with anything we put in our body. Moderation is important and there are natural substances that are highly toxic. There is frequent neurotoxicity with certain substances and that can have complications for various parts of the brain.”
David Bronner, who lives in Encinitas, is the CEO of Dr. Bronner’s. Bronner says his company, founded by his grandfather, fights for and financially supports causes he believes in: regenerative agriculture, fair trade, animal advocacy, industrial hemp and drug policy reform.
NBC 7 Investigates discovered his company donated $452,500 to the New Approach Political Action Committee in California. “We look at money as energy, like we’re just stewards. We want to deploy it in where we see real leverage points to really move things along in society,” Bronner said.
Bronner and his company lobby not only for psychedelic legalization efforts but others like marijuana. “It’s life-saving medicine and we need to decriminalize it so people feel comfortable accessing the medicine.”
Bronner is also a board member of a group called MAPS — Multidisciplinary Association for Psychedelic Studies. Bronner says it’s his goal to legalize magic mushrooms and other psychedelics.
“It can just really help people get in there and just break self-destructive patterns of thought and behavior. We have veterans right now who are dying at the rate of 22 a day or taking their own lives,” explained Bronner.
Capone agrees. “Why should individuals who go overseas for war come back here and not get the help they are looking for and then have to go back overseas outside the borders to get treated?” he said.
After his own life-changing experience with ibogaine, Capone and his wife started an organization called VETS – Veterans Exploring Treatment Solutions – which has paid for hundreds of veterans to seek psychedelic treatments where it’s legal.
“What Senate Bill 519 will do is to allow access to these medicines right here,” Capone said. He believes there is no better evidence on the benefits of the treatment than his own life story.
“I feel like I am back and I love that,” he said with a big smile.
Story from – MSN.com
Toronto’s top doctor recommends decriminalizing possession of small amounts of drugs
MSN – November 28, 2021
Toronto’s medical officer of health wants to decriminalize possession of small amounts of illegal drugs in the city in an effort to combat the opioid overdose crisis — and she’s got support from the local police chief.
A report from Dr. Eileen de Villa to the city’s board of health recommends asking the federal government to permit simple possession of all drugs.
It is also asking the province to increase funding to help expand harm reduction services, increase overdose outreach beyond homeless shelters to parks and drop-ins, and deliver mobile drug consumption services outside of downtown.
“The current approach to the drug poisoning crisis is not working and we continue to see tragic outcomes that are preventable,” de Villa said in a statement.
“This is why we are aligned with other jurisdictions and recommending decriminalizing the possession of all drugs for personal use and connecting all people who use drugs with health and social supports.”
Toronto police Chief James Ramer said in a letter to de Villa that the force supports a new approach to drug criminalization.
“We agree that the current approach to managing drug use does not support safe communities or advance the health of people who use drugs,” Ramer wrote.
“Decriminalization of the simple possession of all drugs — combined with the scale-up of prevention, harm reduction, and treatment services — is a more effective way to address the public health and public safety harms associated with substance use.”
Ramer said a decriminalization model should also include a safe supply of drugs, something health-care workers have demanded for years.
De Villa is asking for an exemption to a section under the Controlled Drugs and Substances Act that would apply only to those living in the city.
She is recommending the city make the request by the end of the year.
Her report says there were 531 opioid toxicity deaths in 2020, which is an 81-per-cent increase from 2019.
The city, like the rest of the province, is in the midst of a worsening deadly opioid crisis, which has been exacerbated significantly during the pandemic.
Paramedics responded to 5,776 suspected opioid overdose calls over a one-year period between Nov. 1, 2020 to Oct. 31, 2021, a 61-per-cent increase in the same time frame the year before.
There have been 351 deaths, according to paramedic data in that time frame, up 53 per cent from the same period the year prior.
De Villa said the increase is due to multiple factors, including the “toxic nature of the unregulated drug supply, as well as pandemic-related service reductions and physical distancing requirements.”
Vancouver has made the same request to Health Canada, de Villa noted.
Ontario’s Big City Mayors have also urged the move in recent months.
Jeff Lehman, the mayor of Barrie, Ont., and the chair of the mayors group, said the province and the federal government have to treat the problem as a public health one, not a criminal matter.
“We’ve got a federal government that sounds like they’re interested,” Lehman said.
“It may be a little tougher to convince the Ontario government because I think so far they’ve had a little bit more of an enforcement and less of a public health approach. And we’re going to need to push there to get them to change that.”
He said they can’t really decriminalize drugs without also offering more treatment capacity.
“We could make the situation worse, so that’s where that’s where the province really comes in,” Lehman said.
He said the time has come to work on the opioid epidemic, especially given how familiar Ontarians have become with the importance of public health.
“We have another epidemic in a way, but it’s not spread by a virus,” Lehman said.
“It’s spread by drug use, but it’s an epidemic that’s taking almost as many lives and, just like COVID, we need to take a public health approach and maybe that’s why I hear more understanding and support for this approach generally.”
Neither the federal nor the provincial government responded immediately to a request for comment.
The city’s board of health is set to consider the report on Dec. 6.
This report by The Canadian Press was first published Nov. 29, 2021.
Liam Casey, The Canadian Press – MSN
Woman’s tumour shrank after taking CBD oil daily for more than two years: case study
Alexandra Mae Jones – CTVNews.ca writer – November 4, 202
TORONTO — A case study of a U.K. woman whose lung tumour shrunk without the aid of conventional treatments while she was taking a daily dose of cannabidiol (CBD) oil has scientists suggesting it may be worth studying the use of CBD oil further.
The report, published in BMJ Case Reports in October, describes how the woman’s tumour shrunk from 41 mm to 10 mm in roughly two and a half years.
Cannabinoids are similar to endocannabinoids, which are manufactured by the human body to help in various processes, such as nerve function, energy metabolism, pain and inflammation and immune function, among others.
While cannabinoids have been studied as a primary cancer treatment before, the results have been inconclusive and inconsistent, making it difficult to pinpoint if it actually had any impact.
In this case report, a woman in her 80s was diagnosed with “non-small cell” lung cancer in June 2018 after months of a suspicious cough. She was a life-long smoker, smoking roughly 68 packs a year, and had a background of “mild chronic obstructive pulmonary disease,” the report stated.
When she was first diagnosed, even though she was a candidate for treatments aimed at curing her cancer, she declined surgery, radiotherapy and other treatments she was offered.
The report offered the patients’ perspective, in which she explained that she declined treatment because she had watched her late husband go through the struggle of radiotherapy.
So doctors decided to simply perform regular CT scans to check up on the patient every three to six months.
During these scans over the next couple years, doctors observed that her lung cancer was shrinking. By February 2021, it had reduced by approximately 76 per cent in diameter, which averaged to a 2.4 per cent reduction per month since diagnosis.
In 2019, the shrinking of the tumour piqued doctors’ interests, and the patient was brought in to discuss her results.
In this meeting, she revealed that she had been taking CBD oil “as an alternative self-treatment for her lung cancer” since August 2018, which she had sourced from outside of the U.K. She was taking 0.5 ml of the CBD oil, two-three times per day.
“The supplier advised that the main active ingredients of the ‘CBD oil’ used by this patient were Δ9-tetrahydrocannabinol (THC) at 19.5 [per cent], CBD at 20.05 [per cent] and tetrahydrocannabinolic acid (THCA) at 23.8 [per cent],” the report stated.
She had noticed a reduced appetite since taking the CBD oil, but apart from that, she had no other changes to her prescribed medications, diet or lifestyle — she was even still smoking one pack of cigarettes a week still, despite being advised to quit.
The endocannabinoid system in humans, which was only identified in the 1990s, is still a mystery in many ways. Although we know it helps to regulate physiological and cognitive processes and manufactured endocannabinoids that “act as neuromodulators,” just how this system can be tapped into with medication and drugs is a growing research avenue.
Cannabis and cannabinoids in general do have proven therapeutic uses, such as assisting with chronic pain, anxiety and sleep disorders, but research into whether cannabinoids could be used as a direct cancer treatment has not yet come up with a clear answer.
If the CBD oil did play a part in the woman’s tumour shrinking, doctors aren’t sure how the active ingredients worked together to achieve this. Previous research into CBD and THC as treatments for cancer have had contradictory results at times, with THC having been shown in some studies to decrease tumour growth, but has been shown to increase cancer cells in other studies.
Doctors also acknowledged that they were unable to confirm the full list of ingredients in the CBD oil this particular patient took.
The patient certainly believe the CBD oil made the difference, and was quoted in the report as being “over the moon” and intending to continue taking the CBD oil “indefinitely.”
But one case report does not prove the treatment works — yet.
“Although there appears to be a relationship between the intake of ‘CBD oil’ and the observed tumour regression, we are unable to conclusively confirm that the tumour regression is due to the patient taking ‘CBD oil’,” the report stated.
“More research is needed to identify the actual mechanism of action, administration pathways, safe dosages, its effects on different types of cancer and any potential adverse side effects when using cannabinoids.”
3 years after legalization, number of cannabis charges pardoned is low: expert
‘Very few Canadians actually knew that the system existed,’ said researcher Akwasi Owusu-Bempah
CBC Radio · Posted: Oct 24, 2021
While many, including business owners and producers, have benefited from the federal government’s legalization of marijuana three years ago, programs to expunge certain past cannabis convictions have a long way to go, says one expert.
The federal government said that an estimated 10,000 Canadians would be eligible for its cannabis amnesty program, offering free pardons to those convicted of simple possession of cannabis, when it launched two years ago, but Akwasi Owusu-Bempah says only around 500 individuals have been pardoned so far.
Numbers provided to CBC News indicate 780 applications for pardons were submitted to the Parole Board of Canada between Aug. 1, 2019 and Oct. 1, 2021.
“Very few Canadians actually knew that the system existed; that this record suspension system had been introduced,” said Owusu-Bempah, assistant professor of sociology at the University of Toronto and director of research for the Campaign for Cannabis Amnesty.
“Even for those that do know it exists, the parameters are rather narrow.”
Owusu-Bempah said that police will often charge individuals with multiple offences beyond simple possession, and those charged may choose to avoid the process of seeking amnesty. He adds that time restrictions on when individuals can apply, as well as documentation requirements, create additional barriers for those seeking pardons.
“So although the system is in place, it is not one that’s easily navigated by individuals who are eligible, even for those that do know that it exists.”
With the third anniversary of the Cannabis Act’s passing, the federal government is set to undertake a statutory review of the law.
Public Safety Canada declined to provide a statement on the number of pardons given to date.
Cannabis convictions affect Black, Indigenous communities
For Vivianne Wilson, owner of the retailer GreenPort Cannabis in Toronto, the government’s decision to legalize marijuana is one to be applauded.
But three years on, she believes that too little action has been taken on the issue of pardons.
Wilson says that Black and Indigenous people have been disproportionately harmed by the prohibition of marijuana, and have faced charges as a result.
That’s a sentiment echoed by Owusu-Bempah who said those criminal records are keeping many individuals out of the workforce — including from jobs in the now-legal cannabis industry.
A report released Oct. 14 by the Centre on Drug Policy Evaluation and the University of Toronto, and co-authored by Owusu-Bempah, found that 84 per cent of cannabis industry executives are white.
Only two per cent of industry leaders are Indigenous, and one per cent are Black.
Wilson, who bills herself as the first woman of colour to own a cannabis company in Canada, wants that to change.
As the three-year review of the Cannabis Act approaches, she hopes to see governments commit to reconciliation for those affected by the criminalization of the drug.
“[That] could be financial — hopefully financial from the tax dollars that they’re gaining from the industry. That’s something that we definitely need to see to address some of the past injustices that [have] been done,” Wilson said.
Gov’t can offer financial help for those with past convictions: Owusu-Bempah
Beyond clearing the criminal records of those charged with cannabis-related offences, Owusu-Bempah agrees that the government can redirect a portion of revenues to communities who have been historically targeted by prohibition laws.
What’s more, they could create avenues for those same individuals to enter the cannabis industry.
State governments in Illinois and New York have taken similar approaches in their laws decriminalizing marijuana for recreational use.
Social equity programs in those states have been set up to allow those negatively impacted by criminalization of marijuana to benefit from its legalization.
It’s an acknowledgement, said Owusu-Bempah, that “we’ve spent decades enforcing unjust laws that have had a disproportionately negative impact on largely Black and brown people in poor neighbourhoods and the resources that could have been spent on things like schools, community centres [and] libraries.”
Story From – CBC Cross Country Checkup
Toronto moving forward with plan to decriminalize all drugs for personal use
Jack Landau – Blog TO – September 2, 2021
After a few years of discussion, a report released by Toronto Medical Officer of Health Dr. Eileen de Villa at the beginning of June got the ball rolling for what could be a monumental shift in the way policing is carried out in this city.
The report recommended that the city create a working group with police and people with relevant lived experiences to develop a proposal to the federal government that would exempt locals from drug laws under the Controlled Drugs and Substances Act, effectively decriminalizing all substances for personal consumption in the 416.
Of course, this plan would be subject to federal approval, something far from guaranteed.
Even if approved, people probably shouldn’t interpret decriminalization as a green light to take up a new side hustle. Trafficking and other drug-related offences would remain as illegal as ever, with the policy instead aimed explicitly towards users.
This “Developing an Alternative Model to Drug Criminalization in Toronto” plan is now moving to its next phase, with Toronto Public Health initiating the process to secure a federal exemption.
Part of this plan involves public feedback to inform the Toronto Public Health exemption request to Health Canada. The city has released an approximately ten-minute-long survey asking respondents to share their views on various issues stemming from decriminalization.
These topics include the objectives of drug policy in Toronto, benefits or challenges of decriminalization, the role of police, allocation of public services, barriers to drug users seeking these services, and limits on possession of specific quantities of drugs.
If the exemption were to be approved by the federal government, Toronto’s municipal borders would suddenly become lines of demarcation for drug tolerance.
It is unknown how such a radical change would affect surrounding municipalities, especially concerning police jurisdiction. Roads like Steeles Avenue and waterways like Etobicoke Creek and the Rouge River could transform into frontiers of differing local drug policies.
Other questions remain, such as how the TTC’s Special Constables would manage this policy on Toronto’s transit routes — some spilling out into neighbouring municipalities like the northwestern branch of the Line 1 subway which crosses into Vaughan.
The basis for this move is the growing awareness that drug policy enforcement disproportionately affects vulnerable and racialized communities, with a goal of harm reduction.
Story from – Blog TO
Are Psychedelics Legal In The US? Where Are They Decriminalized? A Deep Dive Into The Legal Status of Psilocybin, MDMA, LSD, Ketamine And More
This article was made possible thanks to research from Calyx Law, the Emerge Group and Psilocybin Alpha.
As psychedelics like LSD, ayahuasca and “magic mushrooms” come rushing back into the public conversation, a few simple questions come up after discussing the potential of these substances in treating a wide variety of mental health disorders:
Contents
- What Are Psychedelics?
- Are Psychedelics Legal In The U.S.?
- Where Are Psychedelics Allowed In The U.S.?
- Where Are Psychedelics Being Considered For Legalization?
“Psychedelic” is a broad term that encompasses a few different substances, some of which enjoy decriminalization or “low-level law enforcement” in certain jurisdictions around the country.
Psychedelics are usually described as drugs capable of producing non-ordinary states of consciousness.
While there are hundreds of natural and synthetic substances that can fall into the general definition of “mind-altering drugs,” most people refer to some compounds in particular when speaking of psychedelics:
- LSD, or Lysergic Acid Diethylamide. Street names: acid, mellow yellow.
- Psilocybin, a compound naturally produced by Psilocybe mushrooms. Street names: magic mushrooms, shrooms.
- Mescaline, naturally found in the Peyote and San Pedro cacti.
- DMT, or dimethyltryptamine, is a compound found in ayahuasca, a traditional Amazonian concoction used in shamanic rituals.
- Ibogaine, naturally produced by the iboga plant, a shrub native to West Africa.
- 5-MeO-DMT, a psychedelic toxin produced by the Sonoran Desert Frog and some plants. Street name: toad venom.
- MDMA. This “empathogen” can be considered a drug of a different category from the “classic psychedelics” listed above, but it’s often grouped within this definition. Street names: ecstasy, molly.
Are Psychedelics Legal In The U.S.?
As a general rule, all of the substances listed above are considered Schedule 1 substances by the federal government and are therefore illegal to produce, sell, possess or consume without special government authorization.
As a general rule, all of the substances listed above are considered Schedule 1 substances by the federal government and are therefore illegal to produce, sell, possess or consume without special government authorization.
Although scheduled, every one of these substances is currently under clinical research and most are expected to become approved in the coming years as psychiatric medication for specific mental health indications.
In the meantime, some U.S. jurisdictions have passed legislation reducing law enforcement of some psychedelic substances, allowing for the use and possession of small amounts of these drugs.
Exception: The Case Of Ketamine
Ketamine is a dissociative drug originally approved as an anesthetic in 1970. In recent decades, its psychedelic-like effects were discovered to produce a reduction in depression symptoms.
While ketamine is only officially approved as an anesthetic, physicians are allowed to prescribe it off-label for the treatment of depression and other mental disorders.
This has placed ketamine at the forefront of the psychedelics movement, as a prescribable drug that can be legally administered at clinics under physician supervision.
Where Are Psychedelics Allowed In The U.S.?
Using Psilocybin Alpha’s Psychedelic Legalization & Decriminalization Tracker, we compiled a list of U.S. jurisdictions where psychedelics are allowed.
Oregon
In November 2020, Oregon became the first U.S. state to eliminate criminal penalties for all illegal drugs including cocaine, heroin, oxycodone and methamphetamine, as well as every psychedelic substance like LSD, psilocybin and MDMA.
Possession of small amounts of these substances were made a Class E violation, instead of a misdemeanor. This reduces penalties to a $100 fine or the option to enlist in one of the state’s “Addiction and Recovery Centers.”
Additionally, in the same 2020 ballot Oregonians voted to launch a program for the therapeutic use of psilocybin, creating the country’s first state-licensed psilocybin-assisted therapy system.
The program, currently in development, will allow patients over the age of 21 to buy, possess and use psilocybin under the supervision of trained facilitators, while manufacture, delivery and administration of psilocybin will be allowed at supervised, licensed facilities.
California: Santa Cruz and Oakland
While the state of California still places a ban on scheduled psychedelic molecules, two cities within its borders have passed resolutions preventing the city from spending resources in imposing criminal penalties for the use and possession of entheogenic plants and fungi.
In both Santa Cruz and Oakland, personal use, possession and cultivation of plants like iboga, mescaline cacti, the ingredients in ayahuasca as well as psilocybin mushrooms are classified among the lowest law enforcement priorities. In Oakland, purchasing, transporting and distributing these natural psychedelics fall into the same category.
District of Columbia
Similar measures were passed in Washington D.C., where psychedelic plants and fungi became decriminalized in November 2020.
“Non-commercial planting, cultivating, purchasing, transporting, distributing, engaging in practices with, and/or possessing entheogenic plants and fungi” are considered “lowest enforcement priorities” by the DC Metropolitan Police, banning the investigation and arrest of persons 18 years of age or older for these practices.
Colorado: Denver
Denver became the first U.S. jurisdiction to reduce penalties on psilocybin mushrooms in May 2019. Psilocybin mushrooms are among the “lowest law enforcement priority,” preventing law enforcement from using Denver city funds for criminalizing the personal use and possession of these fungi.
Michigan: Ann Arbor
Ann Arbor is currently the only city in the American Midwest where cultivating, purchasing, transporting, distributing, engaging in practices with, or possessing natural psychedelics is not criminalized.
Entheogenic plants or plant compounds, which are on the Federal Schedule 1 are a “lowest law enforcement priority,” meaning that “city funds or resources shall not be used in any investigation, detention, arrest, or prosecution” and that the district attorney must “cease prosecution of persons involved in the use of entheogenic plants or plant-based compounds.”
Massachusetts: Somerville, Cambridge and Northampton
In January 2021, the Boston suburb of Somerville passed a legislation wherein no “city funds or resources” shall be used “to assist in the enforcement of laws imposing criminal penalties for the use and possession of entheogenic plants by adults.”
Soon after, neighboring cities of Cambridge and Northampton adopted the same legislation, which states that “the investigation and arrest of adult persons for planting, cultivating, purchasing, transporting, distributing, engaging in practices with, and/or possessing entheogenic plants shall be amongst the lowest law enforcement priority,” calling upon the District Attorney to cease prosecution of persons involved in these practices.
Where Are Psychedelics Being Considered For Legalization?
Federal legislation decriminalizing psychedelic substances does not appear to be on the horizon despite the approval of specific psychedelic substances for medical use via the FDA clinical trial pipeline.
In late July, Rep. Alexandria Ocasio-Cortez reintroduced an amendment to remove federal barriers to research the therapeutic potential of psychedelic substances. The measure was widely rejected by the House, although floor support grew from a previous introduction of the same measure in 2019.
However, several U.S. states have recently passed legislation that calls for research around psychedelic molecules. Other states have bills in congress that could enact further measures around psychedelic legalization.
In California, a bill is being considered that would remove penalties for the possession, personal use and social sharing of certain natural and synthetic psychoactive drugs including psilocybin, DMT, ibogaine, mescaline, LSD, ketamine and MDMA.
The bill passed a Senate vote and is currently on track to the Assembly floor. In a recent interview with Benzinga, Sen. Scott Wiener, the bill’s main sponsor, said he is in favor of full drug decriminalization and this measure is a first step toward that goal.
In 2021, Connecticut and Texas approved bills that launched working groups to study the medical use of psilocybin. In Texas, MDMA and Ketamine are also being studied for the same purpose, with military veterans as the main target group for these therapies.
A similar resolution to study the therapeutic potential of psilocybin was introduced in Hawaii, where a separate senate bill to deschedule psilocybin is also under consideration. In an interview, Hawaii Senator Stanley Chang told us that the goal of the bill is to remove psilocybin and psilocin from the list of Schedule I substances and require Hawaii’s Department of Health to establish treatment centers for the therapeutic administration of these compounds.
Measures involving the decriminalization of psychedelics have also been introduced in a number of other state legislatures, including Florida, where a psilocybin legalization bill died in the senate. In Illinois, a bill to loosen restrictions on entheogenic plants was introduced but never made it to a floor vote.
Iowa, Maine, Missouri, Vermont and New York currently have active bills in their legislature that could bring different levels of decriminalization to certain psychedelic substances. In the Empire State, a bill introduced by Assemblywoman Linda Rosenthal would establish a psychedelic research institute and a therapeutic research program to study and provide recommendations on the use of psychedelic substances.
As investors, scientific institutions and the general public grow more knowledgeable and interested in the medicinal potential of psychedelics, more states and jurisdictions are expected to roll out further bills and legislative moves that will hopefully open access to psychedelics in different ways across the country.
Story from – Yahoo
Why we love drugs
Michael Pollan on America’s broken — but improving — relationship with drugs.
What makes a drug a drug?
It’s strange to say, but we don’t really have a good definition of the term. You could say a drug is any substance that transforms our subjective experience of the world, but food does that, too. So what’s the difference?
In this country, it turns out the difference is pretty arbitrary. Drugs are whatever the government says they are. And for a long time, the government has classified them in a deeply dishonest and cynical way. We call this absurdity “the drug war.”
But here’s the good news (especially if you’re one of the groups victimized by it): The drug war is dying. You can see it in the marijuana legalization movement and you can see it in the so-called psychedelic renaissance. The country will have to think seriously about what comes next. How will our taboos shift? What sorts of reforms will we need? What kind of cultural infrastructure should we build?
Michael Pollan is perhaps best known for his 2006 book The Omnivore’s Dilemma, but his 2018 work How to Change Your Mind did more than any other to vault psychedelics into the mainstream, and it remains one of the best explorations of the therapeutic potential of psychedelics.
Pollan’s latest book, published in July, is titled This Is Your Mind on Plants. This one is about psychedelics too, but it’s a much broader look at our all-too-human obsession with psychoactive plants — not just hallucinogens, but also caffeine and opium — and why our culture has such a fraught relationship with them.
So we talk about all that, and we explore what we can learn from other cultures about how to use psychedelics, and why he thinks these plants are powerful antidotes to our disconnected lives.
You can hear our entire conversation (as always, there’s much more) in this week’s episode ofVox Conversations. A transcript, edited for length and clarity, follows.
Read and Hear more here … Vox Podcast
The future of psychedelic science
by Ryan O’Hare –
From treating depression to understanding consciousness, the promise of psychedelics is shifting their study from fringe to frontier neuroscience.
In 2019 a small group of researchers at Imperial established the world’s first dedicated centre for research into the action and clinical use of psychedelic compounds.
Two years on, the Centre for Psychedelic Research has completed landmark studies into the therapeutic potential of magic mushroom compound psilocybin for depression, exploring the ‘waking dream state’ linked to ayahuasca, and digging deeper into the science of micro-dosing with LSD.
Ryan O’Hare spoke to Dr Robin Carhart-Harris, the head of the Centre, to discuss what’s in store for the future.
Here are five of the big questions the work of the Centre for Psychedelic Research hopes to answer in the future.
1. How do psychedelics change our brain?
Work from the Centre has shown that psilocybin may help to ‘reset’ the brain and break out of long-entrenched patterns of activity seen in depression.
Early, unpublished follow up work from the team shows that when people are shown emotionally charged faces, SSRI antidepressants (drugs like fluoxetine and escitalopram) blunt the response to all faces, but psilocybin may only dampen the negatively charged faces.
Dr Carhart-Harris explains: “With the Prozac-like antidepressant…we see a dampening or muffling of the brain’s responsiveness to emotional stimuli relative to the psilocybin. That makes sense because the psilocybin is more like an emotional recalibration or reset, whereas the SSRI [antidepressant] is more like taking the edge off emotional intensity which helps with stress management.”
Delving into this further, the Centre plans to study how psychedelics change the activity of our brains. Studies are due to begin analysing brain waves and MRI data in volunteers given psilocybin and DMT (the active compound found in the psychedelic Amazonian brew ayahuasca) to compare their brain activity before and after their experience.
2. How are people using psychedelics and can we reduce potential harms?
Over the last two years, the team has been gathering real-world data on how people are using psychedelic drugs, gaining valuable insights.
Through the ongoing Psychedelic Survey and the imminent launch of the MyDelica app, the team hopes to use a data-driven approach to help inform people intent on taking psychedelics of the importance of the setting, wider context and psychological state on outcomes.
One of the aims is to educate people and provide advice, which may help to reduce harms and ultimately improve psychological outcomes.
“We’ve actually seen, looking at some recent data, that use of psychedelics over the last 10 years has increased exponentially,” explains Dr Carhart-Harris.
“With the online sampling and the app we’re developing, the intention is to de-risk some of that and provide harm reduction, psycho-education advice to try and keep people safe, essentially.”
The researchers warn that people should not attempt to self-medicate or replicate findings from clinical trials with psychedelics, as the team provided a special therapeutic context for the drug experience and things may go awry if the extensive psychological component of the treatment is neglected.
3. Could psilocybin help to treat anorexia?
Following positive initial results in a small trial of psilocybin assisted therapy for depression, the Centre is set to look at whether the same approach could help with anorexia nervosa.
Building on evidence from a small number of historical case studies of using psychedelics in eating disorders, the team will trial psilocybin-assisted therapy in young adults with anorexia to see if the treatment is feasible and effective.
According to the Centre: “Anorexia nervosa is the most fatal of all psychiatric conditions. With the current paucity of effective pharmacological and psychological treatments, and fewer than half of those diagnosed making a full recovery, there is a great need for new treatment avenues to be explored.”
A small study is due to begin in the coming months.
4. Can psychedelics offer relief from chronic pain?
Despite numerous advances in pain relief, effective and non-addictive treatments for long-term chronic pain – such as lower back pain – remain elusive.
There is mounting evidence that in those with chronic pain conditions, the brain connections which relay and processes pain signals can become reinforced and strengthened over time, as part of a feedback loop which sensitises them even more to feeling pain and associated negative emotional response.
Psychedelics could offer an opportunity to ‘reset’ these neural pathways. The hope is that by disrupting this entrenched pain circuitry, psychedelics might offer a way to reduce the brain’s over-sensitivity to pain signals.
According to Dr Carhart-Harris, the Centre hopes to begin a study later this year.
5. What is consciousness?
One of the more fundamental areas researchers are hoping to advance with psychedelics is our understanding of human consciousness.
By analysing brain activity before, during and after psychedelic experiences, the team hopes they can shine more light on brain states linked with the so called ‘mystical experience’ associated with psychedelics.
The team has already laid some of the groundwork, with its previous DMT research into the ‘waking dream state’ linked to ayahuasca. It is thought that a better understanding of how different patterns of brain activity give rise to hallucinations and waking consciousness could enable us to nudge the brain when it’s stuck in certain negative patterns.
Psychedelics could potentially ‘reset’ brain activity and enable people to break out of entrenched, negative behaviour patterns – linked to addiction, depression or pain, for example – which have been reinforced and strengthened over a person’s lifetime.
“DMT is a particularly intriguing psychedelic,” Dr Carhart-Harris commented previously. “The visual vividness and depth of immersion produced by high-doses of the substance seems to be on a scale above what is reported with more widely studied psychedelics such as psilocybin or ‘magic mushrooms’,” he explained.
“Our sense it that research with DMT may yield important insights into the relationship between brain activity and consciousness, and [our previous work] is a first step along that road.”
Article from – Imperial College London – UK News
Drug decriminalization: Vancouver mayor proposes amounts users should be able to carry
Monday, April 12, 2021
VANCOUVER — The City of Vancouver has outlined the amounts of various drugs people should be allowed to carry for a three-day supply as it seeks a federal exemption to decriminalize the possession of small amounts of drugs for personal use.
Its proposal aimed at combating the overdose crisis is part of an application to Health Canada and lists possession thresholds for four main drugs: opioids such as heroin and fentanyl, cocaine, crack cocaine and amphetamine.
The recommended amounts for opioids are listed as two grams, while three grams are proposed for cocaine, one gram or 10 rocks for crack cocaine and 1.5 grams for amphetamine, based on long-term studies of drug users.
The effort is aimed at removing criminal sanctions and reducing stigma as part of a health-focused approach to substance use.
British Columbia has also asked for a federal exemption to decriminalize the possession of small amounts of drugs for personal use after a record number of people died from overdose last year.
This report by The Canadian Press was first published April 12, 2021.
Story from – BC CTV News
PROMISES MADE
2 Years After Legalizing Cannabis, Has Canada Kept Its Promises?
Legal pot has made Canadian justice a little fairer, with “heavily racialized” arrests for possession mostly ending. But vows on amnesty, illicit sales and Indigenous inclusion are works in progress.
OTTAWA — When Robert was 18, he was arrested by Montreal’s police for possession of a small amount of hashish, an event that would upend his young life.
The charge brought him 30 days in jail, and the conviction ended his part-time job as a translator.
“Back then, you smoke a joint, you would get arrested,” said Robert, who asked that only his first name be used because of the continuing stigma of his criminal record. “Then the cops would put you in a car, then pull over and give you a couple of shots in the head. You get slapped around just because of smoking.”
His arrest in 1988 as a teenager marked the start of a long, unhappy history with Canada’s legal system, with his first jail stint opening up a new trade: burglary.
“It was like school,” said Robert, who spent a total of 14 years locked up, roughly divided between convictions on drug offenses and thefts to buy more drugs. “I went there for smoking and then guys are showing me how to open doors.”
That promise has largely been kept, with legalization essentially ending what Akwasi Owusu-Bempah, a professor of sociology at the University of Toronto who studies race and policing in Canada, called the “heavily racialized” arrests for marijuana possession.
But some other key promises, and hopes, that came with Canada being the first industrialized nation to legalize marijuana remain unfulfilled.
The for-profit industry it created has struggled. Pot sales outside the legal system still thrive. Indigenous communities feel their needs are being ignored. And the injustices that came from criminalizing pot in the past have yet to be fully remedied.
As more of the United States legalizes marijuana, with voters in New Jersey, South Dakota, Montana and Arizona this past November backing recreational use, joining about a dozen other states, here’s a look at the Canadian experience two years into its national experiment.
WHAT WE FOUND
An Emphasis on Fairness and Equality
Mr. Trudeau’s pledge to legalize marijuana was not universally welcomed by Canadians, including some members of his Liberal party, who feared it would encourage use, particularly among teenagers.
But the prime minister persuaded his party, and many voters, with an argument based on fairness and equality.
Mr. Trudeau illustrated the system’s bias with a family story. In a 2017 interview with Vice, he said that his brother, Michel, was found carrying a couple marijuana joints by the police in 1998, six months before he was killed in an avalanche.
Their father, Pierre Trudeau, a former prime minister, came to the rescue.
“We were able to make those charges go away,” Mr. Trudeau said. “We were able to do that because we had resources, my dad had a couple connections, and we were confident that my little brother wasn’t going to be saddled with a criminal record for life.”
Legalization, he promised, would ensure that not just the connected and wealthy could avoid a criminal record.
A report released in August by the Ontario Human Rights Commission showed just how tied to race cannabis arrests had been before legalization: An analysis of police data found that while Black people made up 8.8 percent of the population of Toronto, they faced 34 percent of marijuana possession charges there between 2013 and 2017.
The police have lost one tool they once used, Professor Owusu-Bempah said, “as a way of bringing certain marginalized populations into the criminal justice system.”
But how much change that’s brought to the system as a whole is open to question. While Canada is only starting to collect crime and police data that includes race, several leaders from minority communities continue to demand action against what they call systemic racism within many police forces. Last June Mr. Trudeau acknowledged that systemic racism is found in the Royal Canadian Mounted Police, the national police force, and other law enforcement agencies.
WHAT WE FOUND
‘I’ve Got So Much Against the System’
While decriminalizing marijuana possession is viewed as a step toward building a fairer justice system, many charged under the old law are still dealing with the devastating consequences, despite promises of redress.
“We haven’t reckoned as a country with the impact that drug prohibition has especially had on Black Canadians,” Professor Owusu-Bempah said. “Unfortunately, too many of them are being left with a criminal record.”
The legalization effort came with an amnesty program the government said would erase criminal records for possession, but there are barriers to access.
While there is no government statistic for the number of Canadians with possession records, a 2014 report by the Center for Addiction and Mental Health, a Toronto hospital and research center, put the figure as high as 500,000.
As of mid-November, just 341 people had succeeded in erasing their records. There are no fees, but applicants must frequently spend money to travel to the place of their arrest to retrieve their records, and they must be fingerprinted.
Even if Robert, who has lived in Vancouver the past 25 years, could afford to return to Montreal, he says it wouldn’t be worth it. Removing the possession charges would not alter the theft convictions that followed.
“I’ve got so much against the system,” said Robert, who has stayed out of jail the past decade and works for an overdose-prevention group. “It made everything go out of my reach.”
When marijuana was illegal in Canada, the Green Mile was a popular place to buy it, with about a dozen mismatched shops along a stretch of highway in Ontario offering every kind of cannabis product imaginable.
“These people know what I’m looking for,” said Jess Lihou, whose one-hour drive to Maryjane’s Cannabis Dispensary in the Green Mile was justified, in her view, for two main reasons: price and selection.
The licensed retail chains “don’t have enough options,” Ms. Lihou said: “And it’s cheaper. So great deals and great people.”
The provincial police in Ontario generally respect the sovereignty of Indigenous communities and take enforcement action against shops like those along the Green Mile only if requested by a community’s leaders.
But the new system has been criticized for keeping these Indigenous operations in a gray-market legal limbo, despite promises that Indigenous people would be consulted and made part of the new system.
“Legalization happened so quickly that these issues of equity and issues of sovereignty with respect to Indigenous people were not properly addressed,” Professor Owusu-Bempah said. “The government’s still trying to figure out exactly what it wants to do.”
In Ontario, the provincial government is meeting with Indigenous leaders about the shops, according to Jenessa Crognali, a spokeswoman for Ontario’s attorney general.
But with their legal status still unclear, the threat of being shut down hangs over Green Mile shops.
“We’re hopeful, but we’ve never been too confident,” said Laurie Marsden, a co-founder of one of the shops, Healing House, which emulates the provincial system by running a lab that tests for potency and contamination. “We believe in our sovereign rights and that we have the ability to produce, grow and sell the medicines to our customer base.”
WHAT WE FOUND
Profits, and Diversity, Hard to Find in Legal Market
When Mr. Trudeau announced his government’s plans for legalization, the creation of a major new source of jobs — or tax revenue — was not in the program.
But investors envisioned tremendous business opportunities, as a “green rush” swept the Toronto Stock Exchange and legal players invested millions of dollars in supersized greenhouses.
Two years later, most marijuana producers are still reporting multimillion-dollar losses.
And these companies’ executives are overwhelmingly white, according to an analysis by Professor Owusu-Bempah. It concluded that 2 percent of the companies’ leadership are Indigenous people and 1 percent are Black Canadians.
“African-Canadians and other racialized Canadians that were adversely affected by cannabis prohibition need to be given a chance to benefit from the fruits of legalization,” Professor Owusu-Bempah said. “We had this situation where Black and Indigenous people were being overly criminalized. Now they’re being left out of what is a multibillion-dollar industry.”
WHAT WE FOUND
‘Not Just Going to Roll Over and Go Away’
In addition to a fairer legal system, the government promised legalization would shift marijuana sales out of the black market, parts of which are dominated by organized crime.
“By controlling it, by legalizing it,” Mr. Trudeau said in 2018, “we’re going to ensure that criminal organizations and street gangs don’t make millions, billions of dollars of profits every year.”
And the strict regulations governing legal sales, the prime minister promised, would ensure that Canadians were consuming marijuana not adulterated with other drugs or toxins and would eliminate sales to minors.
The current pot scene in Vancouver is a good illustration of a promise that still has a ways to go before being fulfilled.
The city once had more pot shops than Starbucks, with more than 100 at the peak. Now, there are about 19 unlicensed shops, along with 34 legal operators, numbers that broadly reflect the situation across Canada: Sales outside the legal system are shrinking but have not disappeared.
With loyal customers and often a competitive advantage on price (with no taxes to pay) and selection, the illegal shops are hanging on.
“They’re not just going to roll over and go away,” said Mike Farnworth, the minister of public safety in British Columbia.
In its latest survey released just over a year ago, Statistics Canada, the census agency, found that 28 percent of Canadians shopped for marijuana exclusively at legal stores and websites, while 58 percent used a mix of legal and illegal sources.
Shutting down the unlicensed stores has not been a priority amid an opioid crisis: In British Columbia, from January through November 2020, 1,548 people died from overdoses.
For Canada’s illegal growers, marijuana “is still a good business,” said Detective Inspector Jim Walker, deputy director of the Ontario Provincial Police’s organized crime enforcement bureau.
But there are clear signs the legal domestic option is forcing gangs to look elsewhere. The number and size of seizures of outbound marijuana, said Mr. Walker, referring to pot headed to the United States, “are growing exponentially.”
Tracy Sherlock contributed reporting from Vancouver, British Columbia.
Story From – The New York Times
Smoking Cannabis Flower May be the Best Way to Combat Chronic Pain Says New Medical Study
Is actually smoking weed the best way to deal with pain issues in the body?
Smoking Flower May Be The Best Way To Combat Pain, Says New Medical Study
Over 1.5 billion people globally suffer from chronic pain, says the American Academy of Pain.
In fact, pain is the most common reason people suffer from long-term disability in the United States, affecting some 100 million people. Pain is no joke: for many, it’s so debilitating that doing seemingly normal tasks like getting out of bed or doing household chores can be a huge challenge.
So it’s no surprise that so many are turning to cannabis as a way to naturally manage pain. Cannabis has powerful analgesic properties that many over the counter pharmaceuticals can’t beat. And with so many ways to consume cannabis these days, medicating for pain has never been more convenient.
However, researchers have found that smoking flower could be the most efficient way to medicate for pain. A recent study conducted by researchers from the University of New Mexico revealed that pain patients have a better chance of efficiently managing pain when smoking flower compared to the other forms of cannabis consumption. The findings state that “whole cannabis flower was associated with greater pain relief than were other types of products.” They also add that “higher tetrahydrocannabinol (THC) levels were the strongest predictors of analgesia and side effects prevalence across the five pain categories.”
“Perhaps the most surprising result is just how widespread relief was with symptom relief reported in about 95% of cannabis administration sessions and across a wide variety of different types of pain,” says Xiaoxue Li, the study’s lead author.
“Our results confirm that cannabis use is a relatively safe and effective medication for alleviating pain, and that is the most important message to learn from our results,” says Jacob Miguel Vigil. “It can only benefit the public for people to be able to responsibly weigh the true risks and benefits of their pain medication choices, and when given this opportunity, I’ve seen numerous chronic pain patients substitute away from opioid use, among many other classes of medications, in favor of medical cannabis.”
“Cannabis likely has numerous constituents that possess analgesic properties beyond THC, including terpenes and flavonoids, which act synergistically for people that use whole dried cannabis flower,” Vigil says.
“Overwhelmingly, when the whole plant is used rather than isolating one compound of the plant inevitably it’s more effective,” explains Om of Medicine co-founder Mark Passerini, who worked with the University of Michigan for an International Review Board sanctioned survey on opioid and cannabis use.
Other Benefits Of Smoking Flower
Aside from the notable medical benefits of smoking flower, there are many reasons it continues to be the most popular way of consuming cannabis. It’s extremely versatile but it’s also so simple to consume; whether you want to use a bong or pipe, or rolling it up into a blunt or joint, smoking flower is champion for most.
Smoking flower also has a quicker onset; because of its extremely high bioavailability, that means you can feel its effects much quicker. Not only will you get high quicker, but it will also deliver pain relief within minutes whereas pharmaceutical drugs often take half an hour to work and in the case of other medicines, you have to take them for 2 weeks to see relief. But unlike medications, smoking flower doesn’t have any side effects for your kidneys and livers just to feel its impact.
When smoking a high-THC strain, you also don’t need a lot to feel its effects. That can make flower a very economical choice since a little goes a long way. However, keep in mind that smoking flower doesn’t have any standard dosing unlike other forms of consumption. That means the only way to truly find out how much works for you is by trial and error. So if you come across a strain with 18.64% THC, that means you’ll get around 186.40mg of THC in every gram of flower. If it’s your first time to smoke flower, always start small and then work your way up gradually until you find what works best for you.
Most of all, the best part of smoking flower is that you get its full-spectrum of health benefits in its purest, most natural form. You also get the benefits of the Entourage Effect, which means that all the compounds and benefits of the plant enhance each other synergistically to give you the most efficacious experience. This effect cannot be felt with other forms of consumption since smoking flower is the only way to make sure that the complete range of secondary compounds and terpenes are present too. So while concentrates and edibles are equally popular ways to medicate, most of the secondary compounds have already been burned off during the extraction process because it involves high heat. For this reason, many people especially those suffering from chronic pain don’t experience maximum relief when consuming concentrates. On top of all these awesome benefits, you also get much more flavor and terpenes when smoking flower. It makes the whole process of medicating so much more enjoyable.
With new research telling us that smoked cannabis flower being the top method of medicating for pain, it’s a good excuse to go out there and experiment with strains that are best known for combating pain. You can even mix it up with concentrates and edibles to enhance the symptom relief. There’s no limit to the relief you can get once you start trying cannabis for pain instead of pharmaceutical meds.
Story from – Cannabis.net
House votes to federally decriminalize marijuana
Friday marks the first vote ever of its kind on a federal level.
Oregon first state to legalize hallucinogenic ‘magic’ mushrooms
By CELINE CASTRONUOVO – November 4, 2020
Oregon has become the first state in the country to legalize psilocybin, or psychedelic mushrooms, with the passage of a state ballot measure Tuesday.
According to The Oregonian/OregonLive, Measure 109 passed Tuesday evening with approximately 56.1 percent support from voters.
The measure, backed by chief petitioners and psychotherapists Sheri and Thomas Eckert, will permit regulated, therapeutic use of psychedelic mushrooms.
The Oregonian/Oregon Live reported that the new mandate will allow anyone age 21 or older to access the drug for “personal development” upon passing a screening.
Research at universities including Johns Hopkins, Imperial College in London and the University of California, Los Angeles, have shown indications that psychedelic mushroom therapy could be helpful for patients experiencing depression, PTSD and addiction.
“We need options. And this is a valid therapeutic option that could help thousands of people,” Tom Eckert told The Oregonian/OregonLive in September.
Oregon voters on Tuesday also approved a ballot measure that will decriminalize the possession of small amounts of harder street drugs including heroin, methamphetamines and cocaine.
The ballot measure would mean that the possession of a “non-commercial” amount of a number of drugs would be punishable by no more than a $100 fine. Violators can also opt to complete a health assessment for drug addiction instead of paying a fine, and the measure also sets up free addiction recovery centers funded by tax revenue from retail marijuana sales.
The measures in Oregon come as voters in Washington, D.C., voted to decriminalize the growing, possession and noncommercial distribution of hallucinogenic mushrooms on Tuesday.
More than 76 percent of voters in the nation’s capital supported the initiative with just over 40 percent of precincts reporting, according to the district’s Board of Elections.
Cities across the country have previously decriminalized the use of psychedelic mushrooms, with Denver, Colo., being the first to do so with a ballot measure in May 2019. Other cities have since followed, including Ann Arbor, Mich., and the California cities of Santa Cruz and Oakland.
Story from The Hill
Mental illness is on the rise due to COVID-19.
Could psychedelic drugs be the ‘game changer’?
Thomas Hartle is a 52-year-old IT technician from Saskatoon who doesn’t smoke, rarely drinks and never dabbled in drugs before trying medicinal cannabis. As part of his profession, the soft-spoken, detail-oriented father of two typically spends much of his time planning and researching.
But these days his preparations have taken a devastating turn — planning for his family’s future as he awaits his imminent death.
Hartle was diagnosed in April 2016 with stage-four colon cancer. It went into remission, but last year he learned it was back, had spread and will ultimately kill him. What followed were crippling panic attacks triggered by worries for his family and the uncertainty of not knowing which day could be his last.
“What caused the anxiety for me was the fact my cancer is completely invisible to every test they do. So I literally have no idea the extent or severity of my cancer right now … and neither do the doctors.”
But now Hartle is no longer spending his life worrying about death. He has come to terms with the concept of dying thanks to an unconventional treatment: Psychedelic-assisted psychotherapy.
Hartle was one of the first four Canadians approved by the federal government in August to use psilocybin, the active ingredient in magic mushrooms, for end-of-life anxiety treatment. He is one of the first known patients in Canada to be granted permission to use the drug for non-research purposes since it was criminalized in 1974.
The federal government says since August it has granted 11 exemptions for patients to use psilocybin and expects to make a decision soon on therapist use.
Researchers say the government’s recent decision to allow terminally ill Canadians to use psilocybin is an example of the psychedelic sphere opening up, leading some to say the class of drugs, also known as hallucinogens, is having its moment in the mainstream.
In the 1950s and ‘60s, there was a wealth of research into the efficacy of psychedelics in treating mental health conditions and to better understand psychosis and hallucinations in patients with schizophrenia. But the counterculture of the 1960s led to the class of drugs being demonized and criminalized. Most research into their potential has since stalled.
Advocates of psychedelic-assisted therapy emphasize that the drugs themselves are just one part of the treatment and must be used within a therapeutic context under the supervision of a trained professional to be effective. Psychedelic drugs are not for everyone, they say, and could be destabilizing or detrimental for certain people.
For some, however, there is evidence psychedelic drugs can be useful in psychiatry. Despite this, the medical establishment and governments have been apprehensive about embracing psychedelics for psychotherapy. And because the drugs are still illegal in most of the world, research and treatment are difficult or prohibited.
“They have some challenges regular kids don’t have. And as a result, you kind of have to plan a little more extensively. For me, unfortunately, those plans have a limited calendar,” Hartle said from his home in Saskatoon.
Since his first psychedelic therapy session in August, Hartle said his anxiety levels are “markedly lower.”
During the session, he sat in bed blindfolded and listened to music under the supervision of a therapist. He described the experience as calming and serene and said experiencing different states of consciousness helped him accept “this isn’t all there is.”
He said the session largely eliminated the constant negative chatter in his head and made him feel he can actually live in the moment.
“Just imagine you’re out at a nice supper with your family, your family’s having fun, but the only thing in your head is worrying about what’s going to happen next. Now … I’m actually there.”
It was Hartle’s dedication to meticulous research that led to him finding TheraPsil, an organization that has been lobbying the federal government to allow psilocybin to be used by palliative-care patients and therapists to treat end-of-life anxiety. He decided it was worth trying, after finding relief from chemotherapy side effects with medicinal cannabis.
The federal government is now considering granting an exemption so therapists can also use psilocybin for training purposes. TheraPsil’s CEO Spencer Hawkwell said they’ve been told a decision is coming soon.
On Oct. 22, Numinus Wellness Inc., a Vancouver-based company researching and developing psychedelics for psychotherapy, announced it has completed the first legal harvest of magic mushrooms by a public company in Canada. It is the first publicly traded company to be granted a licence by Health Canada to conduct research into extracting psilocybin from mushrooms for research purposes.
Earlier this year in Toronto, Field Trip Health opened what has been called the “first psychedelic-enhanced psychotherapy centre in Canada,” using ketamine, an anesthetic and psychedelic that can provide out-of-body experiences, to treat depression as well as PTSD.
Toronto’s Mind Medicine Inc. is studying the use of LSD (lysergic acid diethylamide) to treat anxiety and as well as the effectiveness of microdoses of LSD in treating adult attention deficit hyperactivity disorder.
In the upcoming U.S. election, psychedelics are on the ballot in two jurisdictions. In the District of Columbia, a piece of legislation proposes making plant-based psychedelics such as psilocybin the lowest enforcement priority for law authorities. A measure in Oregon would go even further, creating a regulated industry for psilocybin therapy.
That’s exactly what Bruce Tobin, the therapist who was present for Hartle’s psilocybin session, is hoping to see in Canada. Tobin is the founder of TheraPsil, the organization that lobbied the government to approve the psilocybin exemption, and a psychotherapist for 40 years.
He said the government’s approval is historic and among the first examples of medical use of psilocybin being approved in North America for close to 60 years.
“I see psychedelics as a potential game changer. And we’re gonna look back on clinical psychotherapy and psychiatry in another 50 years and it’s going to seem like it’s in the dark ages,” Tobin said.
It is believed psychedelics have the potential to address mental health issues because they can unlock parts of our brain that have been buried deep into our subconscious, Tobin said.
He said psilocybin, combined with psychotherapy, can help patients with terminal cancer face “negative emotional material” and come to peace with the concept of death.
“That’s what psychedelics largely do — they throw noises at the system that help you break up your normal framing,” he said. “They shut off a lot of the standard state of self and consciousness.”
He said the need to look at the potential of psychedelics to treat mental health conditions is even more pressing in the age of COVID-19.
“You know what COVID did? It made people feel like they were losing their homes, losing their connections. And at the same time, it put them in this weird almost mythological place where there was this ubiquitous invisible threat out there … and that really spins people out in a powerful way,” Vervaeke said.
Psychiatry is a discipline where lobotomies and shock therapy were once deemed reasonable methods of treating mental illness. But even today, most treatments come with a tradeoff, Tobin said.
Antidepressants most commonly come in the form of selective serotonin reuptake inhibitors, which work for some people, but not everyone. They also come with side effects such as sexual dysfunction, weight gain and loss of personality.
Benzodiazepines, the traditional treatment for anxiety, can cause severe dependency from long-term use.
Story from the Toronto Star
Are Canadians ready to accept psychedelics in palliative care?
Erika Dyck is a professor and a Canada Research Chair in the history of health and social justice at the University of Saskatchewan. She is the author of Psychedelic Psychiatry: LSD from Clinic to Campus.
In August, 2020, Health Canada granted a special exemption to allow four terminally ill patients to take psilocybin. Psilocybin is not legally sold in Canada. In illegal markets it circulates as magic mushrooms, but researchers suggest that psychedelic drugs such as psilocybin have therapeutic potential for easing anxieties, particularly those associated with dying.
Saskatoon resident, 52-year-old Thomas Hartle, who has stage four terminal colon cancer, took psilocybin, under the direction of psychologist Bruce Tobin, with permission from Health Canada. Psychedelic researchers suggest that these drugs help to reduce anxiety, among other benefits that are currently being studied in clinical trials. News reports suggested that Mr. Hartle had a somewhat frightening experience – maybe even a “bad trip.” But, Mr. Hartle’s own view was that it had a remarkable effect on his anxieties about dying. He is grateful for relief he gained from the experience, and now looks forward to his remaining time with his family.
Mr. Hartle’s story is in many ways remarkable, but it aligns with a longer history of psychedelics in Canada.
Psilocybin became famous in the 1950s when husband and wife team Valentina Pavlovna and Gordon Wasson participated in an Indigenous mushroom ceremony in 1955, and later published their findings in Life magazine. Some Indigenous groups have a long history of using plant medicines, some of which were later described as psychedelic.
The word psychedelic was coined in 1957 by psychiatrist Humphry Osmond, a British-trained researcher who conducted internationally significant experiments with drugs including LSD and mescaline (from the peyote cactus) in Saskatchewan in the 1950s, including working with the Native American Church. Famously, Mr. Osmond introduced mescaline to writer Aldous Huxley. Mr. Huxley later gave mescaline to his wife, Maria, as she suffered from late stages of breast cancer. His second wife, Laura, gave Mr. Huxley LSD as he succumbed to his own cancer diagnosis in 1963. Even before the concept of palliative care had been introduced, these early pioneers of psychedelic research recognized the potential for easing the anxieties associated with dying by helping to provide an emotional, psychological, and at times spiritual experience.
Psychedelic research ended in the 1960s due to a combination of scientific, political and cultural backlash, including concerns about psychedelics causing negative effects – flashbacks, bad trips and violent outbursts. Health Canada, like the U.S. Food and Drug Administration, placed restrictions on scientific experimentation and over time psychedelics became better known as recreational drugs, characteristically associated with countercultural hippies. The recreational use and abuse contributed to the popular assumption that psychedelics had no medicinal value. Medical research historically, and today, maintains that these drugs have been unfairly blamed for causing psychological and physical damage. Clinical trials reveal that psychedelics are not addictive, and do not produce harms in adults, though most researchers recommend that psychedelics should be taken in a therapeutic setting only, with qualified supervision. In the case of Thomas Hartle, he was monitored at all times by a qualified therapist familiar with psychedelic treatments.
The recent allowance from Health Canada signals a change in that view. It brings Canada into a growing international conversation about the revitalization of psychedelics, both in research and as a viable mental health treatment option. New psychedelic research units, including two currently in Canada and dozens now in the United States and Europe, are beginning to challenge the prohibition on psychedelics and resurrect some of the historical arguments about the benefits of psychedelics for mental health.
On the surface, the psychedelic renaissance may indicate a collective frustration with the current state of mental health treatments. Daily use pharmaceuticals are expensive, whether for individuals or health care systems. Rates of mental illness have gone up, not down since the dramatic introduction of psychopharmaceuticals in the 1950s. Opiate-based pain relief has created a new set of problems with addiction, overdose, and off-label use.
Psychedelics, whether in the 1950s or now, are often directed as a single-use therapy. They offer a consciousness-raising or pain-confronting approach, not an experience that is necessarily to be repeated, and not an approach meant to dampen or numb pain but to address it through confrontation. In some ways, this approach is an entirely different way of thinking about mental anguish.
Palliative care has also emerged as a hot spot in our health care system. Another Canadian innovation, palliative care units were the idea of Montreal urologist Balfour Mount, who coined the word itself. The development of palliative care and dedicated hospital spaces for dying have helped generate a conversation around dying with dignity, something that can be extended to include the use of psychedelics for terminally ill patients.
We live in a country that pioneered psychedelics as well as palliative care, and one that prioritizes universal health care. Given this legacy, it is fitting that we should explore investments in health care options that combine elements of reconciliation, universality, and dignity.
Article From The Globe and Mail
Medical News & Perspectives – January 4, 1964
LSD Used As Analgesic
JAMA. 1964;187(1):A33. doi:10.1001/jama.1964.03060140099054
A new possibility in the search for an effective, non-habituating analgesic drug is lysergic acid diethylamide (LSD). Heretofore used only in psychic experiments and in studies of schizophrenia, the hallucinogenic drug now is being used experimentally to relieve pain.
The studies are being conducted by Eric Kast, MD, at Cook County Hospital in Chicago, in the department of anesthesiology (Vincent Collins, MD, chairman). Kast is attending in anesthesiology at the hospital and is assistant professor of medicine and psychiatry at Chicago Medical School. Collins is associate professor of surgery at Northwestern University Medical School.
Kast said the drug has been used to date on about 300 patients, most of them in the pre-terminal stages of cancer.
Results are both encouraging and puzzling. Encouraging—because LSD relieves pain much longer than other drugs; puzzling—because many of the patients declined a second administration.
The action of LSD probably is on the enzymatic basis,

Article From – JAMA
The Psychedelic Science of Pain
Psychedelics and Health Research Initiative explores new territory in treating pain
In the last few years, new research has demonstrated the powerful potential for classical psychedelics, especially psilocybin (the active compound in “magic mushrooms”), to treat a range of mental health disorders, including depression, anxiety and addiction. In 2018, the FDA assigned psilocybin a Breakthrough Therapy Designation. In response, UC San Diego’s Arthur C. Clarke Center for Human Imagination organized a new collaboration with groups across campus, including the Center for Human Frontiers at the Qualcomm Institute and the Departments of Anesthesiology and Psychiatry, to launch the Psychedelics and Health Research Initiative (PHRI). Its mission is to study the potential of psilocybin and other related compounds to promote healing and help manage pain.
(a) A circular connectogram showing normal communication between distinct hubs. (b) Markedly increased crosstalk after psilocybin administration. (G. Petri, P. Expert, F. Turkheimer, R. Carhart-Harris, D. Nutt, P. J. Hellyer and F. Vaccarino (2014). Homological scaffolds of brain functional networks. J. R. Soc. Interface. 120140873)
While much of the new research on psychedelics shows its potentially high efficacy for treating psychological disorders, relatively little research has been done to demonstrate their uses for the treatment of chronic pain conditions.
A recently published review paper by UC San Diego PHRI members Timothy Furnish, associate clinical professor of anesthesiology and pain medicine; Joel Castellanos, pain physician for UC San Diego Health and Adam Halberstadt, associate professor of psychiatry, among others, points to the potential for psychedelics to address chronic pain conditions.
Since pain has both physical and affective/cognitive components, the PHRI’s preliminary findings indicate that psychedelics, alone or as part of multi-pronged treatment, can produce significant, meaningful and lasting reductions of chronic pain conditions such as cluster headache, complex regional pain disorder, phantom-limb pain, tinnitus and others. As a non-addictive alternative to opioids, psychedelics represent a revolutionary and much-needed new approach to the treatment of pain.
“Neuropathic pain conditions such as phantom limb pain are often difficult to treat,” says Furnish. “The possibility that psychedelics could reorganize pain pathways in the brain holds out the promise of a much more long-lasting treatment than current medication can offer.”
History of psychedelics research on campus
Research on the classical psychedelics, which include LSD, DMT, mescaline and psilocybin, has a long history at UC San Diego. Mark Geyer, Distinguished Professor of Psychiatry and Neurosciences Emeritus and founding member of the PHRI, has conducted research on the behavioral and neurobiological effects of psychedelics for more than 40 years at UC San Diego. He also helped start the Heffter Research Institute in 1993, dedicated to renewing research into beneficial uses of psychedelics—research that had been cut off prematurely during the 1970s.
“The research pioneered by the Heffter group has already provided breakthroughs in our understanding of the neurobiology and therapeutic potential of psychedelics,” says Geyer. “It is clear that further such research will result in currently unimagined treatments for human illness and a deeper understanding of human nature.”
Though the roots of this research go back decades at UC San Diego, the seeds of the PHRI began with a 2016 accident in the desert involving UC San Diego researcherAlbert Yu-Min Lin. A Qualcomm Institute research scientist and National Geographic Explorer, Lin lost his lower leg in that accident. Afterwards, he experienced debilitating phantom-limb pain, the sensation of pain seeming to come from the missing limb.
“After losing my leg,” says Lin, “I faced two immediate challenges. The first was rebuilding mobility, which could be done with prosthetics. The second was remapping my mind to let go of extreme pain that seemed to come from a body part that was no longer physically there. Luckily for me, the authority on the topic of phantom pain happened to be a UC San Diego faculty member, V.S. Ramachandran.”
Pioneering method, neuroplasticity
While Mirror Visual Feedback—the method pioneered by Ramachandran, distinguished professor of psychology and neurosciences, for treating phantom-limb pain—provided temporary relief, Lin observed that “when the mirror was removed the pain came rushing back, as if my mind just wouldn’t let it go.”
But psilocybin provided the profound relief he sought. A 2018 case study published in Neurocase, co-authored by Ramachandran, Chaipat Chunharas, Zeve Marcus and Furnish, documents Lin’s experience: a single session with psilocybin resulted in immediate, persistent and profound reduction in what had been debilitating post-trauma pain caused by an amputation.
“Freeing myself of the pain gave me back my life,” says Lin, who is the director of the Center for Human Frontiers based at the Qualcomm Institute.
But the use of psilocybin to treat phantom limb pain has not been researched in a controlled, rigorous way. Some studies in Japan in the 1970s used LSD with phantom-limb sufferers, with small but suggestive results.
Recent studies have shown that exposure to psychedelic drugs promotes neuroplasticity. Based on those existing findings, psilocybin may be effective against phantom limb pain because it causes new functional brain connections and pathways to form in brain regions supporting body self-image and the experience of pain. On the other hand, it could be that the profound psychedelic experience facilitates a “restart mechanism” if you will, that modulates the feeling of pain, says Fadel Zeidan, PHRI member, associate director for research at the UC San Diego Center for Mindfulness and assistant professor of anesthesiology.
Mindfulness of pain management
There is intriguing overlap with the research of Zeidan, who works to understand the effects of mindfulness meditation as a treatment for pain. His studies show that mindfulness reduces pain through multiple, unique brain processes that are distinct from placebo and other pain-relieving techniques. Recent research demonstrates that psychedelics produce states of mind and brain connectivity that are similar to those of experienced meditators, and that the two—psychedelics and mindfulness—are mutually supportive. Zeidan says that mindfulness meditation practice also promotes a “restart button” but one that you can press in a moment-to-moment fashion.
Non-opioid treatments for pain conditions—including cluster headache, complex regional pain syndrome, phantom-limb pain, tinnitus and other forms of chronic pain—could mean radical improvements for the more than 100 million sufferers in the United States alone, as estimated by the Centers for Disease Control and Prevention.
Future studies
According to the research team, these studies will provide a better understanding of how psychedelics can be used to treat pain, the mechanisms of action by which they produce their effects and how these phenomena illuminate new aspects of the healthy functioning of the brain. Such advances will help guide how the healthcare system can adapt to best deliver these radically different modes of intervention, all in the context of UC San Diego’s world-class health and neuroscience research communities.
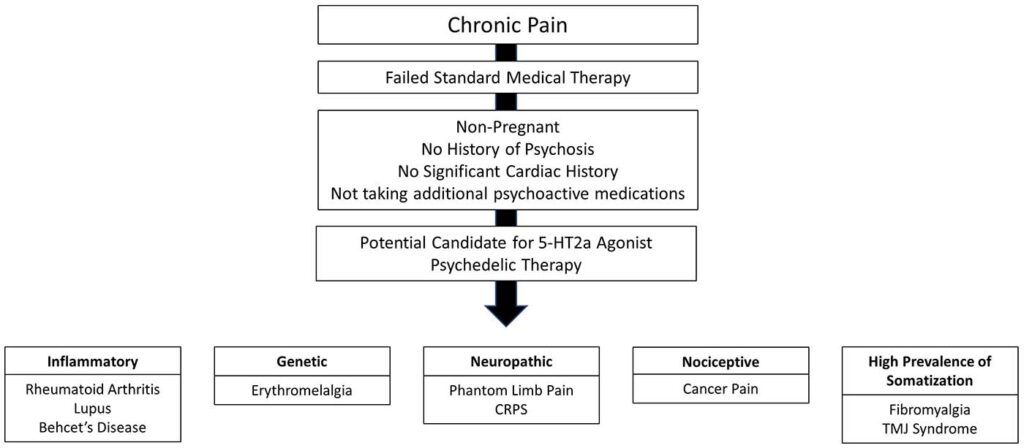
Proposed Screening and Approach for Future Study of Psychedelics and Chronic Pain
“Pain is a very tricky thing,” Lin says. “It can be entirely consuming to those who bear it. But my experience with pain opened a window into the power within the mind to do extraordinary things—to shift the perspective of pain, to potentially remap it away—and if that can help others it was all worth it.”
PHRI fosters further novel basic and clinical research on the use of psychedelics for the treatment of pain and potentially other syndromes. The interdisciplinary team is currently planning the first pilot study of the potential effect of psilocybin on phantom-limb pain, to be followed by future clinical trials and brain imaging research.
Article from – UC San Diego
STUDY: A MICRODOSE OF LSD COULD ALTER A FUNDAMENTAL HUMAN EXPERIENCE
“Anyone on any of these doses could sit behind a computer and do their work.”
IN LARGE DOSES, LYSERGIC ACID DIETHYLAMIDE (LSD) can repair damaged neurons in the brain, and reveal new ways of seeing the world. In small doses, microdosers chase the effects of the drug on creativity or mood, without the full psychedelic experience.
However, a new study suggests that even a microdose might be able to change a powerful human sensation: pain.
Microdoses of LSD increased pain tolerance and decreased ratings of painfulness and unpleasantness. Here, a microdose was defined as about 20 micrograms.
Twenty-fourcollege students were asked to plunge their hands into frigid 37-degree water and see how long they could handle the chill. Compared to a placebo, students on 20 micrograms of LSD could keep their hands in cold water about 20 percent longer and had lower ratings of unpleasantness and painfulness.
Greater increases in pain tolerance were “comparable” to what you might see with traditional pain-management drugs, like oxycodone or morphine during that same task, the authors note.
WHAT PART OF THE COVID-19 PANDEMIC DO YOU THINK CAUSES THE MOST CONFUSION? WE WANT TO KNOW. TAKE THE INVERSE READER SURVEY.
The study was published Monday in The Journal of Psychopharmacology, and was partially supported by the Beckley Foundation, a non-profit that researches psychoactive substances and advocates for “evidence-based changes” in global drug policy.
The study’s first author, Johannes Ramaekers, a professor at Maastricht University, suggests LSD could one day be an alternative to opioids, which are highly addictive.
“That would be of interest,” he tells Inverse. “To see if low doses of LSD could actually replace an opioid and at least reduce the addiction potential, because LSD has no addiction potential.”
While LSD does come with certain risks — a “bad trip” can lead to unpredictable behavior, it can possibly exacerbate certain psychotic disorders, and it’s not recommended for people with severe cardiovascular disease — it does not entail physical dependence or cause withdrawal. People can become tolerant to LSD over time, meaning that they’ll need higher doses to get the same effects.
It also exhibits very low physiological toxicity, even at very high doses. Taken together, its qualities make it an attractive alternative to pharmaceutical drugs to some scientists.
MICRODOSING AND PAIN MANAGEMENT – Research on the therapeutic potential of psychedelics is resurging after a drought between the 1970s and the 2000s. Ramaekers attributes the slowdown to the war on drugs. In 1970, psychedelics were placed into the most tightly regulated group (Schedule I) of The Controlled Substances Act).
Before the research landscape dried up, an influential study was conducted in 1964 on terminally ill patients who were suffering from extreme pain. They received LSD, and two opioids: meperidine and dihydromorphinone. LSD tended to produce longer and more powerful dampening of pain than the other drugs. The drawback was that the doses were so high, that the patients also experienced a psychedelic state.
“When those patients were asked, the next day or the next week, if they would like to have another dose to treat pain, there was a significant amount of patients that said, ‘no thank you,’ because of the strong, psychedelic experience,” Ramaekers says.
In this new study, Ramaekers and his colleagues tried to get that dosage just right: enough to improve pain tolerance, not enough to cause hallucinations.
The team tested three different dosages of LSD: 5 micrograms, 10 micrograms, and 20 micrograms.
“Anyone on any of these doses could sit behind a computer and do their work,” Ramaeker says.
At five micrograms, the team found no significant differences in how long people could withstand the water challenge. At ten micrograms, they saw a small difference that approached significance, but random chance still couldn’t be ruled out.
That 20 microgram dose was enough to produce significant effects on pain.
However, 20 is on the high-end of a microdose. You would be aware that you took a dose of LSD, says Ramaeker. Patients seemed to have more positive moods and were more attentive.
“It’s not really mind-altering or bringing hallucinations,” he says. “You may perceive colors, for example, as a little bit brighter.”
HOW DOES IT WORK? – This study wasn’t designed to illuminate why LSD seems to have an effect on pain, but Ramaekers proposes three ideas in the paper.
- LSD promotes “self-transcendence” that blunts the experience of pain. Psychedelics can cause “breakthrough experiences” that feel like entering another reality. As the paper puts it: “in essence: no self, no pain.”
- Microdoses were linked to increases in the patient’s blood pressure, and increases in blood pressure have been linked to increased pain tolerance before. However, as one 2013 study points out, this relationship may hold for acute pain (like a pinprick), but not chronic pain (that originates in the body).
- LSD can bind to two types of serotonin receptors that are present throughout the brain, body, and spinal cord, Ramaekers says. He suggests that “stimulation of these receptors inhibits the transduction of pain signals to your brain” but adds that there is still scant research on this in humans.
Ramaekers says it’s possible the full explanation involves all three hypotheticals. He’s less compelled by the transcendence idea because the psychedelic experiences reported by his patients were “almost nil” he says and feeling “dissociated” could only explain 6 percent of the variation in pain tolerance.
For now, the study demonstrates that it might be possible to benefit from the pain-reducing aspects of LSD without having to commit to the drug’s hallucinogenic side. In the future, Ramaekers hopes that we might be able to get a bit more specific with the dosage.
Microdosing may be the way forward, but just how “micro” that dose should be is up in the air.
Partial Abstract:
Methods: Twenty-four healthy volunteers received single doses of 5, 10 and 20μg LSD as well as placebo on separate occasions. A Cold Pressor Test was administered at 1.5 and 5h after treatment administration to assess pain tolerance to experimentally evoked pain. Ratings of dissociation and psychiatric symptoms as well as assessments of vital signs were included to monitor mental status as well as safety during treatments.
Results: LSD 20 μg significantly increased the time that participants were able to tolerate exposure to cold (3°C) water and decreased their subjective levels of experienced pain and unpleasantness. LSD elevated mean blood pressure within the normal range and slightly increased ratings of dissociation, anxiety and somatization.
Conclusion: The present study provides evidence of a protracted analgesic effect of LSD at a dose that is low enough to avoid a psychedelic experience. The present data warrant further research into the analgesic effects of low doses of LSD in patient populations.
Story from Inverse OnLine
Canadian Government Will Respond To Psychedelics Decriminalization Petition
Why are Shrooms Illegal?
It’s been almost 50 years since shrooms were banned internationally, but recent developments suggest that the days of prohibition are numbered.
James McClure – July 15, 2020
Magic mushrooms are illegal in nearly every country thanks to the Convention on Psychotropic Substances — an international treaty developed in 1971 by the United Nations to prohibit the production, distribution, and consumption of psilocybin mushrooms and other psychedelic substances. Since the Seventies, more than 180 countries have pledged support to the treaty.
But the United Nations doesn’t have the power or resources to police the streets in all of those countries, so the onus has been on each member state to develop its own laws to prohibit shrooms and other psychedelics.
Here’s how shrooms became illegal in America, the United Kingdom and the Netherlands.
Why are shrooms illegal in America?
The United States was one of the first countries to prohibit psilocybin, but thanks to the efforts of psychedelic researchers and grassroots advocates, America might also become one of the very first nations to knock down prohibition through local reform legislation and nationwide FDA approval of psilocybin in assisted psychotherapy.
America officially outlawed shrooms in 1968 through an amendment to the Food, Drug and Narcotics Act known as the Staggers-Dodd bill, which banned the possession of psilocybin (the main compound in shrooms) as well as psilocin (the compound that psilocybin metabolizes into after being ingested).
Psilocybin prohibition, however, wasn’t seriously enforced until the passage of the Controlled Substances Act (CSA) in 1971, which marked the beginning of America’s disastrous War on Drugs. Under the CSA, psilocybin and psilocin are listed alongside heroin as Schedule I drugs, meaning that they have a high potential for abuse and no accepted medical use—at least, according to the federal government.
Scientific research (both from present day clinical trials and pre-Drug War experimentation) and centuries of ritualistic use in indigenous communities, however, have proven otherwise. Classifying magic mushrooms as Schedule I defied the findings of psychedelic research from the 1950s through the 1970s, showing that mushrooms carried promise as a potential treatment for alcoholism, schizophrenia, autism, obsessive-compulsive disorder, depression, and other conditions.
Story from Double Blind
Group Calls for Canada to Decriminalize Drug Possession
– CBC News –
Two years after Justin Trudeau legalized cannabis, the Canadian Association of Chiefs of Police says arresting people for having small amounts of other drugs, such as cocaine and heroin, is “ineffective.”
As Canada continues to battle an opioid epidemic, the Canadian Association of Chiefs of Police is calling on federal lawmakers to decriminalize the possession of small amounts of illegal drugs for personal consumption.
CACP’s president, Chief Const. Adam Palmer, said it’s time to rethink how police and governments approach the use and abuse of illegal drugs in order to save lives.
“Arresting individuals for simple possession of illicit drugs has proven to be ineffective. It does not save lives,” Palmer said. “The CACP recognizes substance use and addiction as a public health issue. Being addicted to a controlled substance is not a crime and should not be treated as such.
“We recommend that Canada’s enforcement-based approach for possession be replaced with a health-care approach that diverts people from the criminal justice system.”
CACP is a non-profit that represents about 1,300 police chiefs from federal, First Nations, provincial, regional, transportation and military police services across the country.
Palmer said that, as an alternative to the criminal model, partnerships could be formed between social services, police, the health-care sector and governments to ensure drug users get access to the treatment they need.
The focus of police efforts, he said, should be on cracking down on drug trafficking and the illegal production and importation of drugs — a task the police are better suited to address.
Palmer said such a shift in policing would require changes at the federal level to the Controlled Drugs and Substances Act.
In 2018, the CACP tasked a committee with exploring the impacts on public safety and policing of moving toward decriminalization.
#defundthepolice
That report, delivered this month, concluded that substance abuse is a public health issue and that taking a public health approach to the problem would lead to lower rates of crime, overdoses and blood-borne diseases.
Palmer was asked about the #defundthepolice movement on social media and whether police forces in Canada are willing to see their funding diverted toward social services or health care.
He said that in Vancouver, where he serves as chief constable of the Vancouver Police Department, police are already looking the other way on cases of simple possession in order to focus resources on trafficking and production — so there may not be much money to divert.
Palmer did say he was willing to discuss the notion of redirecting police funding to other initiatives if all affected parties are consulted.
A statement from Minister of Health Patty Hajdu and Justice Minister David Lametti said they welcomed the “endorsement of a holistic approach” to dealing with the opioid crisis.
“We appreciate efforts made by law enforcement officers to consider alternative options to criminal charges for simple possession of illicit drugs in appropriate cases, and recognize the importance of reducing barriers to treatment, as well as integrated partnerships between law enforcement and health and social services,” the statement said.
The ministers went on to say that the federal government would continue to work with substance abuse experts, first responders and law enforcement to further their own public health approach to dealing with the opioid epidemic.
“Our government remains committed to advancing evidence-based responses to help reverse the trend of opioid overdose deaths and other substance-related harms in Canada.”
LSD. Good for your health?
This Canadian researcher says it just might be — if you take enough
By Omar Mosleh – Toronto Star – Edmonton Bureau
Friday, Feb. 28, 2020
EDMONTON—Looking for a healthy trip? It turns out a massive dose of LSD might — and let’s really stress might — be just what the doctor ordered.
You may have heard of microdosing: When people consume psychedelics, usually LSD or magic mushrooms, in miniscule quantities for purported cognitive and mental health benefits.
But what about macrodosing?
A University of British Columbia adjunct professor and researcher into psychedelic drugs co-authored a study which examines the impact of people overdosing on LSD. It found that for three people, who consumed extremely large quantities of the drug —in one case as much as 550 times a normal recreational dose — didn’t have any long-term adverse effects and can actually have demonstrable health benefits.
But before you get too excited about trading in your acid reflux for acid flashbacks, the benefits are mostly for mental health conditions such as post-traumatic stress disorder, depression, anxiety and substance-use disorder.
But in one of three cases examined in the report, a woman reported the LSD overdose helped her with physical pain in her foot that had bothered her for roughly 20 years.
The report cautions that the information is “novel” as no clinical trial research has been done with such quantities. The data is anecdotal, no blood or urine samples were available and the exact dosages were approximate.
Psychedelics are a class of drugs that produce mental, visual and auditory changes. The word has replaced the outdated term hallucinogen. LSD is one of the most powerful psychedelics and is one of the few recreational drugs measured in micrograms (one millionth of a gram).
“It wouldn’t pass ethics review because they would argue it’s not safe,” Haden explained.
So researchers decided to look at accidental overdoses. The people in the study reported taking anywhere from 1,000 micrograms to 55 milligrams, which would be the equivalent of a 550 times a normal recreational dose (about 100 micrograms).
In the first case report, a 15-year-old girl with bipolar disorder accidently consumed 1,000 micrograms of LSD instead of 100 due to a decimal point error when the supplier was diluting liquid LSD into a glass of water. Observers reported erratic behavior for nearly seven hours, including her lying in a fetal position with her arms and fists clenched and seizures.
She was transported to a hospital where she was treated for the seizure. The next day, something miraculous happened.
The girl’s father reportedly entered the hospital room and the girl told him “it’s over.” But she wasn’t referring to the LSD trip – she meant her bipolar disorder was cured.
“This case report documents a significant improvement in mood symptoms, including reductions in mania with psychotic features, following an accidental LSD overdose, changes that have been sustained for almost 20 years,” the report states.
The second case examines a 26-year-old woman who accidently consumed 500 microgram while two weeks pregnant. Her son is now 18 years old and healthy.
“The second case documents how an accidental overdose of LSD early in the first trimester of pregnancy did not negatively affect the course of the pregnancy or have …other negative developmental effects on the child.”
The report says she “blacked out” for roughly 12 hours and was vomiting frequently. But after the vomiting episode she reported feeling “pleasantly high.”
The next day, foot pain she had experienced since her early 20s as a result of Lyme disease was gone. She had been prescribed morphine for 10 years to contend with the pain.
“She continued microdosing LSD with daily morphine until January 2018, when she stopped the morphine and all other pain medications, as she believed that her pain was significantly reduced enough that pain medications were unnecessary,” the report states.
However, it states that she did experience an increase in anxiety, depression and social withdrawal after discontinuing morphine.
The report ultimately concludes that there appear to be “unpredictable, positive” effects ranging from improvements in mental illness to reduction in physical pain.
Haden said no one really knows why this is the case.
But he believes it has something to do with psychedelics allowing people to tap into what he calls “unconscious material,” our subconscious emotions and memories that we’re not aware of.
“We live our lives largely unconsciously,” Haden explains, using the example of when you’re driving to work and thinking about what you’ll make for dinner rather than your foot on the gas pedal.
When a person experiences trauma, it’s stored deep in the brain, Haden said.
“That stuff gets buried and we don’t have access to it. … And you can’t contain it or control it because it’s in your unconscious mind,” he said.
Enter psychedelics. Haden says this class of drugs has the ability to tap into the unconscious thoughts and feelings so they can be analyzed and addressed in a clinical manner. It’s part of a process he calls “psychedelic healing.”
It’s still unclear why these people reported health benefits from overdosing on LSD.
“My speculation is that it has something to do with new neural pathways,” Haden said, or an ability to effectively reset parts of the brain.
He hopes the report will encourage more clinical studies into the potential benefits of psychedelic drugs. He wants to see them eventually legalized and offered as a service by “psychedelic supervisors,” who could train people on how to use the drugs safely and offer therapy for conditions like depression and anxiety.
“The more we can observe, either anecdotally or through the lens of trial research, the benefits of psychedelics … if public opinion says these are not taboo anymore, these are something we can actually look at in terms of (therapy).”
Story from The Toronto Star
Ontario eyes OK’ing cannabis lounges, cafes
Toronto Sun – February 10, 2020
Premier Doug Ford’s government said it is considering allowing cannabis lounges and cafes as it moves toward an open market for pot in the province, and is asking the public to weigh in on the proposal.
The government said Monday it will consult on the possibility of so-called “consumption venues” as well as special occasion permits that would apply to outdoor festivals and concerts.
In a posting on its regulatory registry, which closes March 10, the government said it wants to hear from the public before committing to any direction, and gave no timeline to make changes.
“We are asking Ontarians to share their feedback as we explore certain expanded cannabis-related business opportunities as part of our responsible approach to protecting families and communities,” Attorney General Doug Downey said in a statement. “What we hear from the public and expert groups will help to inform possible next steps.”
The Progressive Conservative government has said its ultimate goal is an open cannabis market, but a supply shortage forced it to start with a limited lottery system for retail licences shortly after marijuana was legalized in 2018.
In December, the province announced it was doing away with the controversial lottery system that was criticized as a cumbersome process preventing the province from staying competitive.
The Alcohol and Gaming Commission of Ontario said it has received more than 700 applications for retail operator licences since the system was scrapped on Jan. 1.
Downey said allowing greater competition in the retail sector will help combat the black market.
“Ontario continues to take a responsible approach to cannabis retail sales across Ontario, allowing private sector businesses to build a safe and convenient retail system to combat the illegal market while keeping our kids and communities safe,” he said Monday.
Robyn Rabinovich, a business strategy lead at strategy firm Hill+Knowlton who advises cannabis sector clients, said the proposal could legitimately help the Tories advance their goal of combating the black market by giving consumers another option to buy legal cannabis.
“There’s a lot of opportunities for businesses like cafes and restaurants to start making steps into the cannabis industry,” she said. “This could ensure it’s done in a regulated and safe way.”
Rabinovich said special occasion permits would give the government a chance to further regulate cannabis use in some public spaces and acknowledge the reality of post-legalization Ontario.
“If you’re at a music festival and you look around, it’s clear that cannabis is being consumed,” she said. “If they were to organize it and regulate it, it may not be in the presence of minors or be causing any harm to others at the event.”
Ontario’s previous Liberal government was exploring the idea of cannabis consumption lounges in 2018, announcing consultations just months before it was defeated in the most recent provincial election.
Story from The Toronto Sun
Famed investor Michael Novogratz said psychedelics will be the next ‘short-term bubble’ after cannabis — and predicts Compass Pathways will go public this year
Fresh News Now – January 29, 2020
Investor and crypto evangelist Michael Novogratz says medicine derived from psychedelic drugs will be the next “short-term” bubble at a hedge-fund conference in Florida.
Novogratz backed Compass Pathways, a UK-based startup working on bringing drugs derived from psilocybin — the active ingredient in magic mushrooms — to market.
He said he expects the startup to go public later this year.
Famed investor Michael Novogratz made a big bet on psychedelics — one he expects will pay off soon.
“I’m positive this will be the next short-term bubble because it’s such a positive story,” the former Goldman Sachs partner, hedge fund manager, and cryptocurrency evangelist said at the Context Summits conference in the Fontainebleau Hotel on Miami’s South Beach.
To that end, Novogratz has backed UK-based Compass Pathways, a biotech working on bringing drugs derived from psilocybin — the active ingredient in magic mushrooms — to market.
“There’s an awakening that these old drugs, these old plants, magic mushrooms or ayahuasca or the Iboga root from Africa have real positive medicinal qualities,” Novogratz said.
Novogratz predicted the company will go public “before the end of the year.”
A spokesperson for Compass Pathways told Business Insider that “we are always looking at options to ensure continued growth and funding,” but that the company doesn’t comment on “speculation.”
The company raised a $32 million Series A funding round in October of 2018, per the data provider Crunchbase.
Psychedelic drugs hold promise for a range of ailments, from mental health to obesity
While the science is in its early stages, top-notch institutions like Johns Hopkins have developed programs to study the effects of psychedelic drugs including psilocybin, MDMA, ketamine, and others on a range of ailments including depression, obesity, Alzheimer’s, and even smoking cessation.
Story from Fresh News Now
Move over, pot: Psychedelic drug companies gear up to list on Canadian stock exchanges
Companies developing treatments from LSD, ketamine and the active ingredient in magic mushrooms are finding interest from investors, including Kevin O’Leary
The first companies developing medical treatments from psychedelic drugs like LSD, ketamine and the active ingredient in magic mushrooms are gearing up to list on Canadian stock exchanges.
Mind Medicine Inc., which is undertaking clinical trials of psychedelic-based drugs, intends to list on Toronto’s NEO Exchange by the first week of March, said JR Rahn, the company’s co-founder and director. A NEO spokesman confirmed the listing, which is pending final approvals.
The company plans to list via a reverse takeover under the ticker MMED. It’s not yet generating revenue and is targeting a valuation of approximately US$50 million, Rahn said. Mind Medicine counts former Canopy Growth Corp. co-chief executive officer Bruce Linton as a director and Shark Tank star Kevin O’Leary as an investor.
“Our ambition is to be one of the first publicly listed neuro-pharmaceutical companies developing psychedelic medicines,” Rahn said in a phone interview.
CLINICAL TRIALS
For those who are still getting used to legal marijuana, the idea of publicly traded companies working with psychedelic drugs like MDMA and psilocybin, which is derived from magic mushrooms, may sound a bit out there.
In late 2018, the FDA gave “breakthrough therapy” status to a psilocybin treatment developed by London-based Compass Pathways Ltd. for clinical depression, expediting the development process.
Meanwhile, Toronto-based Mind Medicine is preparing a Phase 2 clinical trial into the use of a psychedelic called ibogaine to treat opioid addiction, which will be conducted in New York and governed by the FDA.
Compass Pathways declined to comment on whether it’s planning a public listing, but the company is “always looking at options to ensure continued growth and funding,” chief communications officer Tracy Cheung said in an email.
The Canadian Securities Exchange, which has become the go-to bourse for U.S. cannabis companies that can’t list in their home country, is also expecting listings from psychedelic drug companies in 2020.
The FDA has “given clearance for a variety of trials at this point and it looks like they are going to be expanding that framework,” said Richard Carleton, CEO of the Canadian Securities Exchange. “If that is the case then I’m certain we’ll see our first issuers probably before the middle of the year.”
INSTITUTIONAL CAPITAL
There’s growing investor interest in psychedelics, said Ronan Levy, executive chairman of Field Trip Psychedelics Inc. Field Trip is building a network of clinics focused on ketamine-enhanced psychotherapy, with the first one opening in Toronto next month and others planned for New York City and Los Angeles. It’s also conducting research into psilocybin at the University of the West Indies in Jamaica.
Last week, Field Trip closed a Series A financing round that raised US$8.5 million from a variety of investors including cannabis-focused asset manager Silver Spike Capital and Harris Fricker, the former CEO of GMP Capital Inc., which helped a number of marijuana companies go public.
The funding round attracted interest from all over the world, including “some very large Silicon Valley tech investors and entrepreneurs,” Levy said.
Field Trip is considering a public listing, although Levy also sees further opportunities to raise private funding, he said. Unlike cannabis, which remains federally illegal in the U.S., the work psychedelic companies are doing is legal. This creates “greater opportunity to access growth capital from private investors in the U.S. who may not touch cannabis,” he said.
It also sets the industry apart from cannabis, which has seen stock prices collapse amid slower-than-expected sales in Canada and ongoing federal illegality in the U.S.
“I think that the psychedelics industry could be much bigger than the cannabis industry because it’s going to attract institutional capital and already is starting to,” Rahn said. “It’s also going to be a more concentrated space because the barriers to entry are much higher.”
Story from – Bloomberg News
DC election board allows proposal to decriminalize psychedelics
WASHINGTON (AP) — Supporters of a proposal to decriminalize the use of certain psychedelic plants and fungi are one step closer to putting the measure on the ballot in the District of Columbia.
The D.C. Board of Elections agreed Wednesday to allow the proposal to be put up for a citywide vote in November, news outlets reported.
The initiative aims to place the use of psychedelic plants, often referred to as magic mushrooms, among the lowest priorities for law enforcement.
The proposal now moves to a challenge period in which proponents must gather 25,000 signatures to officially place the measure on the ballot. The signatures need to be obtained by July 1, news outlets reported.
Melissa Lavasani proposed the initiative. She told news outlets that she suffered from depression after giving birth to her second child. She said psychedelic mushrooms helped ease her condition. Wyly Gray, a Marine, told The Washington Post that psychedelics helped him deal with post-traumatic stress after he returned home from serving in Afghanistan.
Copyright © 2020 The Associated Press. All rights reserved. This material may not be published, broadcast, written or redistributed.
Story from The Associated Press – WTOP
Five things to know about munching on cannabis edibles
Vancouver Coastal Health is sharing a few reminders for those munching on cannabis goodies for the first time.
POSTMEDIA NEWS/Vancouver Sun – February 7, 2020
Curious about cannabis but not sure about smoking or vaping it? You could always try edibles.
With edibles now available through licensed dispensaries and more products expected throughout 2020, Vancouver Coastal Health is sharing a few reminders for those munching on cannabis goodies for the first time.
“We’ve seen for many years that it’s easy for people, especially those who have less experience with cannabis, to consume more cannabis than they mean to with edibles,” said Dr. Mark Lysyshyn, medical health officer with VCH.
“Because the psychoactive effects of cannabis are a little different and take longer to kick in when digested, people often make the mistake of taking additional doses. But once the effects kick in, they can find themselves dealing with unpleasant sensations and feeling more impaired than they expected to be.”
Here are five things to know about munching on cannabis edibles.
Start small.
If you’re new to edibles, it’s best to start with a small dose and see how your body responds before increasing the amount you eat. Edibles can often pack a bigger punch than smoking cannabis so until you know what works for you, start small. Be sure to always check the THC levels in your edible and be mindful that a dose of 2.5 to 5 mg of THC is often enough for many. Cut an edible into halves or quarters if needed.
Wait and see.
Edibles might take a bit longer to kick in than smoking so be sure to wait and see before eating more. Be patient — wait at least an hour to feel the full effect. Ingesting edibles on a full or empty stomach can also affect the amount of time it takes to feel the effects. Plan ahead and be sure you’ll be in a comfortable place approximately an hour after ingesting your edible.
Avoid too much and avoid mixing.
Avoid eating too much cannabis, using strong extracts or mixing it with alcohol, as this can cause anxiety, vomiting and fainting for those unfamiliar with how their body will respond. Eating a meal before ingesting an edible can help moderate the intensity of any possible negative effects. In short, keep it simple until you know what to expect or what works for your system.
Don’t drive if impaired.
Health officials recommend not driving or engaging in other potentially dangerous activities when enjoying edibles, as cannabis can impair co-ordination, reaction time and other cognitive abilities. While the time it takes for the effects to wear off can vary from person to person, experts recommend waiting at least six hours after ingesting cannabis to drive.
Don’t panic.
This one will be hard but do your best. If you start to feel the effects and it’s not what you expected or you think you’re too high, don’t panic. Drink some water, eat something and find a safe place where you can get cosy and comfortable and wait it out. Ground yourself by laying down and taking a nap if you need to, or keep yourself near a washroom or bin if you think you might vomit. The effects should wear off between two to eight hours.
Other things to remember when ingesting cannabis edibles:
• Label and store all cannabis securely, particularly when many edibles look like regular food or candy. Store cannabis products away from regular food products and ensure they are out of reach from children and pets, to prevent accidental consumption.
• Be sure to obtain your cannabis from a legal source or a source that you trust.
• If you or someone you know doesn’t feel well after consuming cannabis, call the B.C. Poison Control Centre at 1-800-567-8911 or 604-682-5050. You can also call 911 or visit your local hospital emergency department.
Story from Vancouver Sun
Ontario to ban flavoured vaping products from being sold in convenience stores
Carly Weeks – Health Reporter – February 3, 2020
The Ontario government is moving to ban most flavoured vaping products from convenience stores and gas stations and cap nicotine levels in a bid to prevent young people from using e-cigarettes.
Health Minister Christine Elliott will present proposed regulatory changes to provincial cabinet members in the coming days.
The new rules won’t apply to specialty adult-only vape shops, which require proof of age to make a purchase, and sell only vaping products. Those stores will still be able to sell a variety of flavoured products and e-cigarettes with higher nicotine content.
Governments across Canada are wrestling with how to address youth vaping rates, which have soared in recent years. In December, the federal government announced it would ban most forms of e-cigarette advertising that young people could see, including on social media, and it has promised new flavour restrictions this year. The government has also suggested it might cap nicotine levels in vaping products.
Under the current federal law, companies cannot promote e-cigarette flavours that could appeal to youth, such as candy, dessert or soft drink flavours.
Health Canada recently singled out specialty vape shops as having “unacceptable” levels of non-compliance for federal vaping laws. In a December letter to retailers, the department said more than 80 per cent of specialty vape shops that inspectors visited last year were selling and promoting products in violation of federal law. The most common infractions were promoting flavours that appeal to young people and using testimonials or endorsements in product promotions. Under the law, testimonials or endorsements refers to using people, characters or animals in ads.
Only two other provinces – Nova Scotia and PEI – have moved forward with flavour bans. As of April 1, no retailer in Nova Scotia will be permitted to sell any flavoured vaping product other than tobacco or unflavoured e-cigarettes. Specialty adult-only stores will not be exempt. PEI is in the midst of consultations on vaping restrictions, and the province’s Health Minister has promised to ban flavoured products in the coming months.
Travis Kann, a spokesman for Ms. Elliott, said the province is finalizing its new policies, and will “take a balanced approach that keeps Ontario children and youth safe while also avoiding fuelling an underground market for unsafe vapour products.”
Under Ontario’s plan, convenience stores and gas stations would no longer be permitted to sell any flavoured e-cigarettes, with the exception of tobacco and menthol. The government also wants to limit the nicotine content of any vaping product sold by those retailers to 20 milligrams a millilitre, which is the same level the B.C. government has proposed.
Some vaping products now on the market come with nicotine concentrations as high as 59 milligrams a millilitre.
Ontario’s proposed changes would affect the big-name e-cigarette brands that sell primarily in convenience stores, such as Juul and Vype. Both companies sell single-use e-cigarette pods that come in flavours such as cucumber, mango, strawberry and vanilla. Earlier this month, Juul Labs Canada announced it would temporarily halt production of all of its e-cigarette flavours in Canada except mint and tobacco. The company said it would sell its existing stock of flavours, and manufacture no more until the federal government announces its new rules.
Darryl Tempest, executive director of the Canadian Vaping Association, which represents specialty adult-only vape shops, said he supports Ontario’s proposals. Restricting the products sold in convenience stores can help discourage youth uptake, but allowing the full spectrum of products in specialty shops helps provide options for adult smokers looking for a less harmful alternative, he said.
But Dave Bryans, chief executive officer of the Ontario Convenience Stores Association, said the changes put the interests of specialty vape shops before those of convenience-store retailers. Mr. Bryans said he had a meeting with Ms. Elliott recently in which the association asked the province to adopt industry-wide restrictions such as banning the display of vaping products in all retail environments instead of restricting flavours.
“My fear is that the government’s not taking its time in understanding this,” Mr. Bryans said.
Rob Cunningham, senior policy analyst with the Canadian Cancer Society, said restricting where flavoured e-cigarettes are sold could help reduce access and make laws easier to enforce. But he added that it would be better if Ontario applied its proposed new rules to the entire industry.
“What Ontario’s doing could be further strengthened with comprehensive restrictions on flavours for all stores, as well as nicotine levels,” Mr. Cunningham said.
Story from The Globe and Mail
The Trouble with Crime Statistics
It’s surprisingly hard to say what makes crime go up or down.
Cannabis edibles now available online through Ontario Cannabis Store
Thurday, January 16, 2020
TORONTO – Ontario cannabis shoppers scooped up thousands of edibles and vape products within an hour of them going on sale for the first time on the Ontario Cannabis Store’s website.The online retailer experienced 2,000 transactions on Thursday in the hour after 70 products — cannabis-infused chocolates, cookies, soft chews, mints, tea and vapes — were made available at 9 a.m. local time.Some products sold out within a half-hour, said the cannabis distributor’s spokesperson Daffyd Roderick.
“At 8:59 a.m., we had 3,000 people in the lobby hitting refresh, waiting to get online, so there was obviously some excitement in the marketplace,” he said.“We were sold out of soft chew products within 25 minutes.”
The rollout is part of Cannabis 2.0, where the country is allowing a second wave of products like edibles, extracts and topicals to hit the market following the October 2018 legalization of cannabis in Canada.
The frenzied pace of sales online Thursday comes after the products first appeared on store shelves last week. Such items were approved for sale in Canada in mid-December, but several provinces, including Ontario, delayed their rollout.
When the OCS website was first launched and the first round of cannabis products went on sale in 2018, Roderick said the site experienced “high demand,” causing online deliveries to take as long as five days to arrive. Ontario Premier Doug Ford said in the first 24 hours the OCS processed 38,000 orders.
Roderick said the online debut of the edible and vape products went well, but acknowledged that there were “a few bumps.”
“Because there were so many people simultaneously refreshing, their page would drop and then they would hit refresh a couple times and they would get back,” he said.
“It’s similar when you’re buying concert tickets or anything else where everyone is online trying to do the same thing at the exact same moment, so we did face some challenges but that’s completely sorted itself out now.”
When shoppers Thursday did make it through to the site, which was down between 12:01 a.m. and 9 a.m. to prepare for the launch, Roderick said they were most interested in soft chews.
Several packs were priced for between $6.65 and $12.35 and came in flavours like raspberry vanilla, peach mango, pineapple orange, apple green tea and grapefruit hibiscus.
Roderick figured their popularity stemmed from soft chews having a “convenience factor” and because “not everybody loves chocolate.”
There were only three kinds of chocolate left for shoppers by noon, when The Canadian Press reviewed the website.
Roderick would not share when more stock will arrive or how much of each product was available for sale, but said its allotment is equal to physical stores and the distributor has a limited supply it has been provided with by licensed producers.
“We know that they’re doing their best to ramp up their production capacity and like everyone else, we’re waiting and watching for when those products are going to come,” he said. “The producers are very interested in getting these products to market, so they’re working as quickly as they can.”
The OCS expects cannabis topicals, concentrates and beverages to be sold in the coming months.
This report by The Canadian Press was first published Jan. 16, 2020.
Story from The Canadian Press
Ontario Cannabis Store to begin selling edibles online Thursday
By Shayla Vize – January 16, 2020
The Ontario Cannabis Store (OCS) will begin selling 70 new items online Thursday including cannabis edibles.
The new items have been tested by Health Canada and will be available for purchase starting at 9 a.m.
Last Monday, the OCS began selling the items in-store.
OCS President Cal Bricker says he is hoping the expansion of products will help combat sales of cannabis through the underground market.
Story from CHCH
Ontario to scrap pot shop lottery system, will open more stores in new year
The Tories had initially said there could be up to 1,000 cannabis stores in the province
Puff in Public! Ontario Allows Adults to Smoke Weed Anywhere Tobacco Is Allowed
Green Party would decriminalize all drug possession if elected
Opioid crisis needs a health-care approach, party leader Elizabeth May says
Cannabis smokers get more bong for their buck at bud-and-breakfasts with a different vibe
But the room isn’t just for her enjoyment. It’s seen a handful of visitors since Roach, the owner of the nearby cannabis-centric Hotbox Café, listed it about four months ago on rental website Airbnb as a “funky 420” space.
Critics say sticker shock at cannabis prices will push customers back to the black market
Matt Daisley said his first visit to a legal cannabis retail outlet in St. Catharines, Ont. this week ended without a purchase after he heard the prices and almost had a heart attack.
“I knew immediately that I would not leave the black market,” he said. “There’s no chance.”
The 60-year-old is a longtime cannabis user and visited The Niagara Herbalist to check out its government-approved marijuana options after the store officially opened Monday. But, when he went up to the counter to buy 3.5 grams of MK Ultra, he said he was asked to pay $45 plus tax and was rocked by sticker shock.
His complaint about the comparatively high price of legal pot was a routinely heard one from customers during the first week of legal retail sales in the province.
The Ontario Cannabis Store says its products are priced to compete with the black market but critics, including a professor at Brock University, say buying illegally offers those willing to take the risk significant savings, meaning legal prices will have to drop if they want to bring in more customers and cut out the black market. Police have also pointed to affordable pricing as an important tool to combat organized crime’s involvement in the drug trade.
Daisley claims he could buy as much as seven grams of MK Ultra for about $40 from an illicit vendor online.
That’s what he plans to keep on doing, he told CBC News, adding the laws around black market weed and the consequences for purchasing it are still vague so he’s willing to go public about his concerns in hopes the government and retailers will listen.
“I’m making a conscious choice to use the black market rather as opposed to the legal market. I understand the ramifications of that,” he said. “[But] what can they really do to a 60-year-old guy who’s smoked for the better part of 25 years every day?”
The price has to be right to defeat organized crime
The laws around cannabis use in Canada are still evolving and need to be tested in court, so there’s “some validity” to Daisley’s point, according to Joe Couto, a spokesperson for the Ontario Association of Chiefs of Police.
He added police aren’t naive enough to think legalization means the black market will die overnight — especially if there’s a big price difference.
“I don’t know if the price is right,” he said, adding law enforcement officials have to trust the government to make those decisions.
“We’ve always recommended to them that if you don’t price the product at a market price obviously it does create pressures and black market activity.”
Cannabis has long been a source of income for organized crime in Canada, explained Couto, so police are concerned they’ll take advantage of the early stages of legalization to turn a profit.
“If we’re going to eliminate cannabis as a potential source to fuel criminal activities … obviously ensuring the product is accessible and is priced right is really important.”
Daisley said up his experience at The Niagara Herbalist was largely positive until he went up to the counter and found out how much he would be charged.
He said he’d prefer to purchase cannabis legally, but believes that, like him, the buying decisions for most cannabis consumers will be dollar-driven and the price tags raise questions about markup that will keep people out of legal stores.
Like comparing a ‘fine wine’ to moonshine
Hamilton-based cannabis consultant, Olivia Brown, disagrees. She says the quality legal outlets offer is worth paying for.
“I wouldn’t compare a $180 bottle of fine wine to moonshine just because it’s cheaper.”
Brown said the prices charged by private legal retailers are generally similar to those posted on the OCS online store, but added that, like gas stations, consumers could see a slight difference of $1-3 depending on which shop they’re in.
Still, Brown said she hears people complaining about the price of legal pot every day.
She agreed black market prices are lower than their legal counterparts, but pointed out government regulated cannabis is a big business that has to pay many employees and meet all sorts of standards.
“It’s very highly regulated, it’s very expensive to maintain and has huge operating costs.”
Brown also said cannabis is a product where you get what you pay for — there’s a reason the black market is so much more affordable.
“It’s probably grown outside by someone who may not know what they’re doing, they could be using pesticides or have all kinds of bugs or whatever,” she explained. “These people aren’t understanding the difference between really fantastic, lab-tested quality-grown, labeled, packaged beautiful products.”
Offering more options for purchasing those high-quality, legal products is the only way to make sure black market usage is really curbed, according to Hamilton Mayor Fred Eisenberger.
The mayor’s comments came in response to recent criticism leveled at police and officials in Hamilton by Premier Doug Ford who said failure to shut down illegal dispensaries in the city was his “biggest frustration” when it came to cannabis legalization in Ontario.
OCS says legal cannabis is ‘competitively priced’
In a statement to CBC News a spokesperson explained the OCS buys its cannabis from producers licensed by Health Canada then sets a retail price, which can go up or down based on factors including market conditions, supply and the purchase price from producers.
“Armstong”- Michael Armstong, Brock University
Legal products are tested and “competitively priced” with the illegal market in mind, the statement read.
The spokesperson added the pricing structure for retailers allows them to set their own prices that “reflect their individual business models.”
On the OCS website MK Ultra, the same strain Daisley said he was trying to buy is listed from $12.85 / gram or $39.95 for 3.5 grams — though it does not appear to be currently available.
Customers need a discount option like ‘No Name’ weed
In the short term the limited number of stores in Ontario mean each location should be able to draw plenty of customers, but an associate professor at Brock University said big changes have to happen if government wants to compete for the long haul.
Michael Armstrong teaches at the Goodman School of Business and has been watching Canada’s foray into legalization closely.
“Absolutely the black market enjoys a big price advantage,” he said, pointing to a Statistics Canada report for the last quarter of 2018 showing the average price paid for legal, dried cannabis was $9.70, compared to $6.51 its illegal counterpart.
At some point, the pool of customers willing to pay up to 50 per cent more for a legal product will dry up and the stores will have to start appealing to people who are only willing to cough up something in the range of 25 cents more per gram.
Armstrong said the government has to be ready and offered a few suggestions for how to cut costs.
The first is lowering the overall production cost by going large scale, automating the process or moving growing operations outdoors. When those saving lead to a drop in price, the professor said provinces should lower their wholesale process so retailers can also sell for less.
Another obstacle is the federal government’s excise tax structure. Armstrong said excise tax currently varies by province, but the default is about $1 per gram minimum, which makes it tough to keep up with the black market.
“Even if a producer can make it really cheaply and a retailer is willing to sell it for a low price, that dollar is a big chunk.”
He argues the government should drop that minimum and just set the tax at 10 per cent.
Under that model a premium product could pay around $2 a gram in tax and an averageproducts could pay around $1, but retailers could offer a discount brand.
“Eventually the retail stores need to be able to sell something like a No Name cannabis, pre-rolled joints for maybe $5 a gram, maybe $3 bucks a half gram,” said Armstrong.
“To compete with the black market in the longer term absolutely we need some of the products priced low.”
Pot is now legal in Ontario. Here’s what you need to know
Everything you need to know about legalized pot and what’s to come in Ontario
How Canada Legalized Weed
It’s one of Justin Trudeau’s few policy wins, but he doesn’t deserve all—or even much—of the credit. SHARE TWEET
Holy shit. We made it. Weed will be legal in Canada on Wednesday. Ninety years of cannabis prohibition in the garbage where it belongs. Savour this unforgettable moment—at least until you space on it ten minutes after your first legitimate draw.
Anyway, the dark ages are over now so let’s never dwell on it again. But it’s worth tipping our hats to everyone who helped make this happen. Before you take a toke on Wednesday, thank a medicinal cannabis activist, because they’re the ones who did all the legal legwork.
Cannabis was first outlawed in 1923 (largely based on racist reasoning). Although a 1972 Royal Commission recommended it be decriminalized, there was no legal thaw around its use until the turn of the 21st century. In 2000, the Ontario Court of Appeal ruled that a blanket ban on all cannabis consumption violated the constitutional rights of those who used it for medicinal purposes. Terrence Parker’s case is the thin end of the wedge that would eventually split apart cannabis prohibition in Canada. Once the federal government accepted that it would have to sanction some cannabis use (and production), full legalization was only a matter of time. (Roughly 18 years, as it turns out.)
In 2001 the federal government brought in the Marihuana for Medical Access Regulations, its first set of laws codifying legal cannabis use. This allowed licensed medicinal users to grow their own plants, or purchase flower from a licensed grower. Both Liberal prime ministers Jean Chretien and Paul Martin tried to decriminalize the possession of small amounts of cannabis, but each were thwarted: the former by pressure from the US Drug Enforcement Agency, and the latter by the 2004 federal election.
But by the mid-aughts, the political will to liberalize drug policy in Canada had vanished. In the first year of his first minority government, Stephen Harper increased criminal penalties for possession and trafficking. Anyone illegally growing dope faced up to 14 years in prison.
While going extra aggro on non-violent drug offences was near and dear to Conservative hearts, neither legal precedent nor the national zeitgeist were on their side. The 2011 R v. Mernagh decision by the Ontario Superior Court gutted federal restrictions on cannabis so thoroughly it risked legalizing cannabis production all over Ontario and possibly the whole country. The ruling was overturned in early 2013 by the Ontario Court of Appeal, but it was clear by this time that the country’s cannabis laws were untenable.
The writing was on the wall by 2012, when the Liberals picked up full cannabis legalization as a party policy. The Conservatives, meanwhile, opted to double-down: they changed medical regulations to abolish all personal production licenses and force patients to register with licensed producers. Ironically, more than just setting the Crown up for a slam-dunk legal challenge, this sowed the seeds of a commercial cannabis industry by mandating mass cannabis production.
Regulations continued to fall apart in court. A Supreme Court of Canada ruling in 2015 established that edibles, oils, and other concentrates were legitimate forms of medicinal cannabis, and thus legal to produce and possess—further bolstering and diversifying the production (and marketing) of cannabis in Canada.
By the time the Federal Court of Canada ruled in 2016 that medicinal users could grow their own supply, Justin Trudeau was prime minister and the full repeal of prohibition was already underway. But it does hammer home the point that legalization is an elegantly simple solution to this extremely stupid policy problem.
It’s difficult now to place the role legalization had during the 2015 election campaign. It wasn’t a central plank, but the promise of legal weed—along with electoral reform, deficit spending, peacekeepers, reconciliation, and a new Trudeau—helped to amplify the Liberals’ branding as the true champions of progressive Canadiana. Now it’s the twilight of Trudeau’s first term, and legal cannabis is one of the few landmark initiatives to actually be carried through. Perhaps it’s to help us cope with the about-face on everything else.
The journey of the Cannabis Act alone is another story. After a year of consultations with Canadians, in early 2017 the government brought in its first draft of weed law. (It also updated the Impaired Driving Act to vastly increase police powers to detect drugged drivers.) The Act set out the broad parameters of recreational use: anyone 18 and older can possess up to 30 grams in public, with the provinces able to tinker with that minimum legal age and whatever additional details they wanted. The whole thing sparked anticipation for a legalization date of July 1, 2018, but the Senate nearly torpedoed it at the 11th hour. The bill ultimately passed its final reading in June 2018—too late to save your Canada Day BBQ, but just in time to blow up your Halloween.
About the provinces: the feds get all the credit, but it’s the provinces doing all the heavy lifting. As a result, legal cannabis looks a little different everywhere in the country: legal age runs from 18 (Alberta) to 21 (Quebec), and in Manitoba and Quebec you won’t be able to grow your own plants. Also, in Ontario, the new Ford government spiked the old Liberal plan for a provincial monopoly less than a month out from the first day of legal sales. It will be sold in private stores, but not until sometime in April. Have fun!
So it’s been a long time coming, but here we are at last. Ironically, now that weed is legal it is likely to be policed more heavily than ever before. The cops can’t bust you just on account of holding a joint, but they can throw the book at you if try to buy in bulk or try to sell any on your own. Anyone who felt legalization should involve addressing the injustice of the drug war is justified in feeling less than euphoric about how many weed corporations are run by former prohibitionists—especially while those convicted under drug offences which no longer exist have no guarantees of amnesty.
The story isn’t over. The fight for amnesty continues, and legalization continues to unfold. Arguably the real cannabis boom is coming on October 17, 2019, when edibles are fully regulated. Beyond that, one hopes that the end of one ridiculous drug prohibition might be the begin of the end of them all. At a convention in Halifax earlier this year, Liberal membership signalled they would be interested in decriminalizing all drug use in Canada in the interests of harm reduction. The Liberal brass laughed it off—Trudeau has been emphatic that there is no interest in further changes to federal drug policy—but if the legalization of cannabis is successful it does seem to be the next logical step. North America remains mired in an opioid crisis, and Portugal has seen tremendous success in treating drug abuse as a social and medical problem instead of a criminal one. The prohibitions around medical use of other psychedelic drugs are also finally thawing; the therapeutic use of MDMA, LSD, ketamine, and psilocybin mushrooms may yet herald a revolution in psychiatry. This doesn’t mean we will ever see a day when the government is sanctioning a full-scale acid production and retail industry, but it does mean, God willing, we will someday soon reach a point where all drug war is relegated to a museum along with old film reels of Reefer Madness.
A more humane way to live together isn’t hard to imagine. All the easier, now, with a little bit of grass.
Follow Drew Brown on Twitter.
